|
In today's rapidly evolving world of scientific research and development, Contract Research Organization (CROs) play a vital role in driving innovation. CROs are specialized companies that provide a wide range of research services to pharmaceutical, biotechnology, and medical device companies. This article explores the significant contributions and essential functions of CROs in advancing scientific discovery and accelerating the development of life-changing therapies. U.S. Contract Research Organization (CROs) serve as collaborative partners, working hand in hand with pharmaceutical companies and research institutions. They bring together multidisciplinary teams of experts with diverse backgrounds and skill sets. These teams consist of scientists, researchers, project managers, and other professionals who possess extensive knowledge and experience in various fields, including preclinical and clinical research, data management, regulatory affairs, and quality assurance. One of the primary roles of CROs is to streamline the complex research processes involved in drug development. They provide comprehensive solutions for study design, protocol development, patient recruitment, data collection, and analysis. By leveraging their expertise and advanced technologies, CROs optimize research operations, ensuring efficiency, accuracy, and adherence to regulatory guidelines. Speed is crucial in the pharmaceutical industry, where time-to-market can make a significant difference. CROs play a pivotal role in expediting the drug development timeline. Their streamlined processes, efficient management of clinical trials, and expertise in navigating regulatory pathways enable faster completion of research studies. By reducing the time required for drug development, CROs contribute to bringing innovative therapies to patients in need more quickly. U.S. Contract Research Organization (CROs) provide access to specialized resources that might not be readily available within pharmaceutical companies or research institutions. These resources include state-of-the-art facilities, advanced laboratory equipment, and cutting-edge technologies. By leveraging these resources, CROs enhance research capabilities, allowing for more comprehensive and robust studies. Additionally, CROs often have extensive networks and partnerships, facilitating collaborations with leading academic institutions and key opinion leaders in various therapeutic areas. Drug development is a costly endeavor, and the financial risks associated with research and clinical trials are significant. Contract Research Organization (CROs) help mitigate these risks by offering flexible business models. Pharmaceutical companies can outsource specific research functions to CROs, enabling them to optimize resource allocation and reduce overhead costs. This strategic approach allows pharmaceutical companies to focus on core competencies while relying on CROs' specialized expertise for specific research activities. On the outside of macrophages are proteins known as Macrophage Markers. They are used to recognize and research macrophages, a category of white blood cell that is crucial to the immune system. Applications for macrophage markers include cancer research, medication development, and clinical diagnostics. Regulatory compliance is a critical aspect of drug development. CROs are well-versed in regulatory requirements and work closely with regulatory authorities to ensure compliance throughout the research process. They maintain rigorous quality assurance systems, standard operating procedures, and adherence to Good Clinical Practice (GCP) guidelines. By following these stringent standards, CROs help ensure the reliability and integrity of research data, ultimately contributing to patient safety and the approval of new therapies. U.S. Contract Research Organization (CROs) play a crucial role in expanding access to clinical trials. By collaborating with research sites globally, they increase the geographical reach of clinical studies. This broadens the pool of eligible participants and facilitates the inclusion of diverse patient populations. Consequently, CROs contribute to the generation of robust data, allowing for more comprehensive evaluations of therapeutic efficacy, safety, and pharmacokinetics. Pharmaceutical companies often face fluctuations in research and development demands. CROs provide the flexibility and scalability required to adapt to changing needs. They can rapidly expand or downsize research teams, allocate resources efficiently, and adjust timelines based on project requirements. This flexibility enables pharmaceutical companies to navigate dynamic market conditions and optimize research investments.
