|
The Radiotherapy market plays a vital role in the global fight against cancer, and understanding its landscape is essential for healthcare providers, researchers, and investors alike. An in-depth analysis of the radiotherapy market reveals key trends, challenges, and opportunities that shape its dynamics. One significant trend in the radiotherapy market is the increasing adoption of intensity-modulated radiation therapy (IMRT) and stereotactic radiosurgery (SRS). IMRT allows for precise radiation dose delivery, while SRS enables high-dose radiation in a few sessions, often used for the treatment of brain tumors and small lesions. The demand for these advanced techniques is driven by their ability to improve treatment outcomes and reduce treatment duration. Another important aspect of the Radiotherapy Market is the evolving regulatory landscape. Regulatory bodies worldwide are continually updating guidelines and standards for radiation therapy equipment and procedures. Compliance with these regulations is crucial for market participants to ensure patient safety and quality of care. Moreover, reimbursement policies and insurance coverage greatly influence the adoption and utilization of radiotherapy technologies. Challenges faced by the radiotherapy market include high treatment costs, limited access to advanced technologies in developing regions, and the need for skilled healthcare professionals. Addressing these challenges requires collaborative efforts from healthcare providers, industry stakeholders, and policymakers to promote affordability, accessibility, and training programs. Opportunities in the radiotherapy market arise from the integration of novel technologies such as proton therapy, AI, and molecular imaging. Proton therapy offers a unique treatment modality, while AI enables intelligent decision support systems for treatment planning and personalized medicine. Molecular imaging techniques, such as PET and MRI, provide valuable information for precise tumor targeting. A comprehensive analysis of the radiotherapy market reveals a dynamic landscape shaped by trends, regulations, challenges, and opportunities. By staying abreast of these factors, stakeholders can navigate the market effectively, drive innovation, and ultimately contribute to improving patient outcomes in the fight against cancer. The radiotherapy market is experiencing transformative innovations that hold immense potential for improving cancer treatment outcomes. With advancements in imaging technologies, proton therapy, and AI integration, the future of radiotherapy is promising, offering more precise and personalized treatment options for patients. Read More- https://cmi-latestreportorientedblogs.blogspot.com/2023/07/the-increasing-burden-of-cancer-in.html
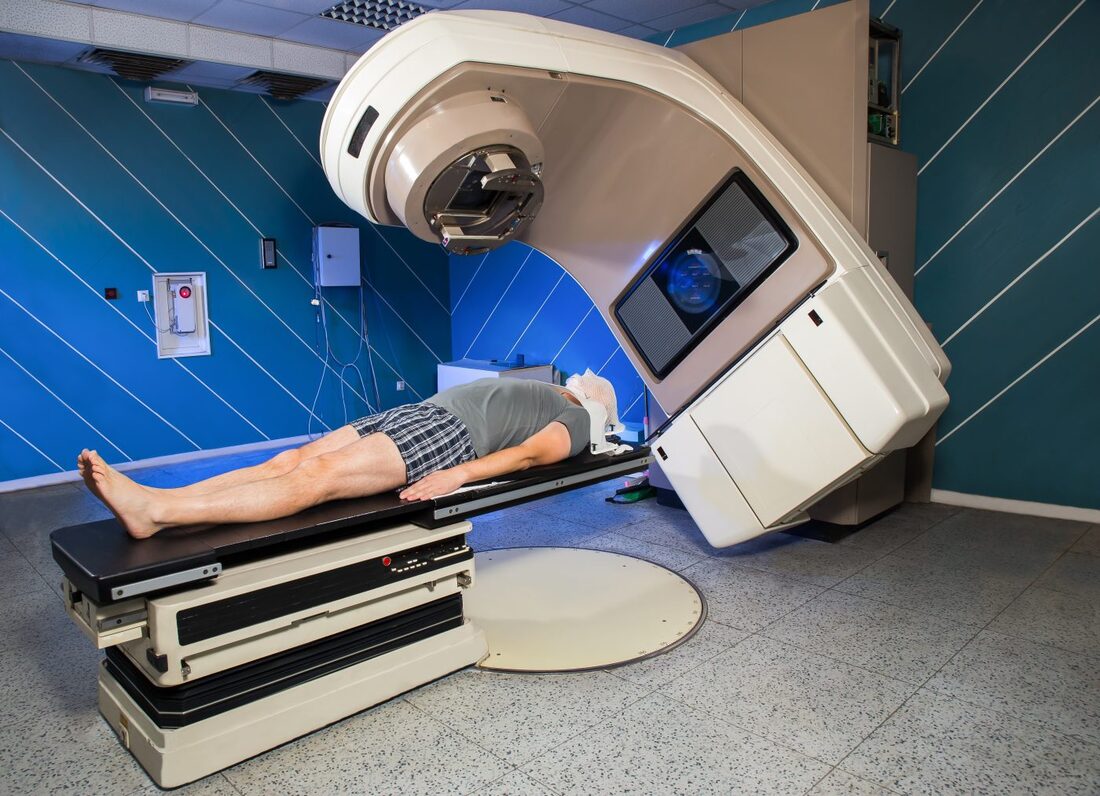
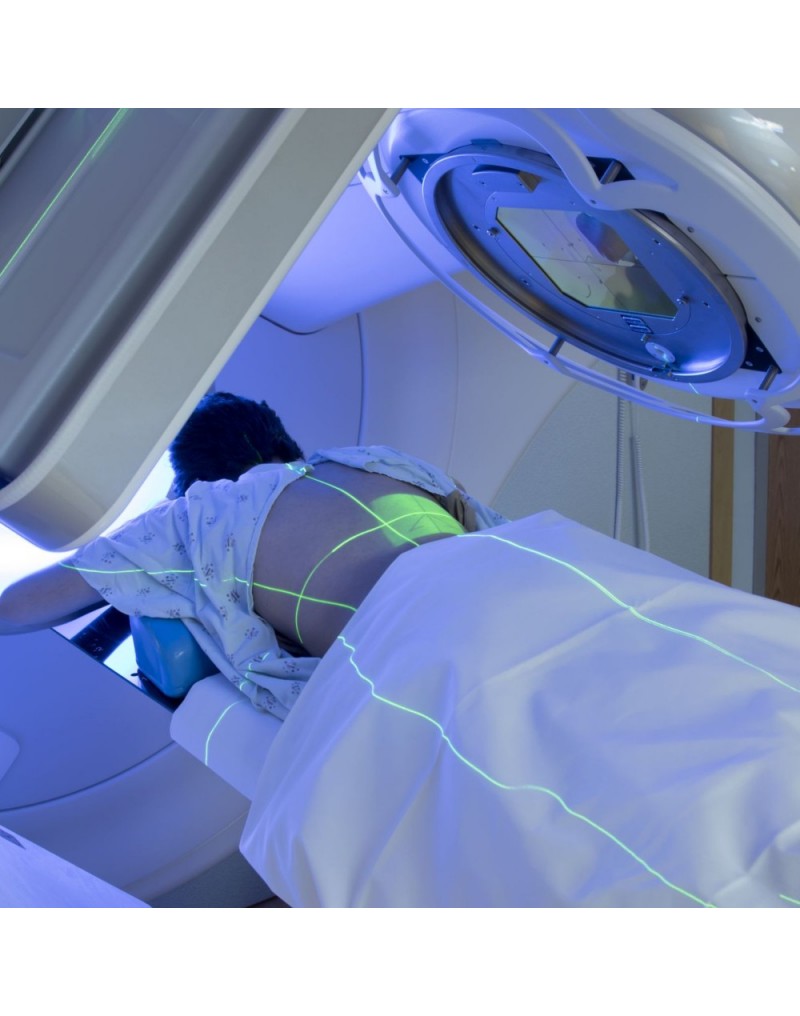
0 Comments
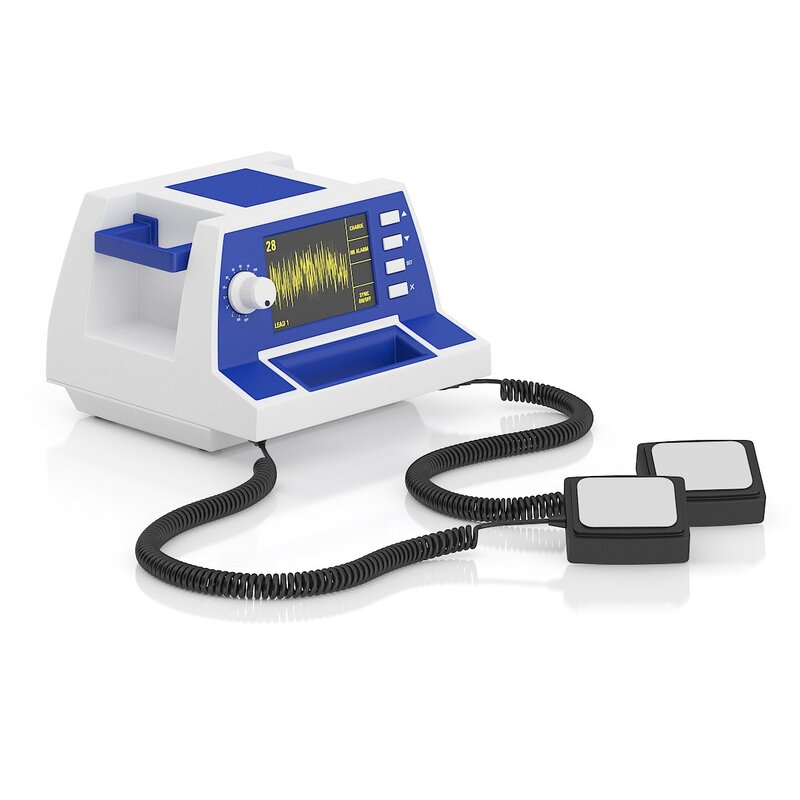
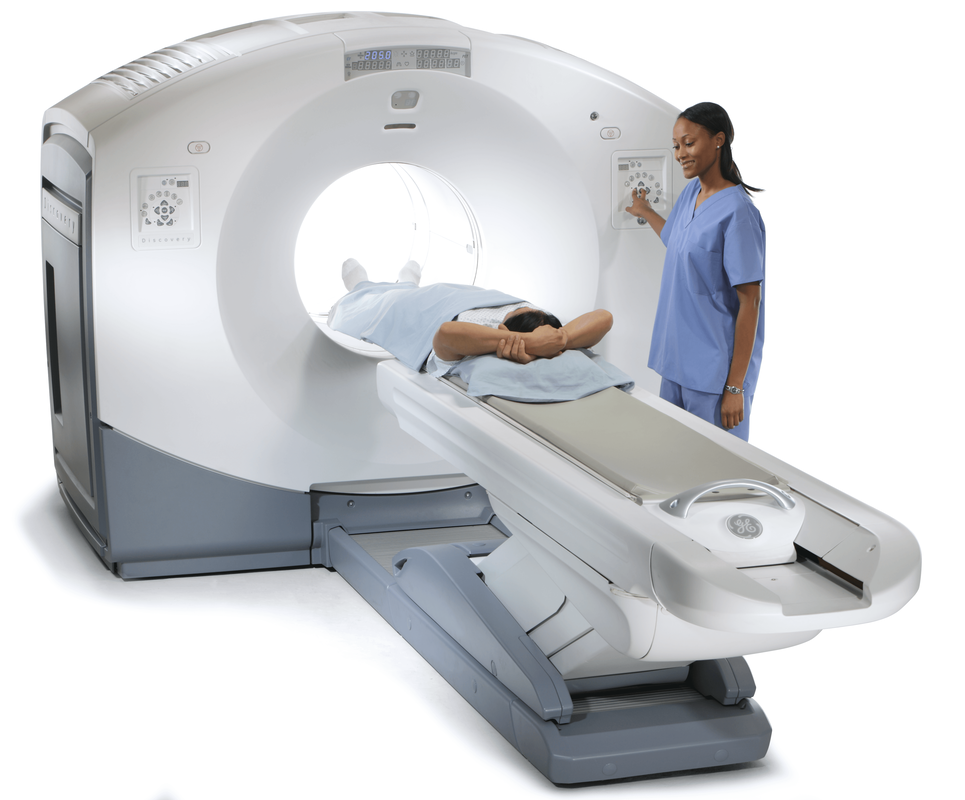
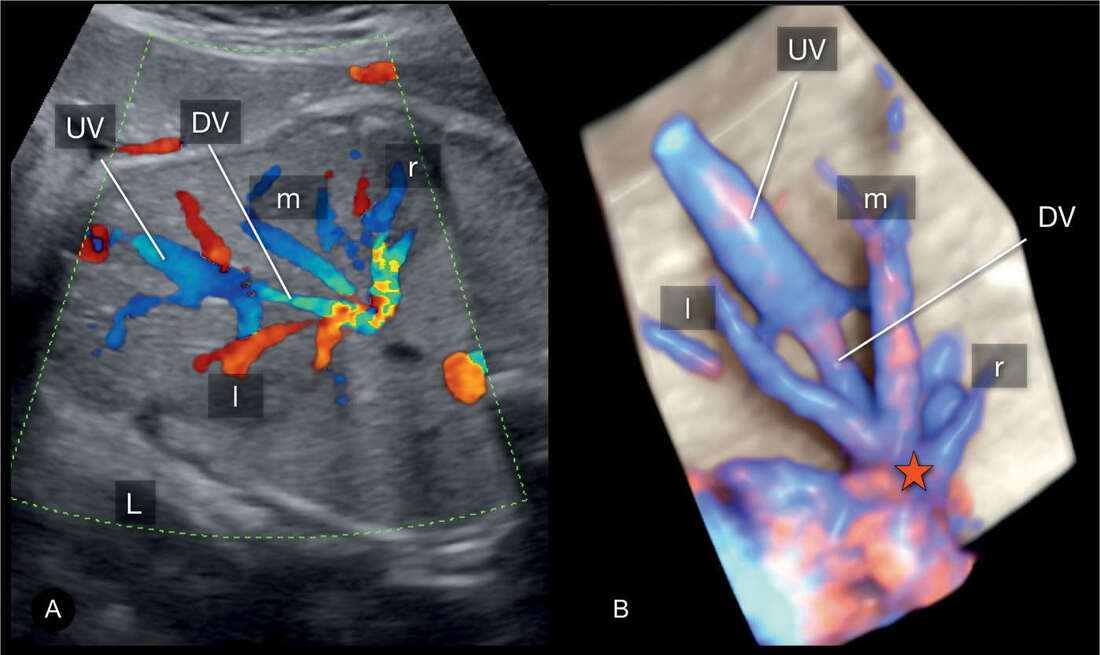
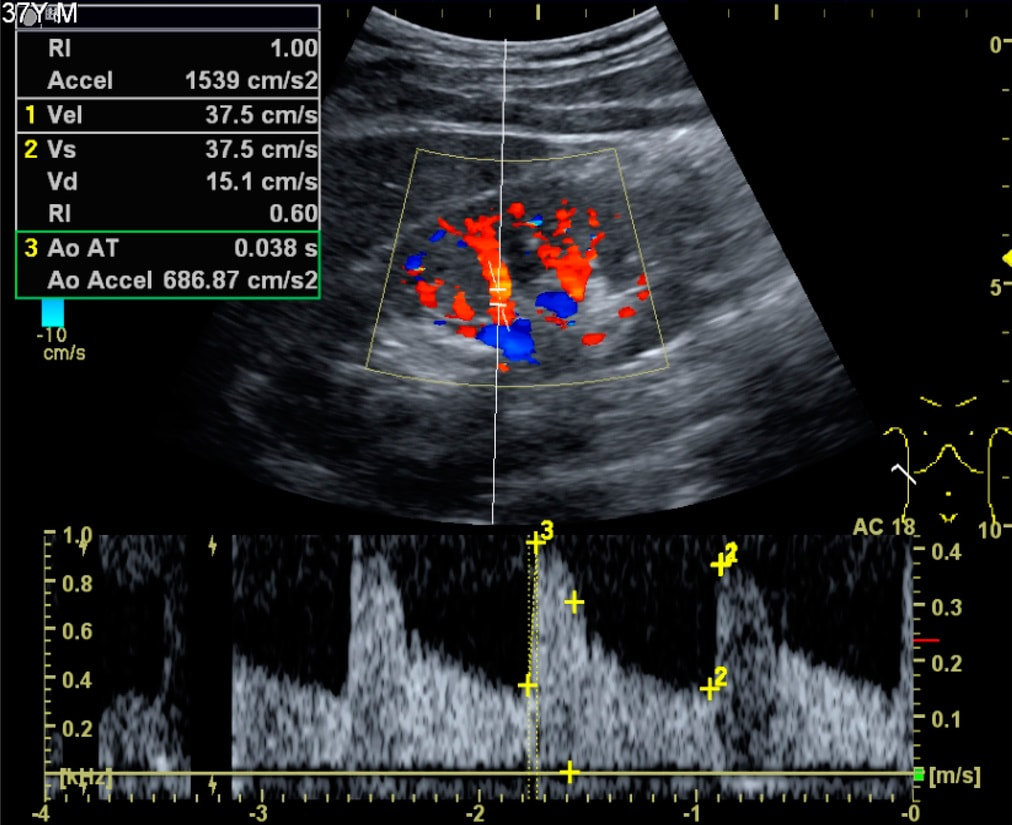
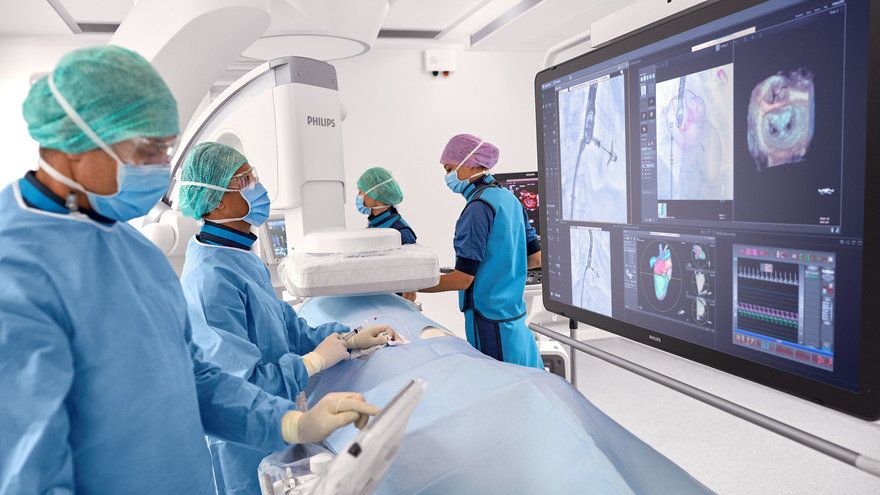
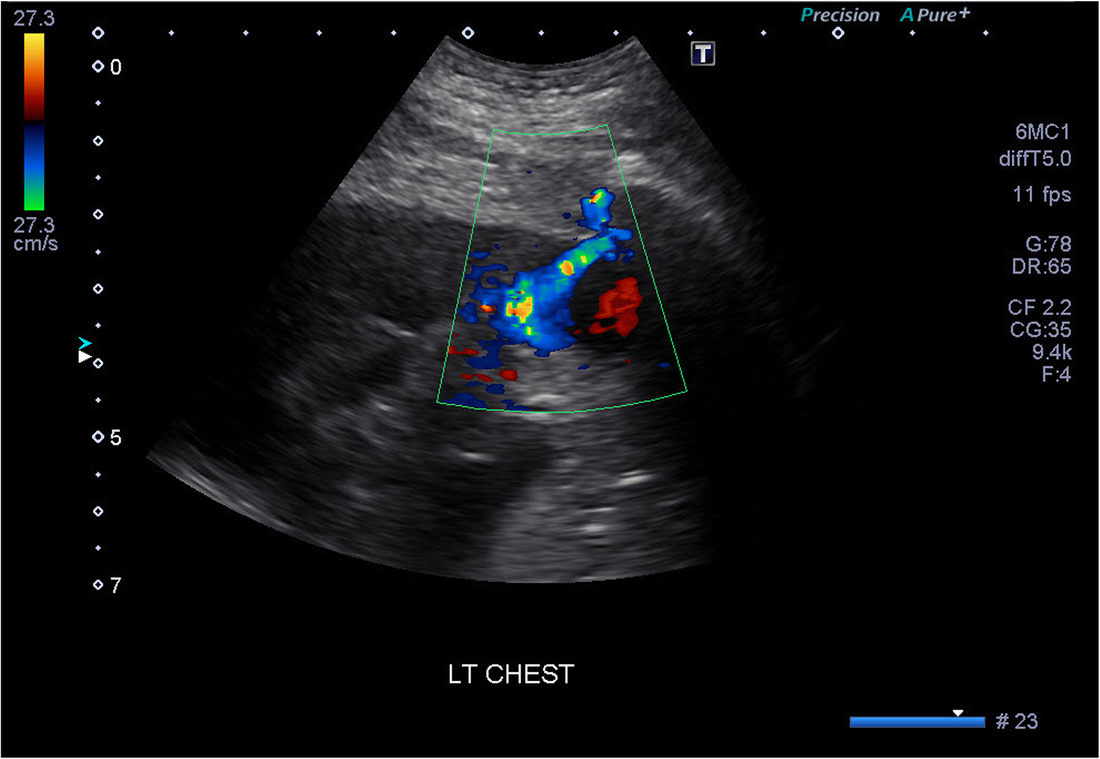
Radiotherapy, also known as radiation therapy, is a cornerstone in the field of oncology, offering a potent tool in the fight against cancer. By utilizing high-energy radiation, radiotherapy targets and destroys cancer cells, offering hope and improved outcomes for patients worldwide. At its core, Radiotherapy involves the controlled use of ionizing radiation to damage or destroy cancer cells while minimizing harm to surrounding healthy tissue. Ionizing radiation consists of high-energy particles or waves capable of penetrating matter and causing biological changes within cells. The goal of radiotherapy is to deliver a precise and optimal dose of radiation to the tumor, impairing its ability to grow and divide or eradicate cancer cells altogether. Multiple techniques and approaches are employed in radiotherapy, tailored to individual patients and their specific cancer types. External beam radiation therapy is one of the most common techniques, where radiation is generated from an external source, such as a linear accelerator, and directed at the tumor from outside the body. This approach allows for precise targeting while sparing surrounding healthy tissues. Internal radiation therapy, also known as brachytherapy, involves the placement of radioactive sources directly into or near the tumor. This technique allows for a highly concentrated dose of radiation to be delivered to the tumor site, minimizing exposure to healthy tissues. Brachytherapy, also known as internal radiation therapy, is a