|
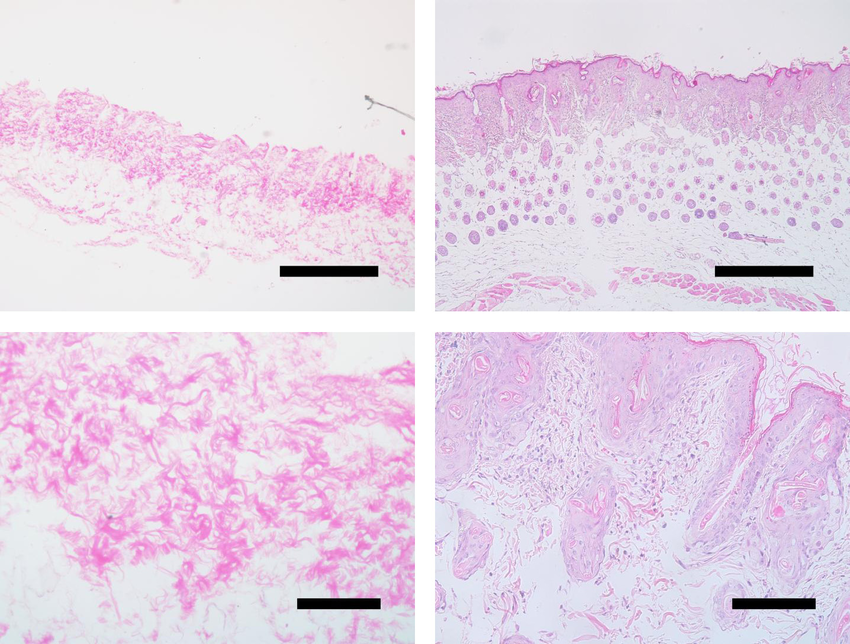
Skin grafting is a crucial procedure used in reconstructive and plastic surgery to repair and restore damaged skin. Traditionally, autologous skin grafts have been the gold standard, but they have limitations such as donor site morbidity and limited availability. However, recent advancements in medical technology have introduced Acellular Dermal Matrices as a promising alternative for skin grafting. ADMs are derived from human or animal sources and offer numerous advantages, including reduced donor site morbidity, improved cosmetic outcomes, and enhanced tissue integration. This article explores the potential of ADMs as the future of skin grafting and their impact on the field of regenerative medicine. Acellular Dermal Matrices are biologically derived scaffolds that serve as a framework for tissue regeneration. They are created by processing human or animal skin, removing cells, and retaining the extracellular matrix (ECM) components. The ECM consists of proteins, growth factors, and other bioactive molecules that facilitate cell migration, proliferation, and tissue remodeling. ADMs can be derived from various sources, including human cadaveric skin and porcine or bovine dermis. One of the significant advantages of ADMs is their ability to provide a three-dimensional structure that supports cellular infiltration and vascularization. Unlike autologous skin grafts, which require a split-thickness or full-thickness harvest from the patient's own skin, ADMs eliminate the need for donor sites and reduce associated complications. This aspect of ADMs makes them particularly useful for patients with limited donor sites or extensive burns. ADMs have revolutionized the field of skin grafting by offering several advantages over traditional approaches. Firstly, they promote rapid wound healing and tissue regeneration by providing a scaffold that facilitates cell migration, angiogenesis, and reepithelialization. The ECM components within ADMs create an optimal microenvironment for cellular activities, leading to improved healing outcomes. Furthermore, Acellular Dermal Matrices minimize scar formation and improve cosmetic outcomes. The preserved ECM structure aids in the regeneration of functional skin with a more natural appearance. Additionally, ADMs can be used in combination with autologous grafts to enhance their effectiveness, providing better contour and improved esthetics in complex reconstructions. Another significant benefit of ADMs is their versatility in accommodating various surgical techniques. They can be used as full-thickness grafts, dermal substitutes, or in combination with split-thickness grafts. This flexibility allows surgeons to tailor the grafting approach to meet the specific needs of each patient, leading to better outcomes and patient satisfaction. ADMs also find applications beyond skin grafting. They have been used successfully in breast reconstruction following mastectomy, treatment of chronic wounds, and repair of soft tissue defects in various regions of the body. The ability to integrate with the host tissue and stimulate neovascularization makes ADMs a valuable tool in regenerative medicine. As the field of regenerative medicine continues to evolve, the future of skin grafting appears promising with the widespread adoption of ADMs. Ongoing research aims to enhance the properties of Acellular Dermal Matrices, including their mechanical strength, immunogenicity, and bioactivity. Additionally, the development of tissue-engineered skin substitutes, incorporating stem cells and growth factors within ADMs, holds tremendous potential for accelerated wound healing and tissue regeneration. However, several challenges must be addressed for ADMs to become the standard in skin grafting. The cost-effectiveness of ADMs remains a concern, as they are currently more expensive than autologous grafts. Further advancements in processing techniques and scaling up production may help address this issue. Acellular Dermal Matrices have emerged as a transformative approach to skin grafting, offering numerous advantages over traditional methods. Their ability to promote tissue regeneration, improve cosmetic outcomes, and reduce donor site morbidity makes them a promising option for patients in need of skin reconstruction. With ongoing research and technological advancements, ADMs are likely to play a central role in the future of regenerative medicine. By addressing challenges such as cost-effectiveness and further refining their properties, ADMs have the potential to revolutionize the field and significantly improve patient outcomes in skin grafting procedures.