0 Comments
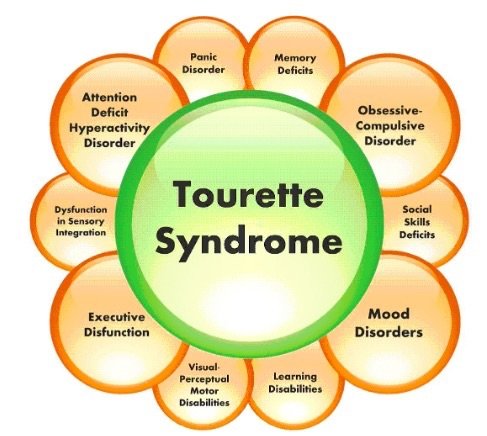
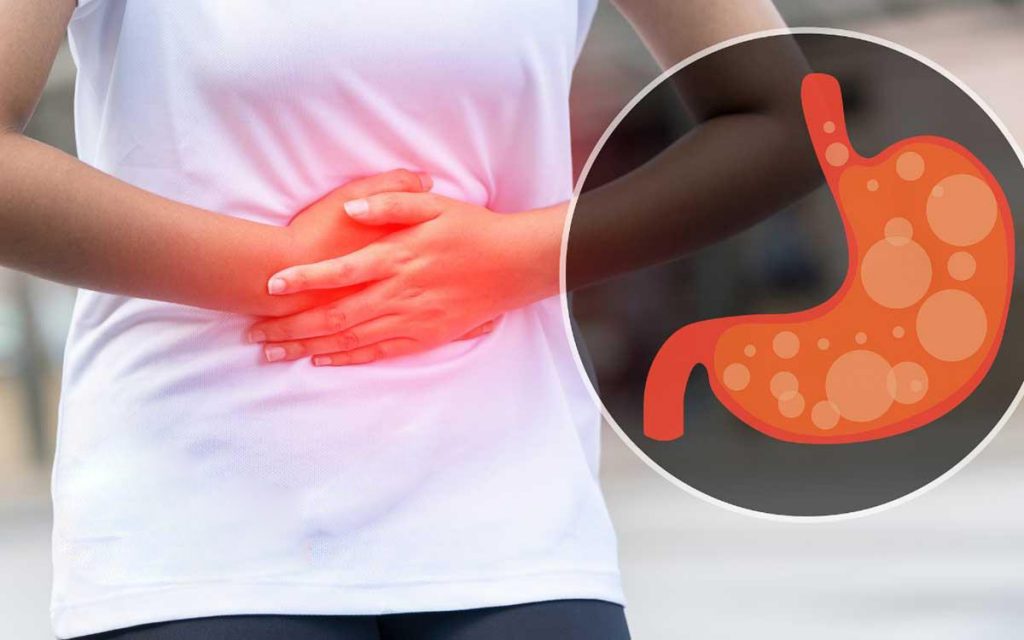
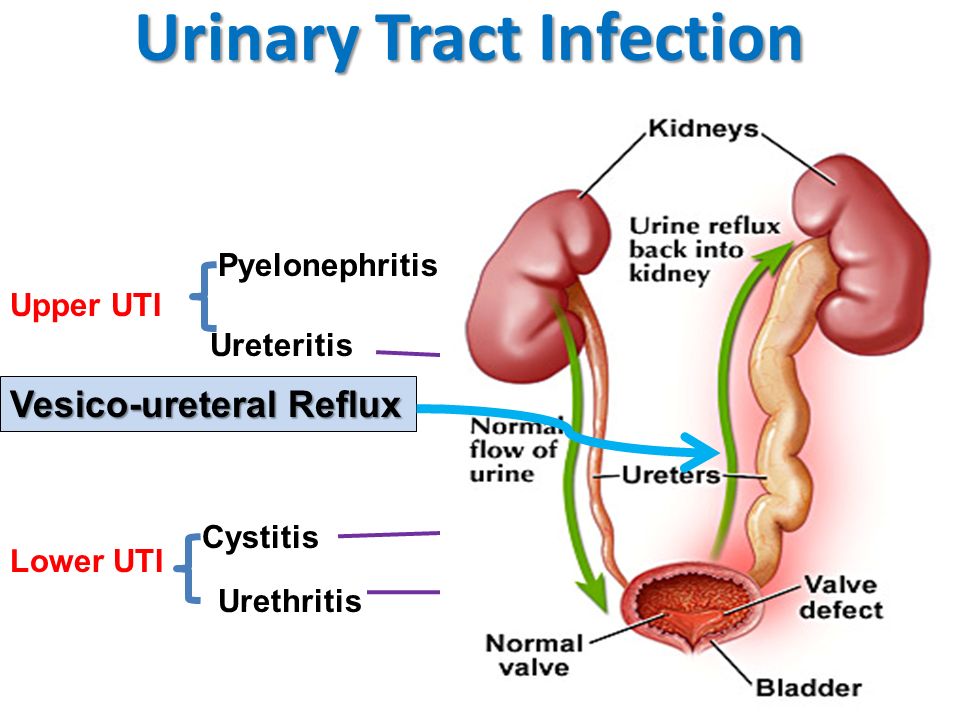
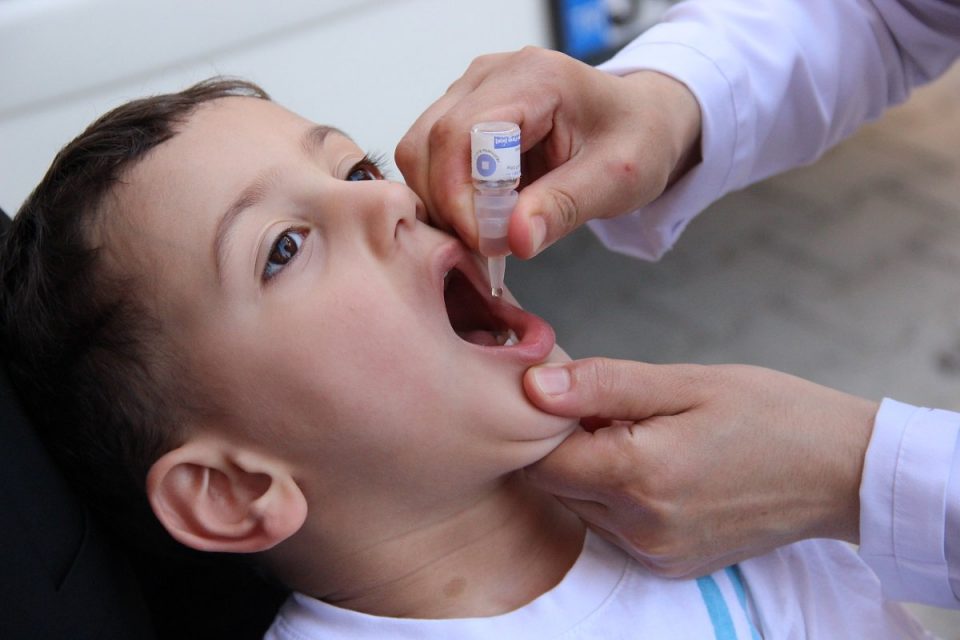
Huntington's disease (HD) is a devastating neurodegenerative disorder characterized by progressive movement abnormalities, cognitive decline, and psychiatric symptoms. Currently, there is no cure for HD, and available treatments focus on managing symptoms and improving quality of life. However, recent advancements in gene therapies have opened up a new frontier in the Huntington's Disease Treatment. Huntington's disease is caused by a mutation in the huntingtin (HTT) gene, which leads to the production of a toxic protein called mutant huntingtin (mHTT). The mHTT protein aggregates in neurons, causing neuronal dysfunction and ultimately leading to cell death. The progressive nature of HD poses a significant challenge in developing effective treatments. Gene Therapies: A Promising Approach: Gene therapy involves the introduction of genetic material into cells to correct or modify gene expression. In the context of HD, gene therapies aim to either silence the mutant HTT gene or enhance the expression of healthy HTT genes. Several strategies have emerged as potential approaches to gene therapy for HD. RNA interference is a technique that utilizes small RNA molecules to selectively degrade specific messenger RNAs (mRNAs). In the context of HD, RNAi aims to silence the mutant HTT gene by targeting its mRNA. Preclinical studies have shown promising results, with the suppression of mHTT protein and amelioration of disease symptoms in animal models. Antisense Oligonucleotides (ASOs) are synthetic DNA or RNA molecules designed to bind to specific mRNA sequences. By targeting the mutant HTT mRNA, ASOs can prevent its translation into the toxic mHTT protein. Clinical trials investigating ASOs in HD patients have shown encouraging outcomes, including a reduction in mHTT protein levels and potential symptomatic benefits. Gene editing technologies such as CRISPR-Cas9 offer precise and targeted modifications to the genome. Researchers are exploring the potential of CRISPR-based strategies to directly edit the mutant HTT gene in HD patients. While still in the early stages of development, these approaches hold promise for correcting the underlying genetic defect. Despite the promising potential of gene therapies, several challenges need to be addressed before they can be widely implemented in Huntington's Disease Treatment. 1. Delivery: Efficient and targeted delivery of gene therapies to the brain remains a significant obstacle. The blood-brain barrier restricts the passage of large molecules, including gene therapy vectors. Developing effective delivery systems that can cross this barrier and specifically target affected brain regions is crucial. 2. Safety: Ensuring the safety of gene therapies is of utmost importance. Gene editing techniques like CRISPR-Cas9 raise concerns about off-target effects and unintended genetic modifications. Rigorous preclinical and clinical studies are necessary to evaluate the long-term safety and potential adverse effects of gene therapies. 3. Timing of Intervention: Determining the optimal time to intervene with gene therapies is critical. Early intervention might be more effective in preventing or slowing disease progression, while intervening during later stages of the disease might focus on symptomatic relief. Defining the appropriate stage of the disease for intervention requires further investigation. 