specialized form of radiotherapy that involves the placement of radioactive sources directly into or near the tumor or the area requiring treatment. Unlike external beam radiation therapy, where radiation is delivered from an external machine, brachytherapy delivers a high dose of radiation directly to the targeted site, sparing surrounding healthy tissues. Stereotactic radiosurgery and stereotactic body radiation therapy (SBRT) are specialized techniques that deliver high doses of radiation with extreme precision, typically used for small tumors or in cases where surgery is not feasible. These techniques rely on advanced imaging technology and computer-guided systems to accurately target the tumor while minimizing damage to surrounding structures. Radiotherapy serves various purposes throughout the cancer treatment journey. It can be used as a primary treatment modality, aiming to cure cancer by eradicating tumors entirely. It may also be employed as an adjuvant treatment after surgery or in combination with chemotherapy to destroy remaining cancer cells or reduce the risk of recurrence. Additionally, radiotherapy can be used as a palliative treatment to alleviate symptoms and improve quality of life in cases where cancer cannot be cured. By targeting tumors that cause pain, obstruction, or other distressing symptoms, Radiotherapy can provide significant relief and improve overall well-being. Advancements in technology have revolutionized the field of radiotherapy, enabling more precise and effective treatment delivery. Image-guided radiotherapy (IGRT) combines real-time imaging, such as computed tomography (CT) scans or magnetic resonance imaging (MRI), with radiotherapy planning and delivery systems. This allows for accurate tumor visualization and alignment, ensuring radiation is precisely delivered to the intended target while minimizing exposure to healthy tissues. Intensity-modulated radiation therapy (IMRT) and volumetric-modulated arc therapy (VMAT) are advanced techniques that allow for the delivery of highly conformal doses of radiation. By adjusting the intensity and shape of the radiation beams, these techniques sculpt the radiation dose to conform to complex tumor shapes, sparing critical structures nearby. Proton therapy is another cutting-edge approach that utilizes protons, rather than photons, to deliver radiation. Proton beams have unique properties that enable precise targeting and greater sparing of healthy tissues compared to conventional radiation. While Radiotherapy continues to be a powerful treatment modality, challenges remain. Access to radiotherapy services is limited in some regions, particularly in low-resource settings. Additionally, there is a need for ongoing research to optimize treatment protocols, minimize side effects, and explore the potential combination of radiotherapy with other therapies, such as immunotherapy or targeted therapy. Radiotherapy is a vital component in the management of brain tumors. It is a treatment modality that utilizes high-energy radiation to target and destroy tumor cells while minimizing damage to healthy brain tissue. Brain tumors can be classified as either primary or secondary. Primary brain tumors originate within the brain, while secondary tumors, also known as metastatic tumors, spread to the brain from other parts of the body. Regardless of the tumor type, radiotherapy can be used as a primary treatment, adjuvant therapy after surgery, or palliative treatment to alleviate symptoms and improve the patient's quality of life. The primary goal of Radiotherapy for brain tumors is to deliver a precise and effective dose of radiation to the tumor site while sparing surrounding healthy brain tissue. To achieve this, a comprehensive treatment plan is developed based on various factors, such as the tumor's location, size, grade, and the patient's overall health condition. The first step in radiotherapy for brain tumors is treatment planning. This involves imaging techniques such as magnetic resonance imaging (MRI), computed tomography (CT), and positron emission tomography (PET) scans to precisely locate the tumor and determine its size and shape. Advanced imaging technologies, such as functional MRI and diffusion tensor imaging, can provide additional information about the tumor's proximity to critical brain structures and help in devising optimal treatment strategies. Once the tumor has been accurately delineated, the radiation oncologist, in collaboration with a team of medical physicists and dosimetrists, develops a treatment plan that defines the radiation dose, treatment schedule, and the