0 Comments
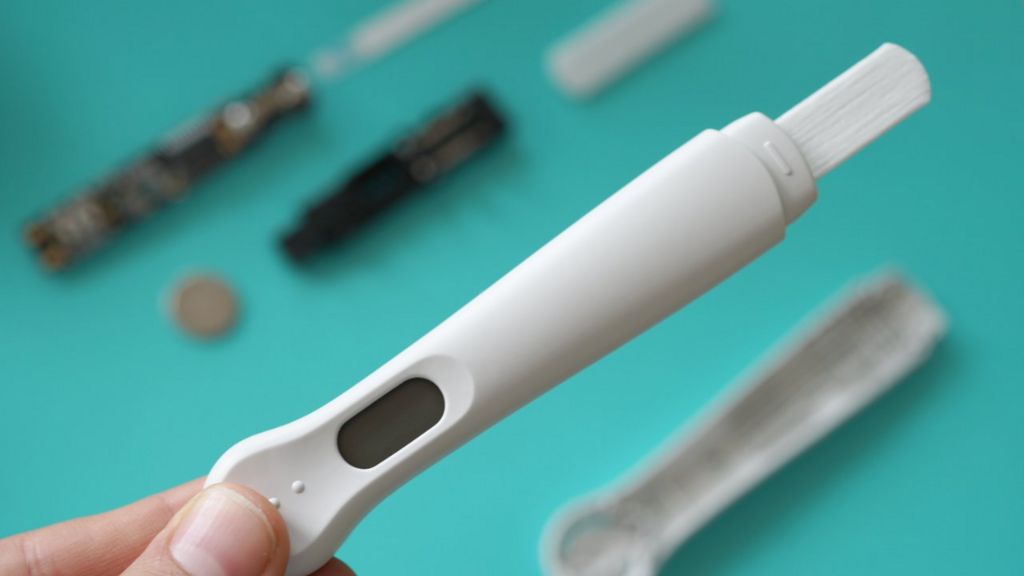
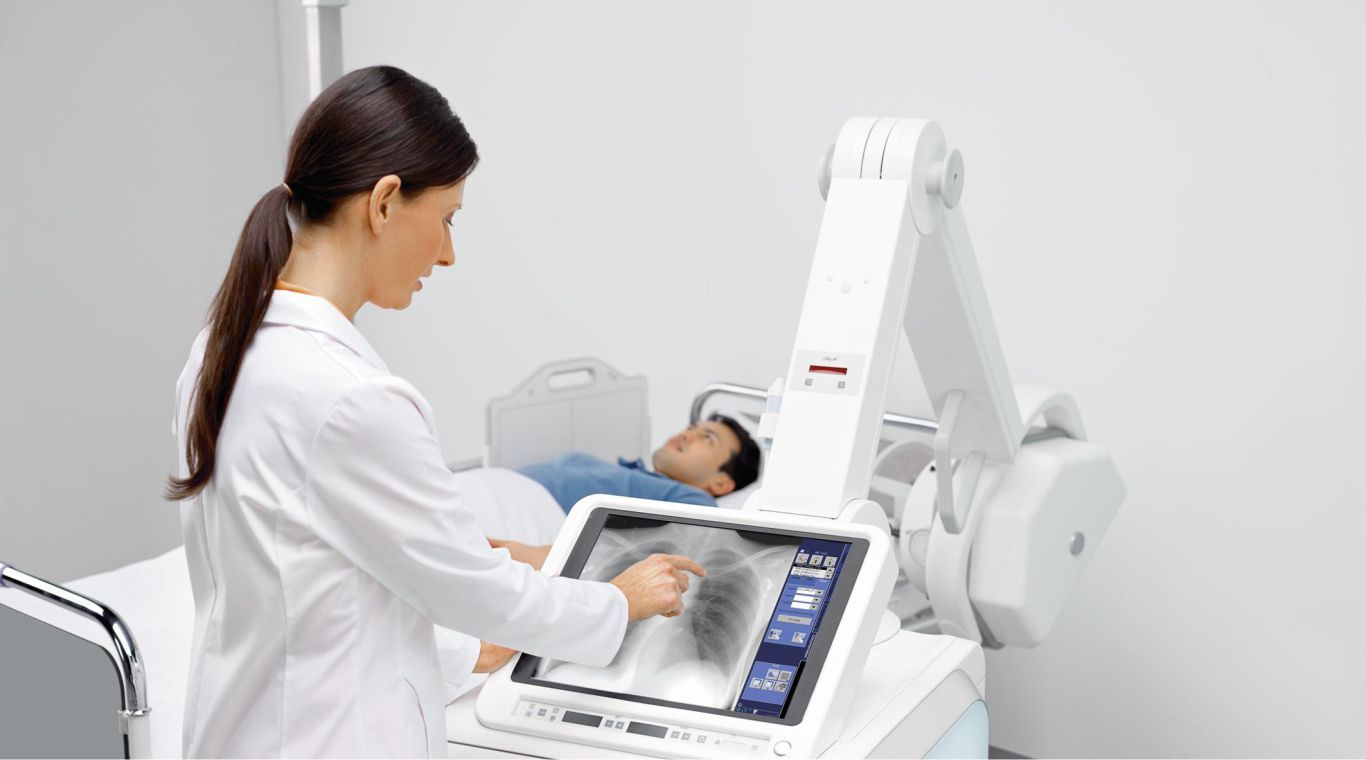
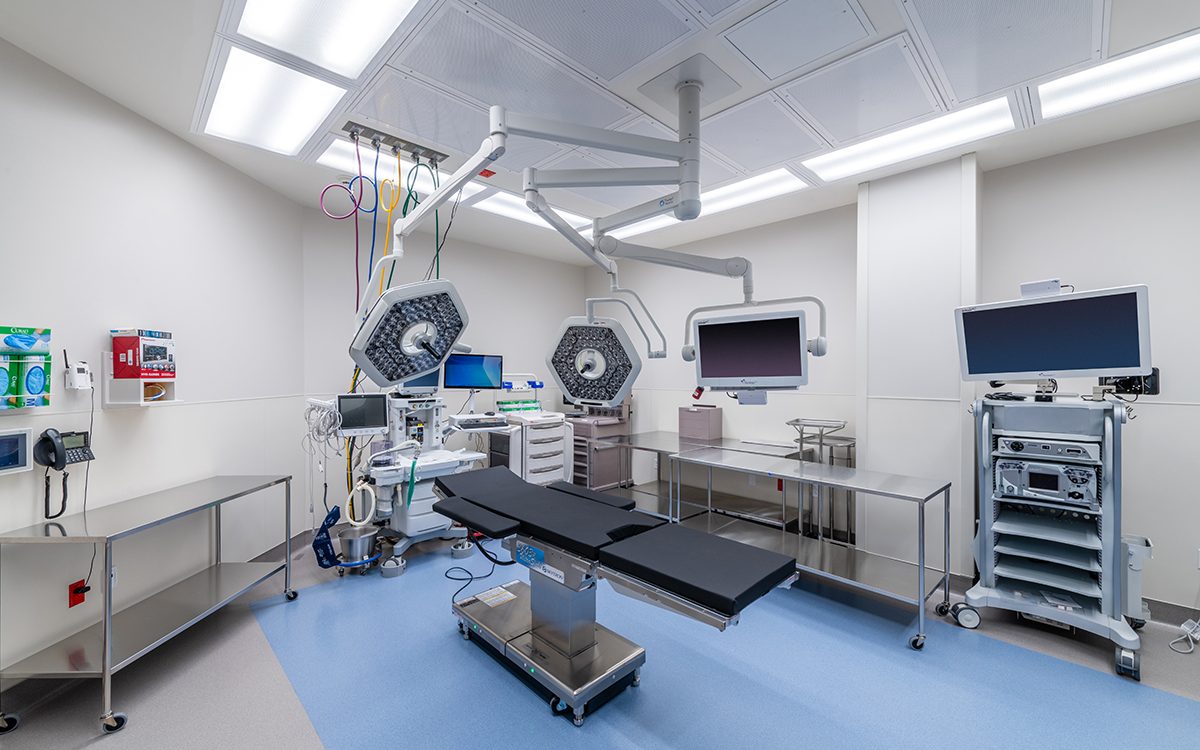
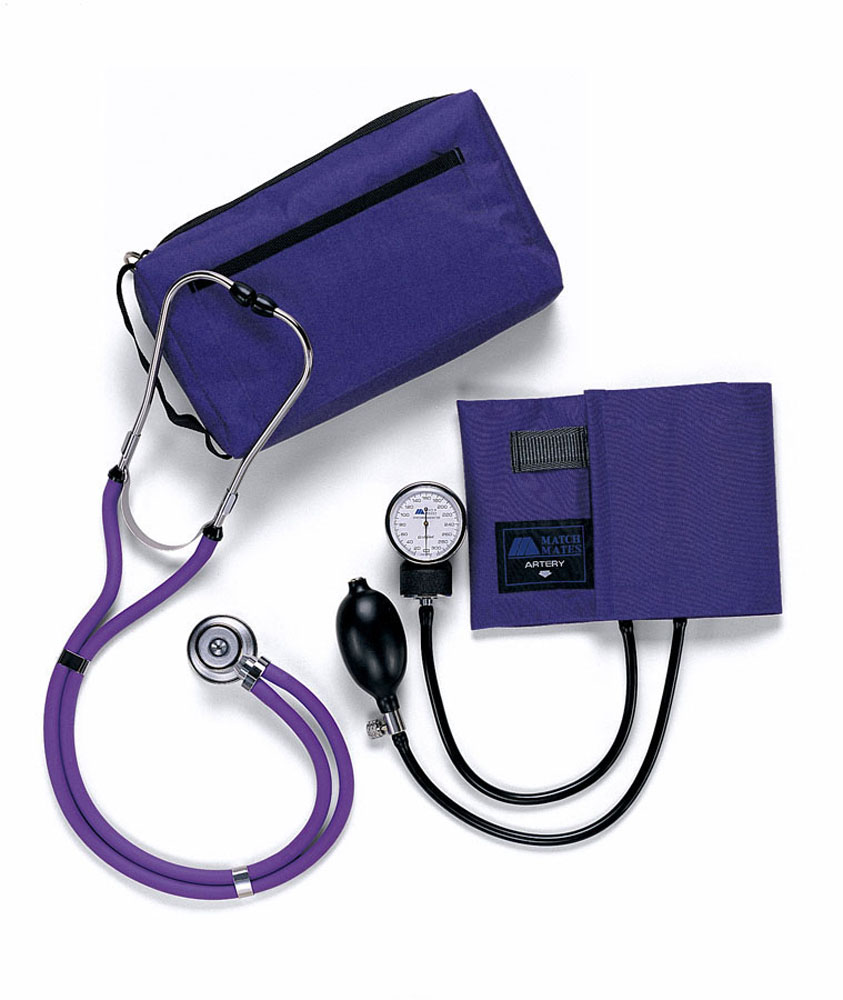
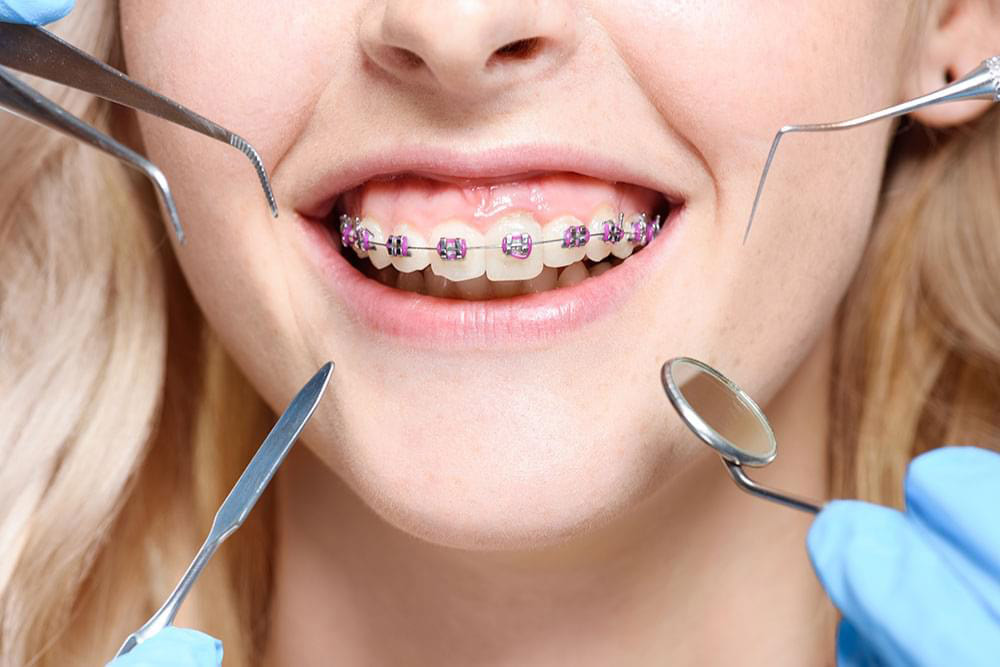
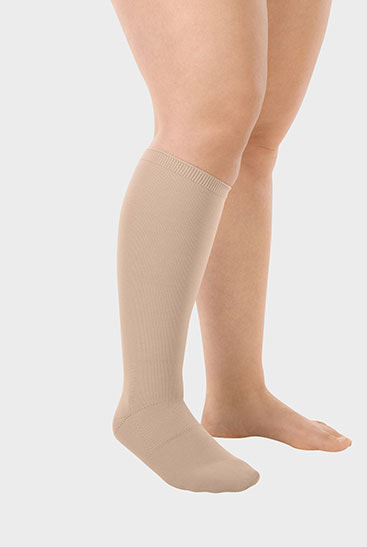
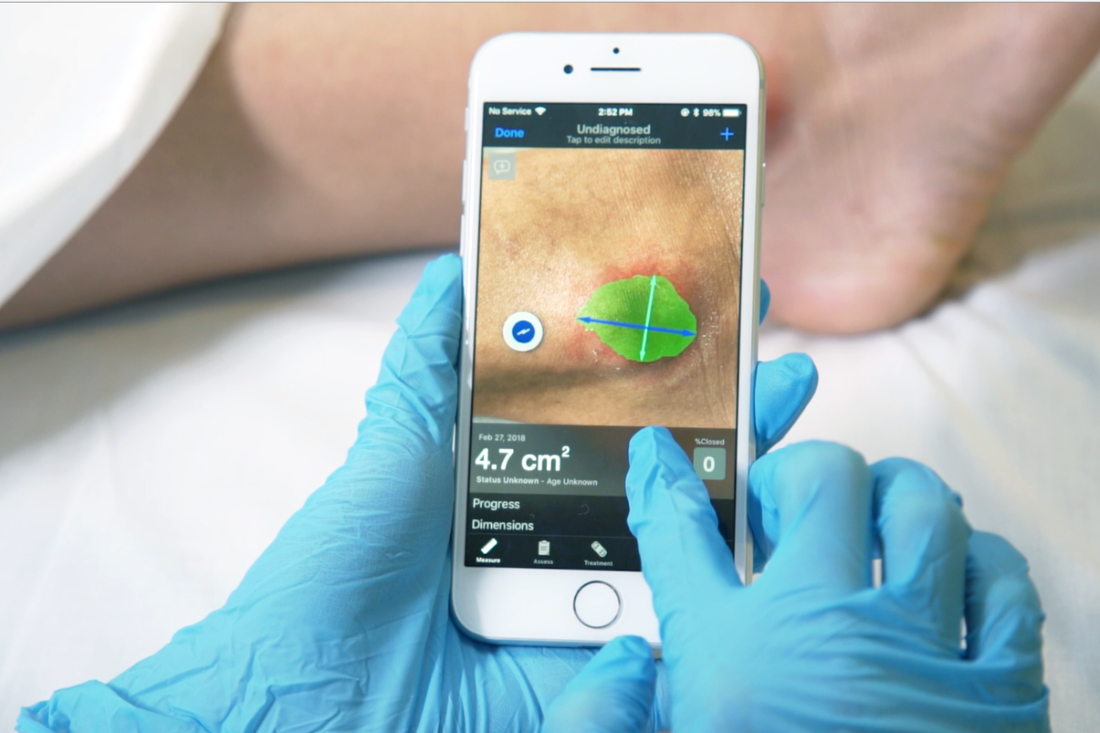
Pregnancy is a life-altering experience that brings joy, anticipation, and a whole array of emotions. For women who are trying to conceive or suspect they might be pregnant, the journey begins with a pregnancy test. In recent years, the advancements in technology have revolutionized the way we approach pregnancy testing. Among these innovations, the Digital Pregnancy Test Kits has emerged as a modern solution for early detection, providing women with quick, reliable results and empowering them with valuable information about their pregnancy. In this article, we will delve into the features, benefits, and the significance of the Digital Pregnancy Test Kit in today's world. The Digital Pregnancy Test Kits is a sophisticated device designed to detect the presence of human chorionic gonadotropin (hCG) hormone in a woman's urine, which indicates pregnancy. What sets it apart from traditional pregnancy tests is its digital display, which clearly indicates whether the result is positive or negative. This eliminates the need for interpreting faint lines or ambiguous results, offering women a definitive answer in a matter of minutes. Early detection of pregnancy holds numerous benefits for women. It allows for timely medical care, proper prenatal care, and early adoption of a healthy lifestyle. By detecting pregnancy at its earliest stages, women can make informed decisions about their diet, exercise routine, and overall well-being. Moreover, early detection can help identify any potential complications or risks, enabling healthcare providers to offer appropriate guidance and support. The Digital Pregnancy Test Kits boasts a high level of reliability and accuracy, giving women the confidence they need during this critical phase of their lives. Its advanced technology minimizes the chances of false positives or false negatives, providing dependable results that women can trust. This reliability is a result of rigorous testing and adherence to strict quality control standards, ensuring the utmost precision in detecting hCG levels. One of the standout features of the Digital Pregnancy Test Kit is its user-friendly interface. The clear digital display eliminates any confusion that may arise from traditional tests, making it accessible and easy to use for women of all ages. The simplicity of its design ensures that women can administer the test confidently in the comfort of their own homes, without the need for any specialized medical knowledge. Through the use of contrast chemicals and X-ray imaging, Cerebral Angiography plays a critical role in the diagnosis and evaluation of diseases like stroke, aneurysms, and arteriovenous malformations. High-resolution detectors and sophisticated image processing software have improved the quality and accuracy of cerebral angiography images, which has further fueled growth. In addition to its accuracy, the Digital Pregnancy Test Kit offers women the privacy and convenience they desire. The discreet nature of the test allows women to maintain confidentiality and perform the test at a time and place of their choosing. This eliminates the need for visits to healthcare facilities solely for the purpose of taking a pregnancy test, giving women more control over their personal journey. The Digital Pregnancy Test Kits goes beyond providing a simple positive or negative result. Some models offer additional features such as weeks indicator, which estimates the number of weeks since conception. This feature offers valuable information to women, helping them understand the progression of their pregnancy and plan accordingly. It enables them to prepare for the upcoming changes and make informed decisions about their prenatal care. When medical emergencies strike and immediate transportation to a healthcare facility is crucial, air ambulance services provide a lifeline from above. These specialized services play a vital role in swiftly transporting critically ill or injured patients to medical facilities where they can receive the necessary care. With their ability to overcome geographical barriers, Air Ambulance Services ensure that patients reach their destinations safely and expeditiously. This article explores the significance of air ambulance services, their operational procedures, the advanced medical care they provide, and their role in saving lives. In emergency situations, every minute counts. Often, ground transportation is inadequate due to factors such as distance, traffic congestion, or geographical obstacles. Air ambulance services bridge this gap by offering rapid transportation to patients who require immediate medical attention. Whether it's a remote location, a disaster-stricken area, or a time-sensitive situation, air ambulances are equipped to provide efficient and timely assistance. Air Ambulance Services operate with a well-coordinated system involving various professionals, including pilots, medical personnel, and ground support staff. The process typically begins with a request for transportation