4. Ethical Considerations: The use of gene therapies in HD treatment raises ethical considerations surrounding informed consent, access to treatment, and potential long-term implications. These issues must be carefully addressed to ensure equitable and responsible implementation. Hydroxychloroquine is utilized to inhibit and cure malaria a disease that takes place by parasites in the body and to aid manage the symptoms of lupus or rheumatoid arthritis. The drug is accessible in 200-mg capsules that must be consumed regularly. It can take 1 to 2 months for hydroxychloroquine to start functioning. One should always consume hydroxychloroquine correctly as per physician’s advice. The pharmaceutical label on the drug will tell one how much to consume, how frequent to consume it and any special directives. The physician may start suggesting on a low dosage of hydroxychloroquine and later raise the dose as required. The normal dosage is 1 or 2 pills daily, however the dose may be high or low than this. This drug can lead to severe complications in some individuals. These complications consist rash, alteration in skin pigment, and weakness. If one have these prodromes, one should consult to the physician. These drugs can also lead to severe complications in the cardiac. These complications consist fast or pounding pulse rate, fluttering in the chest, breathlessness, and sudden dizziness. One should get emergency clinical help if one have these prodromes. As Hydroxychloroquine interferes with the usual function of lysosomes, it can cause retinal destruction. This destruction can lead to circular problems in the retina known as bull's eye maculopathy and diametric problems of the retina. This drug can also lead to anemia in some individuals. If one have anemia, one should consult to the physician. Hydroxychloroquine is an antimalarial; a drug that inhibits or cures malaria and can be utilized to cure lupus erythematosus (DLE or SLE), discoid lupus erythematosus, RA, and other inflammatory disorders. It is an anti- human immunodeficiency virus drug and can be utilized to aid inhibit malaria. It is accessible only with a prescription from the physician or pharmacist. It is accessible in a form of capsule and is generally consumed once or two times in a day. Dosage is based on the age and the disorder being cured. Adult dosage ranges from 200 mg to 400 mg daily. This medicine is usually consumed with food and fats such as butter, to decrease GI complications. It can lead to difficulties with the cardiac rhythm called as a prolonged QT interval or ventricular tachycardia. This is a severe and life-threatening problem that could take place if one take it along with medicines that impact the cardiac rhythm, such as the antibiotic azithromycin. A rare problem known as glucose-6-phosphate dehydrogenase deficit may take place in people consuming Hydroxychloroquine persistently. This situation leads to a loss of RBCs that can cause anemia. Hydroxychloroquine can also lead to vision difficulties if one is consuming it for persistent time at high dosage, or if one have pre-existing eye or renal difficulties or a genetic enzyme deficit. These people require regular eye exams every one to five years. It can also cooperate with medicines that reduce the blood sugar such as insulin or certain mellitus medicines. This can lead to hypoglycemia. Hydroxychloroquine is a medicine that can aid with the prodromes of rheumatoid arthritis and lupus. It functions by controlling the immune system to decrease infection and pain. Anyhow, this drug has some drawback that one should know about. The major drawback is that hydroxychloroquine can destruct a part of the eye known as the retina. This occurs very rarely, generally post persistent usage and at high dosage. It is essential to have an eye diagnose post the first year