angles from which radiation beams will be delivered. The aim is to deliver a high dose of radiation to the tumor while minimizing exposure to healthy tissues. There are several Radiotherapy techniques used for brain tumors. Conformal radiotherapy (CRT) uses three-dimensional imaging to shape radiation beams to the precise dimensions of the tumor, thus reducing radiation exposure to surrounding healthy tissue. Intensity-modulated radiation therapy (IMRT) takes it a step further by using computer-controlled linear accelerators to deliver radiation beams of varying intensity, sculpting the dose distribution to conform to complex tumor shapes. Stereotactic radiosurgery (SRS), on the other hand, delivers a highly focused, single high-dose radiation treatment to the tumor using multiple intersecting beams. This technique is particularly effective for smaller tumors or those in delicate locations. During Radiotherapy sessions, patients are carefully positioned using immobilization devices to ensure reproducibility and accuracy. Radiation is typically delivered in daily fractions over several weeks to allow healthy tissues to repair while continuously damaging tumor cells. The total duration and number of sessions depend on various factors,including the tumor type, location, and the patient's overall health. Although radiotherapy is a targeted treatment, it can still affect surrounding healthy brain tissue. Common acute side effects may include fatigue, scalp irritation, temporary hair loss, and mild skin reactions. Depending on the tumor's location, there may be specific side effects such as temporary worsening of symptoms, headaches, nausea, or cognitive changes. However, these side effects are generally temporary and resolve after completion of treatment. A chitin derivative called chitosan is taken out of the shells of aquatic animals like lobsters, prawns and crabs. Due to its ability to prevent fat absorption in the gastrointestinal tract, Chitosan is a common ingredient in dietary supplements. Due to its biodegradability and biocompatibility, it is also utilised in a number of therapeutic applications. Due to its anticoagulant characteristics, it is utilised in hemostatic dressing to treat wounds. Long-term side effects of brain Radiotherapy are rare but can include radiation necrosis, which is the death of normal brain tissue due to radiation exposure. Advances in radiotherapy techniques, such as the use of proton therapy and stereotactic radiosurgery, have helped minimize the risk of long-term side effects by precisely targeting the tumor and sparing healthy tissue. Radiotherapy, also known as radiation therapy, is a type of cancer therapeutic, which uses high-energy radiation for treatments. The radiation can come from a machine outside the body (external beam radiotherapy) or from a radioactive source placed inside the body near the cancer cells (brachytherapy). Radiotherapy can be used alone or in combination with other cancer treatments, such as surgery and chemotherapy. Cancer is a disease that has claimed many lives worldwide. Despite medical advancements, it remains a significant threat to human life. However, the use of radiation therapy or radiotherapy has significantly improved cancer treatment. Radiotherapy uses high-energy radiation to kill cancer cells and shrink tumors. Radiotherapy works by attacking the DNA inside cancer cells, making it difficult for them to divide and grow. Healthy cells can also be affected by radiation, but they are usually better able to repair the damage than cancer cells. The goal of radiotherapy is to kill as many cancer cells as possible while minimizing damage to healthy cells. External beam radiotherapy (EBRT) is the most common type of radiotherapy. It involves the use of a machine called a linear accelerator to deliver high-energy radiation beams to the cancerous area. The radiation beams are carefully aimed at the cancerous area to avoid damaging nearby healthy tissue. Brachytherapy, also known as internal radiotherapy, involves the insertion of a radioactive source directly into or near the cancerous area. The radiation source can be temporary or permanent. The radiation from the source is delivered directly to the cancer cells, minimizing damage to nearby healthy tissue. Stereotactic Body Radiotherapy (SBRT) is a highly precise form of radiotherapy that uses advanced imaging techniques to deliver high doses of radiation to a specific area of the body. It is commonly used to treat small, early-stage tumors in the lung, liver, and prostate. Proton therapy is a type of external beam radiotherapy that uses