from a medical facility, emergency response team, or individual. Once the request is received, the air ambulance team assesses the patient's condition, prepares the necessary equipment, and coordinates with the sending and receiving medical facilities. The flight crew, along with medical personnel, ensures a safe and comfortable journey for the patient. Air ambulances are equipped with state-of-the-art medical equipment and highly trained medical professionals. These flying medical units are designed to provide critical care during the transportation process. They are equipped with specialized medical devices, such as cardiac monitors, ventilators, and infusion pumps, to stabilize and support patients with complex medical needs. The medical team on board includes doctors, nurses, and paramedics who are skilled in providing emergency medical interventions. Air ambulances are specially designed aircraft that prioritize patient comfort and safety. These aircraft are equipped with advanced navigation systems, ensuring accurate and efficient transportation even in adverse weather conditions. The aircraft's ability to fly at higher altitudes allows for faster and smoother journeys, reducing travel time significantly. The medical team monitors the patient's condition throughout the flight, making any necessary adjustments to ensure their stability and well-being. Air Ambulance Services cater to a wide range of medical needs. They transport patients who require urgent medical attention, organ transplant recipients, burn victims, neonatal cases, and individuals requiring specialized medical care not available locally. These services also facilitate repatriation of individuals who have fallen ill or been injured while traveling abroad, ensuring they can return home safely for further treatment. Air ambulance services work in collaboration with ground medical services to ensure seamless patient transfers. Ground ambulances are often utilized for transportation to and from the airports, providing a complete door-to-door service. Additionally, the air ambulance team communicates with receiving medical facilities, ensuring that the necessary resources and medical staff are prepared to receive the patient upon arrival. Air ambulance services operate on a global scale, enabling patients to access medical facilities beyond their geographical locations. This is particularly valuable in remote areas or when time is of the essence. Regardless of the distance, air ambulance services offer a lifeline for patients who require immediate medical intervention. Air Ambulance Services are invaluable in emergency medical situations, providing lifesaving solutions from above. With their swift response, advanced medical care, and ability to overcome geographical barriers, air ambulances ensure that critically ill or injured patients reach the medical care they urgently need. These services operate with efficiency, coordination, and a commitment to patient safety. Air ambulance services play a critical role in the healthcare system, saving lives and providing hope for those in need, even in the most challenging circumstances. Read the Press Release of Air Ambulance Services Market Portable X-ray devices have ushered in a new era of precise and accurate diagnosis, placing the power of precision directly in the hands of healthcare professionals. These compact devices combine advanced technology with portability, enabling healthcare providers to obtain high-quality images and make accurate diagnoses in various clinical settings. With portable X-ray devices, precision is no longer confined to dedicated imaging centers. Physicians can now bring the diagnostic capabilities to the patient's bedside, emergency rooms, intensive care units, or even remote locations. This immediate access to imaging plays a pivotal role in critical situations where time is crucial for making accurate diagnoses and prompt treatment decisions. These devices are designed to deliver exceptional image quality while maintaining the highest standards of accuracy. Through cutting-edge imaging technology, such as digital radiography and advanced image processing algorithms, Portable X-Ray Devices provide detailed and precise images of anatomical structures. This precision aids healthcare professionals in detecting subtle abnormalities, identifying fractures, assessing lung conditions, and evaluating the progression of diseases. Moreover, the convenience of portable X-ray devices enhances workflow efficiency. With streamlined processes and quick image acquisition, healthcare providers can promptly review and interpret X-ray images, leading to timely interventions and improved patient outcomes. The ability to obtain real-time esults empowers healthcare professionals to make informed decisions and develop personalized treatment plans tailored to each patient's needs. In addition to their diagnostic accuracy, portable X-ray devices offer the benefits of reduced radiation exposure. Advanced dose management systems and optimized imaging techniques ensure that patients receive the lowest possible radiation dose without compromising image quality. This focus on patient safety and radiation reduction underscores the commitment to precision and quality care. Portable X-ray devices have revolutionized