of therapy, then every one to five years. This can be decided with the physician or ophthalmologist. Other drawback of this drug is that it can lead to severe difficulties with the heart rhythm. These takes place very frequently in people who suffer from COVID and who are consuming Hydroxychloroquine with other drugs that impact the cardiac rhythm, such as azithromycin. Sciatica is a common condition characterized by pain that radiates along the path of the sciatic nerve, which extends from the lower back down the legs. It occurs when the sciatic nerve, the longest nerve in the body, becomes compressed or irritated. To comprehend sciatica, it is essential to understand the anatomy of the sciatic nerve. The sciatic nerve originates from the lower back and branches out through the buttocks and down the legs. Any pressure or irritation on this nerve can lead to the development of sciatica symptoms. Sciatica is commonly caused by herniated discs, spinal stenosis, degenerative disc disease, or muscle spasms. It can also be triggered by lifestyle factors such as poor posture, obesity, or sedentary habits. The most prominent symptom of Sciatica is pain that radiates from the lower back through the buttocks and down one or both legs. Other symptoms may include numbness, tingling, or weakness in the affected leg or foot. Diagnosing sciatica involves a comprehensive evaluation of the patient's medical history and a physical examination. The doctor will assess the patient's reflexes, muscle strength, and sensation to identify potential underlying causes. In some cases, diagnostic tests such as X-rays, MRI scans, CT scans, or electromyography (EMG) may be required to confirm the diagnosis and determine the exact cause of sciatica. Most cases of sciatica can be effectively managed through non-surgical approaches. Conservative treatments may include rest, pain medications, physical therapy, hot or cold therapy, and exercises to strengthen the back and core muscles. Medications such as non-steroidal anti-inflammatory drugs (NSAIDs), muscle relaxants, and analgesics can help alleviate pain and reduce inflammation associated with sciatica. Physical therapy plays a crucial role in the treatment of sciatica. A physical therapist can design a tailored exercise program to strengthen the muscles, improve flexibility, and correct posture, thereby reducing pressure on the sciatic nerve. For severe or persistent cases of Sciatica, epidural steroid injections may be recommended. This procedure involves injecting corticosteroids into the affected area to reduce inflammation and provide temporary pain relief. Surgery is usually considered when conservative treatments fail to alleviate symptoms or in cases where there is severe nerve compression. Surgical options for sciatica include discectomy, laminectomy, and spinal fusion, depending on the underlying cause. Practicing proper posture and ergonomics in daily activities can help prevent sciatica by reducing strain on the spine and supporting structures. Engaging in regular physical exercise and stretching routines can strengthen the back muscles, improve flexibility, and promote spinal health, reducing the risk of sciatica. Physical Therapy, also referred to as physiotherapy or PT, is one of the health professions in which healthcare professionals treat a variety of human conditions, including physical impairments brought on by illness, trauma, or injury to the musculoskeletal, cardiovascular, respiratory, neurological, and endocrinological parts of the human system. Maintaining a healthy weight is crucial in preventing Sciatica as excess weight puts additional pressure on the spine and increases the risk of nerve