protons instead of photons to deliver radiation to the cancerous area. Protons are able to deliver a higher dose of radiation to the tumor while minimizing damage to surrounding healthy tissue. Radiotherapy is used to treat a wide variety of cancers. Radiotherapy is commonly used in the treatment of breast cancer. It is often used after surgery to kill any remaining cancer cells and reduce the risk of recurrence. It can be used alone or in combination with other cancer treatments to treat lung cancer. It is commonly used to treat small, early-stage tumors. Radiotherapy is commonly used in the treatment of prostate cancer. It can be used alone or in combination with other cancer treatments, such as hormone therapy. It is often used in the treatment of head and neck cancer. It can be used alone or in combination with other cancer treatments, such as surgery and chemotherapy. Radiotherapy is commonly used in the treatment of gynecologic cancers, such as cervical and endometrial cancer. It can be used alone or in combination with other cancer treatments. Like all cancer treatments, radiotherapy can cause side effects. The side effects of radiotherapy depend on the type and location of the cancer being treated, as well as the radiation dose and the patient's overall health. Common side effects of Radiotherapy include, fatigue is a common side effect of radiotherapy, especially during the later weeks of treatment. The fatigue can range from mild to severe and can affect daily activities. Radiotherapy can cause skin changes, such as redness, itching, dryness, and peeling, in the area being treated. The severity of the skin changes depends on the radiation dose and the location of the cancer. Radiotherapy to the abdomen or pelvis can cause nausea and vomiting. Medications can help relieve these symptoms. Radiotherapy to the head can cause hair loss in the treated area. Radiotherapy to the arms or legs can cause swelling, called lymphedema. This swelling can be managed with compression garments and exercise. Long-term side effects of radiotherapy are rare, but they can occur. These side effects can include secondary cancers, damage to organs and tissues in the treated area, and infertility. Get Free Press Release of Radiotherapy Market By Sending Controlled Electric Pulses To The Heart, Defibrillators Restore Normal Heartbeats22/5/2023 In the realm of emergency medical care, few devices are as crucial and life-saving as Defibrillators. These remarkable machines play a vital role in the resuscitation of individuals experiencing sudden cardiac arrest (SCA), a condition characterized by the abrupt loss of heart function. Defibrillators are designed to deliver an electric shock to the heart, restoring its normal rhythm and potentially saving a person's life. In this article, we will explore the fundamental aspects of defibrillators and delve into their essential role in emergency medical situations. To understand the significance of Defibrillators, it's important to grasp the nature of sudden cardiac arrest. SCA occurs when the heart's electrical system malfunctions, causing the heart to beat irregularly or stop altogether. Within seconds, the lack of blood flow to vital organs, including the brain, can result in unconsciousness, brain damage, or even death. In such critical moments, prompt intervention is paramount, and this is where defibrillators come into play. Defibrillators work by administering an electric shock to the heart, which depolarizes the myocardial cells and allows the heart's natural pacemaker to reestablish its normal rhythm. The electric shock delivered by the defibrillator essentially resets the heart, enabling it to resume its essential pumping function. This process is known as defibrillation and is typically accompanied by cardiopulmonary resuscitation (CPR) to maximize the chances of successful resuscitation. There are two primary types of Defibrillators: automated external defibrillators (AEDs) and implantable cardioverter-defibrillators (ICDs). AEDs are portable devices commonly found in public places, such as airports, schools, and shopping malls. They are designed to be user-friendly and can be operated by individuals with minimal or no medical training. AEDs analyze the heart's rhythm and, if necessary, deliver an electric shock to restore normal heart function. These devices often provide step-by-step voice instructions to guide users through the resuscitation process, making them invaluable in emergencies where immediate medical help may not be available. On the other hand, ICDs are implantable devices that are surgically placed in patients