the way accurate diagnoses are made by putting precision in the hands of healthcare professionals. These devices enable immediate access to high-quality images, ensuring precise interpretations and facilitating prompt treatment decisions. With their portability, advanced technology, and focus on patient safety, portable X-ray devices have become indispensable tools for achieving accurate diagnoses and delivering optimal patient care. Explore More- https://cmiblogdailydose.blogspot.com/2023/07/portable-x-ray-devices-are-aids-in-home.html In recent years, there has been a significant shift in the way healthcare services are delivered, with a growing emphasis on efficiency and convenience. Ambulatory Surgical Centers (ASCs) have emerged as a viable alternative to traditional hospital-based surgeries, offering numerous advantages to both patients and healthcare providers. Ambulatory Surgical Centers, also known as outpatient surgery centers, are healthcare facilities that specialize in providing same-day surgical procedures. Unlike hospitals, ASCs focus solely on elective surgeries that do not require overnight stays. These centers are equipped with state-of-the-art medical technology and staffed by highly skilled healthcare professionals, ensuring the highest standards of care and safety. One of the primary advantages of Ambulatory Surgical Centers is the convenience they offer to patients. With shorter wait times, streamlined admission and discharge processes, and a patient-centered approach, ASCs prioritize efficiency and minimize disruptions to patients' daily lives. Patients can schedule their surgeries at a time that is most convenient for them, eliminating the need for prolonged hospital stays and allowing for a quicker recovery in the comfort of their own homes. Moreover, Ambulatory Surgical Centers often provide a more relaxed and personalized environment compared to hospitals, which can contribute to reduced anxiety and improved patient satisfaction. The focused nature of ASCs allows for specialized care and enhanced attention to individual patients, ensuring a high-quality surgical experience. Ambulatory Surgical Centers are designed to maximize efficiency and optimize resource utilization. With a streamlined workflow, ASCs minimize delays and effectively utilize operating room time, resulting in shorter surgical durations and improved overall efficiency. This translates into cost savings for both patients and healthcare systems. ASCs typically have lower overhead costs compared to hospitals, making them a more cost-effective option for elective surgeries. The reduced expenses are passed on to patients in the form of lower out-of-pocket costs and can also contribute to lower healthcare insurance premiums. For healthcare providers, ASCs provide an avenue to increase their procedural capacity and improve revenue generation. Patient safety and quality of care are paramount in Ambulatory Surgical Centers. These centers are subject to rigorous accreditation standards and regulatory requirements to ensure compliance with best practices and guidelines. ASCs adhere to stringent infection control measures, maintain high standards of sterility, and implement comprehensive safety protocols to mitigate risks associated with surgical procedures. Furthermore, Ambulatory Surgical Centers maintain close relationships with referring physicians and specialists, fostering a collaborative approach to patient care. This seamless coordination among healthcare professionals helps optimize surgical outcomes and facilitates comprehensive post-operative follow-up care. Ambulatory Surgical Centers offer a wide range of surgical procedures across various specialties, including ophthalmology, orthopedics, gastroenterology, dermatology, and more. From cataract surgeries to hernia repairs, ASCs have the capabilities to perform numerous procedures that can be safely and effectively completed on an outpatient basis. The advancement of medical technology has also contributed to the expansion of the types of procedures performed in ASCs. Minimally invasive techniques, such as laparoscopic surgeries, have become increasingly common in ASCs, providing patients with less invasive options and faster recovery times. Ambulatory Surgical Centers have transformed the landscape of outpatient surgeries, providing patients with efficient, convenient, and high-quality care. With their patient-centric approach, focus on safety and quality, cost-effectiveness, and a wide range of procedures offered, ASCs have become an attractive choice for elective surgeries. Blood Pressure Cuffs Are Vital Tools That Enhance Patient Safety And Care In Multiple Ways27/6/2023 Blood pressure cuffs play a crucial role in healthcare settings by providing valuable information about a patient's cardiovascular health. They are used extensively in hospitals, clinics, and even at home to measure blood pressure, a vital parameter in diagnosing and managing various medical conditions. One of the primary reasons blood pressure cuffs are instrumental in patient safety is their reliability and accuracy. Medical professionals rely on these devices to obtain accurate blood pressure measurements, which serve as critical indicators of a patient's overall health. High-quality blood pressure