compression. Physical therapy is one of the most effective ways to relieve sciatica pain. A physical therapist can design a customized exercise program that can help reduce pain, strengthen muscles, and improve flexibility. These exercises are specifically designed to target the muscles that support the spine and alleviate pressure on the sciatic nerve. Physical therapy is a safe and non-invasive way to treat sciatica, and it has been proven to be highly effective in reducing symptoms. Medications such as Tourette Syndrome Treatment can help people with Tourette syndrome control their tics. They are called neuroleptics and can reduce or stop tics by limiting the activity of a chemical in the brain called dopamine. Medication is often a first-line Tourette syndrome treatment for severe or difficult-to-treat tics, and for tic-like symptoms that cause problems in social situations. It’s also helpful for patients who have other conditions, such as ADHD, OCD, or anxiety. For some people, a combination of medications can work best as Tourette Syndrome Treatment. A doctor may try different types of drugs and different doses until the right one works for the patient. Besides medication, behavioral therapy and habit reversal training as Tourette syndrome treatment can also be helpful for Tourette syndrome. Behavior therapy can teach patients to recognize when a tic is starting and to make voluntary movements to prevent or reduce the tic. If patients are seeking psychotherapy as a Tourette syndrome treatment or for other reasons, they need to find a therapist they trust and can work well with. The doctor or health insurance plan can help patients to locate a therapist, or they can find one on their own by asking friends or family. Cognitive behavioral therapy (CBT) as Tourette Syndrome Treatment is a form of talk therapy that helps patients identify and modify negative thoughts that can lead to problems. It can also help people change behaviors that are maladaptive. It can also help patients deal with tics and other symptoms that are common in people with Tourette syndrome, such as anxiety, depression, or anger management issues. It can also improve the overall quality of life by helping patients develop coping skills, reduce stress and avoid triggers that could make tics worse. Biofeedback is a non-invasive Tourette syndrome treatment that helps people learn how to control their body's responses. This can help relieve pain, improve performance, or even alleviate symptoms of certain conditions. A therapist attaches sensors to the body and then uses a monitor to provide feedback on changes in brain waves, skin temperature, muscle tension, heart rate, and breathing. During the session, patients try different mental activities and relaxation techniques to reduce these bodily reactions. During this Tourette Syndrome Treatment, patients can learn how to identify and change these involuntary stress response behaviors, which can reduce the tics and help them feel more in control of their life. This technique can be an effective Tourette syndrome treatment when used in conjunction with other treatments such as medication and relaxation strategies. Deep brain stimulation (DBS) is an effective Tourette syndrome treatment for patients with severe, medication-refractory Tourette syndrome. It is typically used in conjunction with other treatments, such as medications and psychotherapy. The first step of this Tourette syndrome treatment involves surgery to implant electrodes into specific parts of the brain. Neurosurgeons use neuroimaging (MRI or CT scans) to map the brain and determine where to place the electrodes. Next, an electrical pulse generator is placed under