at high risk of SCA. These sophisticated devices continuously monitor the heart's rhythm and can deliver an electric shock if an abnormal rhythm is detected. ICDs are commonly recommended for individuals with a history of heart disease, heart attacks, or other cardiac conditions that increase the likelihood of SCA. By constantly monitoring the heart's activity, ICDs provide a proactive approach to preventing sudden cardiac death and offer reassurance to patients who are at high risk. The importance of Defibrillators lies in their ability to swiftly intervene during a cardiac emergency. Time is of the essence when dealing with SCA, as every passing minute reduces the chances of survival. Research has shown that early defibrillation, within the first few minutes of cardiac arrest, significantly improves the likelihood of successful resuscitation. In fact, the American Heart Association emphasizes the importance of starting CPR and using an AED as soon as possible to improve the chances of survival. Public access to Defibrillators is crucial for maximizing their life-saving potential. This realization has led to the installation of AEDs in various public spaces, creating a more heart-safe environment. Many countries have implemented public-access defibrillation programs, equipping community centers, sports facilities, and other high-traffic areas with AEDs. These programs aim to empower bystanders to take immediate action in case of cardiac emergencies, enabling them to provide critical aid until professional medical help arrives. Positron Emission Tomography (PET) Scanners employ radioactive tracers to exhibit the way body's tissues function. They are a strong analytical device that can aid identify tumor, cardiovascular disorders, and several neurological diseases, such as dementia. A small quantity of a radioactive tracer, known as a radiotracer, is inoculated into the plasma. The tracer is further engrossed by the body and essences in cells and other body parts. The traces assemble in the cells of cancer and other tissues that are utilizing more glucose compared to healthy cells. These regions will be glare on the Positron Emission Tomography (PET) Scanners picture compared to common cells and are indicated as hot spots. Positron Emission Tomography (PET) Scanners can be utilized to cure specific diseases and observe the development of treatment. They can further be utilized to measure and plan some operations, such as cardiac surgery or brain operation for epilepsy. One can prepare for a Positron Emission Tomography (PET) Scanners by consuming the common medications and supplements. One should also allow the physician and the nuclear medication staff know if one is expecting or breastfeeding. The physician will instruct one to lie on a positioning table that moves slowly from a donut-shaped hovel in the middle of a specific machine. The scanner rings of sensors observe the energy liberated from the radioactive tracers in the body and change them into 3D computing pictures. Positron Emission Tomography (PET) Scanners can give physicians essential early data regarding cardiovascular disorders and several neurological diseases, such as dementia. They can also aid identify tumor, to reduce patients costly and painful diagnostic procedures. The scan includes a small sum of radioactive substances known as a radiotracer being inoculated into the vein or breathed in as gas. This radiotracer is further engrossed by specific organs and cells, producing an accumulation of energy known as positrons which is identified by a Positron Emission Tomography (PET) Scanners or probe. Prior the scan, one will be offered a dosage of the radiotracer and suggested to consume adequate amount of water. One should also stop eating and consumption of alcohol for 6 hours prior the test. One will further be fixed on a flat bed and transformed into the center of a huge, circular scanner. One should stay stable when the scanner captures the image of the body, which generally takes around half an hour. Positron Emission Tomography (PET) Scanners is a painless operation, apart for a mild skin problem. Some individuals feel a sense of pressure as the radiotracer is inoculated into the plasma, however this goes away post an hour. Positron Emission Tomography (PET) Scanners are utilized to measure the efficiency of chemotherapy and other procedures for tumor, and to check the advancement of therapy post operation. They can also aid to detect whether a cancer has spread and whether it required more therapeutics, particularly in brain tumor and colorectal tumor. They can further be utilized