cuffs are designed to provide consistent readings, reducing the risk of misdiagnosis or improper treatment. They undergo rigorous calibration to ensure precise measurements, minimizing errors and enhancing patient safety. Blood Pressure Cuffs are designed to be user-friendly and accessible to both healthcare professionals and patients. They are available in various styles and sizes, catering to different individuals' needs. With advancements in technology, digital blood pressure cuffs have gained popularity due to their ease of use. These devices feature user-friendly interfaces, clear displays, and straightforward operation, allowing patients to monitor their blood pressure conveniently at home. This accessibility empowers individuals to take an active role in their healthcare, promoting early detection of abnormalities and proactive management of blood pressure. Standardization is crucial in the medical field to ensure consistent and comparable measurements across different healthcare settings. Blood pressure cuffs adhere to specific standards and guidelines set by organizations such as the American Heart Association (AHA) and the Association for the Advancement of Medical Instrumentation (AAMI). These standards define the appropriate cuff sizes, inflation levels, and measurement techniques, promoting uniformity in blood pressure measurement. Standardization enables healthcare professionals to interpret blood pressure readings accurately, leading to consistent care and better patient outcomes. Blood pressure cuffs offer several benefits that contribute to enhanced patient care. Firstly, regular blood pressure monitoring enables early detection and intervention in cases of hypertension, a leading risk factor for cardiovascular disease. By identifying high blood pressure readings, healthcare providers can initiate lifestyle modifications, prescribe medications, and closely monitor patients to prevent complications such as heart attacks, strokes, and organ damage. Secondly, blood pressure cuffs assist in monitoring the effectiveness of treatment plans. For patients with hypertension or other cardiovascular conditions, regular blood pressure measurements help gauge the response to medication, lifestyle changes, or interventions. Adjustments can be made promptly to optimize treatment and ensure better control over blood pressure levels. Additionally, blood pressure cuffs play a crucial role in preventing adverse events during medical procedures. Prior to surgeries or certain medical interventions, healthcare professionals use blood pressure cuffs to assess a patient's baseline blood pressure and identify potential risks. During procedures, continuous monitoring with blood pressure cuffs helps detect any sudden changes, allowing for immediate interventions and reducing the risk of complications. An acoustic medical tool called a stethoscope is used to physically examine humans or animals via auscultation. The resonator put beneath the tiny disc at one end amplifies sounds from the foetal heartbeat, lungs, and oesophagus. A Stethoscope is an essential tool for a physical examination in the medical field. The incidence of cardiovascular disease is on the rise, there are more healthcare professionals, and medical facilities are getting better, all of which are major growth factors for the stethoscope market. Furthermore, blood pressure cuffs facilitate the management of chronic conditions outside of clinical settings. Home blood pressure monitoring has become increasingly popular, allowing patients to track their blood pressure readings regularly and share them with their healthcare providers. This practice enables remote monitoring, early intervention, and personalized care plans, promoting patient engagement and empowerment. Orthodontics is a specialized branch of dentistry that focuses on the diagnosis, prevention, and treatment of dental and facial irregularities. It is a science that aims to achieve dental harmony, ensuring not only straight teeth but also a balanced and functional bite. By understanding the principles and techniques of orthodontics, dental professionals can help patients achieve healthy, beautiful smiles while improving their overall oral health. The foundation of Orthodontics lies in the understanding of dental occlusion, which refers to the way the upper and lower teeth come together when biting or chewing. Ideally, the upper teeth should fit slightly over the lower teeth, allowing for proper function and equal distribution of bite forces. However, various factors can disrupt this harmony, leading to malocclusions or improper bites. A Study By Coherent Market Insights Says, The Global Orthodontics Market Was Valued At US$ 5.23 Billion In 2022 And Is Forecast To Reach A Value Of US$ 8.95 Billion By 2030 At A CAGR Of 6.94% Between 2023 And 2030. Malocclusions can be classified into different types, such as crowding, spacing, overbite, underbite, crossbite, and open bite. These conditions may result from genetic factors, abnormal tooth development, habits like thumb sucking, or facial trauma. If left untreated, malocclusions can lead to problems like difficulty in chewing, speech impairments, jaw pain, and increased risk of tooth decay and gum disease. Orthodontic treatment involves the use of various devices