the skin and linked to the electrodes. It can be programmed to send continuous electrical pulses to the brain. Studies have shown that DBS can reduce tics by targeting the basal ganglia. However, it has not been shown how the exact locations of stimulation affect tic reductions. There is a vast range of OTC Burn Ointment elements. Some consist anti-septic and sedatives to aid keep burns wet and free from inflammation. They are convenient to find and generally are sold in the form of tube or a sachet. Utilizing a cool compress calms the skin, decreases pain and also decrease bulging. One can immerse a fabric or gauze in cold water and cover it over the burn for 10 minutes on a single time. Using petroleum jelly twice to thrice in a day would aid the burn stay wet and aid the skin recovery. It also mimics as a Burn Ointments to keep bandages from being stick to the burn and can aid inhibit inflammation. With small burns, such as a sunburn, one should use aloevera on the burn may aid the skin recovery and decrease pain. It also decreases itching, and there are some proofs that it aids with injury recovery. Several people utilize ice to decrease their burns, however ice captivates the heat in of skin and can lead to more destruction. It is also not disinfectant, so it can lead to the entrance of bacteria into the wound. Butter and Oil are the fats that can irritate the burn and lead to inflammation. Toothpaste is not sterile, so it can lead to the growth of bacteria in the burn and lead to inflammation. There are some things one can perform at house to care for the burn, however one should always listen to the advice of the burn care doctor. Considering the burn crucially would aid it recovery fast and protectively. One of the primary things to perform post getting a burn is to calm it. One can do this by flowing cool water from the burn or by using a compress in 5- to 15-minute breaks. Using an antibacterial cream, such as Bacitracin or Neosporin, to the individual’s burn is proven to aid inhibit inflammation. The Burn Ointments also acts as a barrier so one can modify the dressing not hurting the burn. One can get this burn ointment in the OTC from the nearby pharma. One can also have an antibiotic ointment from the physicians or burn care expert. Other best ointment is the double antibiotic cream, polysporin. This burn ointment consists two antigens: polymyxin B and bacitracin. Topical antigens is the very efficient method to inhibit inflammation in burn injuries. They can decrease pain and decrease irritation from burns. Ointments is an essential part of the burn treatment plan as they aid decrease the burn from virus and keep the skin wet such that it heals soon. Itching is a very general difficulty for individuals who have injured their skin. Some Burn Ointments consist pramoxine and hydrocortisone to decrease scarring. Vitamin C is other organic ointment that can aid recover a burn. It enhances recovery by enhancing new cell development and strength. A small dosage of vitamin C daily can aid the body heal from an injury very fast. High dosage can aid recover a severe burn. Other organic ointments that may aid burns recover consist propolis, which is a gum prepared from the bees to create their hives, and lavender oil. Several survey is required to identify whether these ointments are effective. Gastritis Treatment is based on the particular cause. Short-term gastritis is occurred by nonsteroidal anti-inflammatory medicines or alcohol may be released by inhibiting the usage of those particles. Medicines utilized to cure gastritis comprise of H. pylori in the assimilation tract, the physician might suggest a mixing of antigens, such as