to assess neurological problems, such as epilepsy. A Doppler Ultrasound is a non-invasive test used to estimate the blood flow through blood vessels by bouncing high-frequency sound waves (ultrasound) off circulating red blood cells. The regular ultrasound uses sound waves to produce images, but can't show the blood flow. Doppler ultrasound uses sound waves to detect the movement of blood in vessels. It is a noninvasive, safe, and painless way for healthcare providers to assess the health of blood vessels and check for the cardiovascular problem. A normal result means the blood vessels show no signs of narrowing, clots, or closure, and the arteries have normal blood flow. Doppler Ultrasound is a diagnostic test that uses sound waves to measure the speed of blood flow in the body. It is a noninvasive test that can detect problems with the heart and arteries, as well as check if there are clots in veins. It is also helpful for determining if there are any abnormalities in the blood flow to the brain, including after a stroke. It is an imaging procedure that uses high-frequency sound waves to view the flow of blood within a vessel. It is a noninvasive and painless test that does not use radiation. It can be used to detect many different medical problems, such as heart diseases, vascular disease, and kidney disorders. It is especially effective for examining arteries and veins that may not show up on regular X-rays or ultrasounds. It is used in pregnancy to study blood circulation in the baby, uterus and placenta. Using it in high‐risk pregnancies, where there is concern about baby's condition, shows benefits. During pregnancy, Doppler Ultrasound is often used to check if the baby’s blood flows properly in the uterus and placenta. This can help diagnose and prevent health issues that could harm an unborn child or cause birth defects. The test is performed by a doctor or radiologist who is specially trained in using Doppler ultrasound technology. The technician places clear water-based gel on the body part being examined to improve the quality of the sound waves. They then place the transducer on the skin in various locations, sweeping over the area of concern to get the best results. A Doppler ultrasound can help the doctor examine any blocked or narrowed arteries, which could lead to serious complications if left untreated. It can also be used to find a blood clot in lungs or legs, which is often called deep vein thrombosis (DVT). Doppler ultrasound is a safe, painless, and noninvasive test that doesn’t involve ionizing radiation. It can be done on people of all ages, including pregnant women. The test uses ultrasound to look at the blood flow in the large arteries and veins in the arms or legs. Doppler ultrasonography examines the blood flow in the major arteries and veins in the arms and legs with the use of ultrasound. Doppler Ultrasound uses sound waves to produce images of blood moving through the circulatory system. It is an imaging test that uses sound waves to show blood moving through blood vessels. It is a quick, painless way to check for problems with blood flow. This information can help healthcare provider screen for diseases, diagnose a problem and evaluate the effectiveness of treatments. Doppler Ultrasound is a medical imaging technique that is commonly used to evaluate the flow of blood in various parts of the body. It is named after Christian Doppler, an Austrian physicist who first described the principle of the Doppler effect in 1842. The Doppler effect is a phenomenon that occurs when there is a relative motion between a wave source and an observer, resulting in a change in the frequency or wavelength of the wave. In the case of ultrasound, this effect is used to determine the speed and direction of blood flow in the body. Doppler Ultrasound works by emitting high-frequency sound waves (usually between 2 and 20 MHz) into the body using a transducer. This transducer is a handheld device that is placed on the skin over the area of interest. As the sound waves pass through the body, they bounce off the tissues and blood cells and return to the transducer. The transducer then converts these echoes into electrical signals, which are processed by a computer to produce a visual representation of the blood flow. There are two main types of Doppler Ultrasound: pulsed-wave Doppler and continuous-wave Doppler. Pulsed-wave Doppler uses short bursts of sound waves to measure blood flow at specific points in the body. This type of Doppler ultrasound is commonly used to evaluate blood flow in the heart, arteries, and veins. Continuous-wave Doppler, on