and techniques to align and straighten the teeth, correct bite issues, and improve facial aesthetics. The most commonly known orthodontic appliance is braces, which consist of brackets bonded to the teeth and wires that apply gentle pressure to guide the teeth into proper alignment. Braces can effectively address a wide range of dental problems and are suitable for both children and adults. In recent years, there have been significant advancements in Orthodontics, introducing more discreet and comfortable treatment options. Clear aligners, such as Invisalign, have gained popularity as an alternative to traditional braces. These custom-made, transparent trays gradually shift the teeth into the desired position, offering a nearly invisible and removable orthodontic solution. Orthodontic treatment begins with a comprehensive evaluation of the patient's dental and facial structures. This involves taking X-rays, photographs, and dental impressions to create a detailed treatment plan. The orthodontist considers factors like the patient's age, severity of the malocclusion, skeletal growth, and individual treatment goals. Once the treatment plan is established, the orthodontist initiates the active phase of treatment. This involves placing the braces or prescribing clear aligners and monitoring the progress through periodic adjustments. Over time, the teeth respond to the applied forces, gradually shifting into their proper positions. Regular check-ups are crucial during Orthodontics treatment to ensure that the teeth are moving correctly and to make any necessary adjustments. These appointments also provide an opportunity for the orthodontist to address any concerns or discomfort experienced by the patient. Orthodontic treatment typically lasts from several months to a few years, depending on the complexity of the case. Once the desired results are achieved, the active treatment phase concludes, and the patient enters the retention phase. During this stage, a retainer is prescribed to maintain the newly achieved alignment of the teeth. Retainers are usually worn full-time initially and gradually transitioned to nighttime use only. The science of Orthodontics extends beyond the physical aspects of tooth movement. It also considers the impact of orthodontic treatment on a patient's self-esteem, confidence, and overall well-being. A straight, healthy smile can boost self-confidence and positively influence social interactions, leading to improved psychological and emotional well-being. A three-dimensional object is built via additive manufacturing, commonly known as 3D printing, from a CAD model or digital 3D model. A digital model can be used to construct an object of any size and shape. The main idea behind 3D Printing is the translation of code, material cartridges, and output flexibility into an obvious pattern. Currently, this technology is utilised for mass customization, mass production, quick manufacturing, and rapid prototyping. Orthodontics is a science that encompasses the diagnosis, prevention, and treatment of dental irregularities. By utilizing various techniques and appliances, orthodontists can achieve dental harmony, aligning teeth and correcting bite issues. Orthodontic treatment not only improves the aesthetics of a smile but also contributes to better oral health and overall well-being. Compression Stockings Are Specialized Garments Designed To Exert Graduated Pressure On The Limb21/6/2023 Venous Thromboembolism (VTE) is a significant concern in the intensive care unit (ICU) setting, posing a substantial risk to critically ill patients. It encompasses deep vein thrombosis (DVT), the formation of blood clots in deep veins, and pulmonary embolism (PE), a potentially life-threatening condition when a clot travels to the lungs. To combat this risk, Compression Stockings have emerged as an effective preventive measure in the ICU. VTE is a multifactorial condition influenced by several factors prevalent in the ICU, including prolonged immobility, invasive procedures, and underlying medical conditions. Critically ill patients are particularly susceptible due to reduced mobility, compromised venous return, and increased blood coagulability. VTE can have severe consequences, leading to organ damage, prolonged hospitalization, and even mortality. Therefore, early identification and prevention of VTE are paramount in the ICU. Compression Stockings, also known as anti-embolism stockings or graduated compression stockings, are specialized garments designed to exert external pressure on the legs, promoting venous return and reducing the risk of blood clot formation. These stockings apply graduated pressure, with the highest compression at the ankle and gradually decreasing towards the thigh. The pressure gradient facilitates the movement of blood from the legs towards the heart, preventing stasis and clot formation. Minimizing VTE Risks in the ICU: 1. Enhanced Blood Flow: Compression Stockings exert pressure on the superficial veins, assisting the calf muscles' pumping action in propelling blood towards the heart. This enhanced blood flow reduces the risk of blood pooling and clot formation, mitigating the chances of DVT development. 