clarithromycin and amoxicillin or metronidazole to destroy the bacteria. The main advantages of Gastritis Treatment is to decrease the pain and heartburn occurred by the infection in the stomach lining. It also decreases the threat of progressing stomach tumor and other side-effects. Gastritis is very usually occurred by a bacterium known as H pylori, which can be detected utilizing breath, plasma, stool, and immunological experiments. Other factors of gastritis comprise a number of infectious problems and drugs that leads to irascibility to the stomach liner. Some gastritis prodromes can be cured with specific lifestyle alterations such as ignoring smoking, decreasing intake of alcohol, consuming acid decreasing drugs, and reducing stress. One should ensure to take the full antigen prescription, generally for one or two weeks, along with medicines to obstruct acid production. Once cured, the physician will retest one for H. pylori to ensure it has been damaged. Drugs that stop acid production and enhance healing. Proton pump inhibitors decrease acid by stopping the action of the parts of cells that generate the acid. These medicines comprise the medicine and OTC drugs omeprazole, lansoprazole, rabeprazole, pantoprazole and others. Persistent usage of proton pump inhibitors, especially at high dosage, might enhance the threat of hip, wrist and spine fractures. One should consult the physician whether a calcium supplement may decrease this threat. Drugs to decrease acid production. Acid blockers — also called histamine (H-2) blockers — reduce the creation of acid released into the assimilation tract, which decreases gastritis pain and enhances recovery. Accessible by prescription or OTC, acid blockers comprise famotidine, cimetidine and nizatidine. Drugs that stable the acid in stomach. The doctor might suggest an antacid in the drug regimen. Antacids stabilize the acid present in the stomach and can offer quick pain relief. Complications can comprise constipation or diarrhea, based on the main components. These aid with instant prodromes relief however are usually not utilized as a main therapy. Proton pump inhibitors and acid inhibitors are very efficient and have less complications. As per U.S pharmacists around 8 in 1,000 people suffer from sudden gastritis in U.S. It is essential to reminisce to keep a food diary and attempt to optimize the consumption of foods that may exasperate the stomach lining, such as peppery or fatty foods. A physician can suggest OTC or prescription drugs to decrease the prodromes of gastritis. These drugs decrease the quantity of acid that the stomach creates, which can decrease the prodromes and enhance the body to recover itself. The physician may suggest taking a dietary additive that comprises probiotics, which can aid refill digestive flora and enhance recovery of gastric ulcers. These additives can be consumed orally, in tablet form or by drinking them with liquid. Urinary Tract Infections (UTIS) are a common medical condition affecting millions of people each year. These infections are caused by bacteria that enter the urinary tract and can cause a variety of symptoms such as frequent and painful urination, fever, and lower abdominal pain. UTIs can affect any part of the urinary tract, including the bladder, urethra, and kidneys. Fortunately, UTIs are treatable, and there are a variety of effective treatment options available. The first step in treating a Urinary Tract Infections is to confirm the diagnosis. This usually involves a urine test to check for the presence of bacteria in the urine. Once the diagnosis is confirmed, the next step is to choose an appropriate treatment option. The choice of treatment