the other hand, uses a continuous stream of sound waves to measure blood flow throughout an entire vessel. This type of Doppler ultrasound is often used to evaluate blood flow in the brain. Doppler Ultrasound is commonly used in a variety of medical applications. One of the most common uses is in the evaluation of the heart and blood vessels. It can be used to diagnose a wide range of cardiovascular conditions, such as blood clots, atherosclerosis, and heart valve problems. It can also be used to evaluate the effectiveness of treatments such as angioplasty or stenting. Doppler Ultrasound is also commonly used in obstetrics to monitor fetal growth and development. It can be used to evaluate blood flow in the umbilical cord and placenta, and to detect abnormalities such as fetal distress or growth restriction. Doppler ultrasound can also be used during pregnancy to monitor the blood flow in the mother's uterus and detect conditions such as placental abruption or pre-eclampsia. In addition to its use in cardiovascular and obstetric applications, Doppler Ultrasound is also used in a variety of other medical fields. It can be used to evaluate blood flow in the liver, kidneys, and other organs, and to diagnose conditions such as liver cirrhosis or kidney disease. It can also be used to evaluate blood flow in tumors, and to monitor the effectiveness of cancer treatments such as chemotherapy. One of the major advantages of Doppler ultrasound is its non-invasive nature. Unlike other imaging techniques such as angiography or CT scans, Doppler ultrasound does not require the use of contrast agents or radiation, making it a safer and more cost-effective option for many patients. Doppler ultrasound is also relatively quick and easy to perform, and can be done in a clinic or doctor's office. However, there are some limitations to Doppler Ultrasound. One of the main limitations is that it can be difficult to obtain accurate measurements in certain situations. For example, it may be difficult to measure blood flow in very small vessels or in areas of the body that are difficult to access. Additionally, Doppler ultrasound may not be able to provide a detailed image of the structures within the body, and may not be able to detect certain types of abnormalities. Image Guided Therapy (IGT) is a revolutionary treatment for several types of cancers, as well as other complex disorders. It is also used to treat patients with chronic obstructive pulmonary disease (COPD). Moreover, a new system called Image Guided Surgery is used to perform surgical procedures in patients with advanced heart disease. With the help of these systems, surgeons can effectively perform complex surgeries without the risk of causing unnecessary damage. Image Guided Therapy is a form of radiation therapy that uses imaging techniques during the treatment process. This treatment has a lower impact on healthy tissue than standard radiotherapy. However, there are some risks and complications. A computer creates a picture of the tumor and the surrounding tissue. The image is compared to a simulation of the tumor and the image is adjusted to ensure more accurate and targeted radiation delivery. Compared to standard RT, image guidance can lead to more precise dose deposition and less systemic side effects. Image Guided Therapy is generally used for patients with lung or brain tumors. The benefits include frameless radiosurgery of these tumors. The safety margin can be narrowed and the risk of injury to nearby healthy tissues can be minimized. Image Guided Therapy may also be referred to as functional or molecular imaging. PET and molecular imaging are important for improving diagnostic accuracy. Chronic obstructive pulmonary disease (COPD) is caused by exposure to air pollution and inhaled toxins. The disease is also associated with an abnormal inflammatory response of the lungs. Although it does not have a cure, treatment can help reduce the symptoms of the disease. Oxygen therapy is often used to treat COPD. A machine with a mask is placed over the nose and mouth to help the patient breathe. Corticosteroids are also given, sometimes inhalers are also used. However, early treatment can be very beneficial. By diagnosing the disease at an earlier stage, patients can be more effectively treated, which can help slow the progression of the disease and lower the risk of relapses. Exercise is another important part of pulmonary rehabilitation. Regular exercise can help patients reduce shortness of breath, improve physical functioning, and improve their quality of life. An Image Guided Therapy System for treatment of