2. Prevention of Venous Stasis: Prolonged immobilization in the ICU can lead to venous stasis, where blood remains stagnant in the veins. Compression stockings combat venous stasis by facilitating the movement of blood and preventing its pooling, thereby reducing the risk of clot formation. 3. Reduction in Edema: Critically ill patients often experience edema, characterized by fluid accumulation in the legs. Compression stockings aid in reducing edema by promoting lymphatic drainage and minimizing fluid retention, which can contribute to improved circulation and decreased VTE risks. 4. Patient Mobility: ICU patients face significant challenges in mobility due to their critical condition. Compression stockings provide a non-invasive and readily available method to support their mobility efforts. These stockings allow patients to move their legs more comfortably, facilitating early ambulation and minimizing the risk of VTE. 5. Complementary to Pharmacological Prophylaxis: Compression Stockings can be used in conjunction with pharmacological interventions, such as anticoagulant medications, to provide comprehensive VTE prevention. The combination of compression stockings and pharmacological prophylaxis has demonstrated synergistic effects, further reducing VTE risks. There are four fundamental biotechnology systems. The first system addresses how biotechnology is used in medications. The following approach makes use of biotechnology to create fresh industrial processes and chemicals. The production of seeds and genetically engineered crops using Biotechnology is the subject of the following significant section. The final section, which is the least established, discusses the employment of biotechnology in maritime environments. These biotechnology uses fall under the headings of biopharmacy, bioagriculture, bioindustrial, and bioservices. Deep Vein Thrombosis (DVT) is a potentially life-threatening condition characterized by the formation of blood clots in the deep veins of the legs. Hospitalized patients, especially those with limited mobility, are at a higher risk of developing DVT due to prolonged periods of immobility. Compression Stockings have emerged as a crucial intervention for preventing DVT in these patients. The healthcare industry has witnessed remarkable advancements in technology, revolutionizing various aspects of patient care. One notable development is the emergence of virtual Intensive Care Units (ICUs), which integrate cutting-edge technologies to monitor and manage critically ill patients remotely. Virtual ICUs leverage real-time data, artificial intelligence (AI), and telecommunication to extend critical care expertise beyond the traditional hospital setting. This essay delves into the virtual ICU landscape, highlighting its benefits, challenges, and potential impact on patient outcomes. Virtual ICU offer numerous advantages that enhance critical care delivery. Firstly, these systems enable round-the-clock monitoring by a team of intensivists and critical care nurses, ensuring continuous surveillance of patients' vital signs and immediate response to emergencies. This constant monitoring reduces the risk of adverse events and improves patient safety. Moreover, virtual ICUs facilitate rapid access to specialized critical care expertise, irrespective of geographical constraints. Patients in rural or underserved areas can receive high-quality care, as they are virtually connected to experienced clinicians located in urban centers. Furthermore, Virtual ICU leverage AI algorithms to analyze real-time data, enabling early detection of deteriorating conditions and prediction of potential complications. This predictive capability allows healthcare providers to intervene promptly, preventing adverse outcomes and reducing mortality rates. Additionally, virtual ICUs facilitate seamless communication and collaboration among healthcare teams, enabling remote consultation and multidisciplinary decision-making. This streamlined communication enhances care coordination and ensures the provision of evidence-based treatments. Despite their potential benefits, virtual ICUs face several challenges and limitations. One key concern is the reliance on technology, which introduces the risk of technical failures and connectivity issues. Inadequate internet bandwidth or power outages could disrupt the real-time monitoring and communication systems, potentially compromising patient care. Additionally, the implementation of virtual ICUs requires significant financial investment, including the cost of infrastructure, equipment, and training. Smaller healthcare facilities or resource-constrained settings may struggle to afford such technology, limiting its widespread adoption. Another challenge is the ethical and legal implications associated with Virtual ICU. Privacy and patient confidentiality must be safeguarded, as remote monitoring involves transmitting sensitive health information. Adhering to stringent data protection measures, such as encryption and secure communication channels, is crucial to ensure patient privacy. Moreover, clear guidelines and regulations must be established to address issues related to licensure, liability, and accountability in virtual critical care settings. Virtual ICUs have the potential to significantly impact patient outcomes. By facilitating early detection of complications and prompt