other complex disorders is an all-encompassing term used to describe medical technologies that are designed to assist doctors in the diagnosis and management of a wide variety of diseases. This includes imaging systems, angiography devices and surgical navigation equipment. Several types of image-guided therapy systems are available nowadays. Some of the most common include MRI, ultrasound and CT scan. The technology is aided by the use of integration software, which allows the physicians to use the images for more than just diagnostics. With a geriatric population on the rise, image-guided therapy systems are poised to provide relief to a growing number of patients. Many companies, along with a host of startups and smaller entrants, are making big waves in the medical arena. Image Guided Therapy systems can make surgery and other medical operations less invasive and provide better patient outcomes. However, image-guided therapy systems also face challenges such as cost, preparation time, and regulations. The technology behind image-guided therapy is expected to help in the treatment of complex diseases. It is also used to improve care quality and reduce mortality rates. These technologies can be applied in imaging, surgical navigation, and ultrasound. Doppler Ultrasound has applications in the medical field. These applications include detection of blood clots in the brain, and treatment of blood clots in the arteries. It has also been found to be helpful in the diagnosis of blood clots in the heart. Doppler Ultrasound is a non-invasive diagnostic test that can help determine the speed and direction of blood flow in the heart. The results are helpful in detecting a number of conditions, such as narrowed arteries and blockages. The test takes thirty minutes or less. Doppler ultrasound uses high-frequency sound waves to send and receive information about the vascular system. These waves are then used to produce images of the circulatory system. During the test, a technician presses a small hand-held device against the skin. This allows the technician to see images of the blood vessels. Depending on the situation, the technician may also need to place pressure on a vein to see if there is a clot. Ultrasound is typically performed in the hospital or in a medical facility. However, there are portable ultrasound machines that can be used to check the severity of blood vessel damage or disease. A Doppler Ultrasound exam usually takes less than an hour. A technician will apply gel to the skin and then press a small device called a transducer against the area. The sound waves bounce off the blood cells and form an image of the artery. Blood flow in the brain can be affected by a number of problems. In particular, the size of the vessels and the change in the shape of the cells can alter the flow of oxygen and blood to the brain. There is a higher risk of stroke. This condition is most commonly caused by tiny blood clots in the brain. Acute ischemic stroke occurs when a blood clot blocks oxygen-rich blood from reaching the brain. Doppler Ultrasound allows surgeons to view the vessels in and around the brain. It can detect blood flow and can also help to detect problems such as heart defects. A radiologist interprets the speed and direction of the flow. The goal of these tests is to detect blockages and abnormalities that affect the blood vessels. They can also diagnose conditions such as strokes. Blood can leak into the surrounding cerebrospinal fluid and destroy nearby brain cells. During an ischemic stroke, a blood clot forms in a blood vessel and cuts off blood flow to the brain. This can result in brain damage and paralysis. The clot can be carried to the brain and cause vasospasm. Doppler Ultrasound is a procedure used to check for blood flow problems. It is a painless test that can be done in the doctor's office, hospital, or other medical facility. The results of the test are immediately available to the doctor, which is important for diagnosis and treatment. The test can be used to detect clots in the heart, brain, or legs. If a clot is found, it can lead to dangerous complications. Some of the symptoms of blood clots are chest pain, shortness of breath, slurred speech, and vision impairment. A venous clot can cause swelling, warmth, and tenderness. Other symptoms may include pain, difficulty breathing, or bruising. This condition can develop slowly over time. Blood clots can be life-threatening, depending on where they occur. They can also mimic other health conditions. Arterial clots, can cause intense pain and result in a heart attack. |
Categories
All
|