intervention, these systems can reduce mortality rates and improve patient survival. Studies have shown that virtual ICUs lead to reduced lengths of stay in the ICU and the hospital, enabling efficient utilization of healthcare resources. Moreover, the continuous monitoring and proactive management of patients' conditions can prevent adverse events, such as ventilator-associated pneumonia or medication errors. Furthermore, Virtual ICU promote standardized care practices through the implementation of evidence-based protocols and guidelines. This consistency in care delivery minimizes variations and improves clinical outcomes. Additionally, the availability of specialized critical care expertise through virtual consultations ensures that patients receive appropriate interventions and treatments, even in areas lacking in-house critical care specialists. This accessibility to expert care helps bridge the gap between urban and rural healthcare facilities, reducing health disparities. Virtual ICUs have emerged as a transformative solution, augmenting critical care delivery by leveraging technology, AI, and telecommunication. The benefits of continuous monitoring, rapid access to expertise, and predictive analytics offer tremendous potential for improving patient outcomes and optimizing resource utilization. In recent years, there has been a remarkable rise in the use of Digital Wound Measurement Devices in healthcare. These innovative tools have revolutionized the field of wound care by providing clinicians with accurate and efficient methods to assess wounds. By utilizing advanced technologies such as imaging, computer vision, and artificial intelligence, digital wound measurement devices offer precise measurements, automated documentation, and enhanced data analysis. Accurate wound assessment plays a crucial role in effective wound management. Traditionally, wound measurement relied on manual techniques, which were time-consuming, subjective, and prone to human error. Digital Wound Measurement Devices address these limitations by providing objective and standardized measurements. These devices capture high-resolution images of wounds and employ advanced algorithms to analyze key parameters such as wound area, depth, and volume. This data not only assists in determining wound healing progress but also aids in identifying factors that may impede the healing process, such as infection or inadequate blood supply. The rise of digital wound measurement devices can be attributed to significant technological advancements. Imaging technologies such as high-resolution cameras, infrared, and 3D scanning enable precise wound visualization. Computer vision algorithms allow for automated wound segmentation, ensuring accurate wound area calculations. Additionally, machine learning and artificial intelligence algorithms enable the identification of wound characteristics, patterns, and the prediction of healing trajectories. These technologies work in tandem to provide clinicians with a comprehensive understanding of wound status and aid in making informed treatment decisions. Digital Wound Measurement Devices offer numerous benefits over traditional wound assessment methods. Firstly, they save valuable time for clinicians, as measurements can be obtained swiftly and accurately. This allows healthcare professionals to focus more on patient care and treatment planning. Secondly, digital devices eliminate subjectivity in wound measurement, leading to improved reliability and consistency. Objective measurements also facilitate better communication between healthcare providers, as wound data can be easily shared and accessed. Furthermore, digital devices generate detailed documentation, allowing for better tracking of wound progress over time. These comprehensive records aid in research, quality improvement initiatives, and legal documentation if necessary. Digital wound measurement devices find applications across various healthcare settings. In acute care, these devices assist in triaging wounds, monitoring post-operative healing, and preventing complications. In long-term care facilities, digital devices help in the management of chronic wounds such as pressure ulcers and diabetic foot ulcers. Home healthcare providers can utilize digital devices to remotely monitor wounds, enabling early intervention and reducing unnecessary hospital visits. Additionally, clinical research benefits from digital wound measurement devices, as they provide standardized data collection, contribute to evidence-based practice, and facilitate the evaluation of novel wound care interventions. The rise of Digital Wound Measurement Devices has the potential to significantly impact patient outcomes and healthcare efficiency. By providing accurate and objective wound measurements, these devices aid in timely treatment interventions, preventing complications, and promoting faster wound healing. The ability to track wound progress over time allows healthcare professionals to identify trends and adjust treatment plans accordingly. Moreover, digital devices contribute to the efficient utilization of healthcare resources by reducing the need for repeated assessments, optimizing wound care supply management, and facilitating telehealth wound consultations. |
Categories
All
|