will depend on a variety of factors, including the severity of the infection, the patient's medical history, and any underlying health conditions. The most common Urinary Tract Infections Treatment for a UTI is antibiotics. Antibiotics work by killing the bacteria that are causing the infection. The choice of antibiotic will depend on the specific type of bacteria that is causing the infection. Common antibiotics used to treat UTIs include nitrofurantoin, trimethoprim-sulfamethoxazole, and ciprofloxacin. These antibiotics are usually taken orally for a period of three to seven days, depending on the severity of the infection. In addition to antibiotics, there are other treatments that can be used to help manage the symptoms of a UTI. Urinary Tract Infections Treatment may include pain relievers to alleviate the pain and discomfort associated with the infection, and anti-inflammatory medications to reduce inflammation in the urinary tract. Patients may also be advised to drink plenty of fluids to help flush out the bacteria and reduce the risk of complications. In some cases, hospitalization may be required for the treatment of a UTI. This is usually only necessary in severe cases, where the infection has spread to the kidneys or other parts of the urinary tract. In these cases, intravenous antibiotics may be administered to help fight the infection more effectively. Prevention is also an important aspect of UTI treatment. Patients can take steps to reduce their risk of developing a UTI by practicing good hygiene, urinating frequently, and wiping from front to back after using the toilet. Women may also be advised to avoid using certain types of birth control, such as spermicidal agents and diaphragms, as these can increase the risk of developing a UTI. Urinary Tract Infections are a common medical condition that can cause a variety of symptoms and complications. However, with proper diagnosis and treatment, most UTIs can be successfully treated. Antibiotics are the most common treatment for UTIs, but other treatments may also be used to manage symptoms and reduce the risk of complications. Patients can also take steps to prevent UTIs by practicing good hygiene and taking other preventative measures. If you suspect that you have a UTI, it is important to seek medical attention promptly to ensure that you receive appropriate treatment. Polio, also known as poliomyelitis, is a highly infectious viral disease that attacks the nervous system and can cause paralysis or even death. The virus spreads from person to person through contact with fecal matter or contaminated food and water. Before the development of polio vaccines, the disease was a major global health threat, causing widespread outbreaks and leaving many children paralyzed for life. In the early 20th century, the polio virus began to spread rapidly, especially in industrialized countries where overcrowding and poor sanitation were prevalent. In the 1940s and 1950s, the United States experienced several large-scale polio epidemics, leaving thousands of children disabled or dead. The fear and panic caused by the disease led to the closure of public pools and movie theaters, and parents kept their children indoors to avoid exposure. The first Polio Vaccines was developed by Dr. Jonas Salk in the early 1950s, and it quickly became a breakthrough in the fight against the disease. Salk's vaccine used inactivated or "killed" polio virus to stimulate the body's immune system to build resistance to the disease. In 1955, a nationwide trial of the vaccine involving over 1.8 million children was conducted in the United States, and the results showed that the vaccine was highly effective in preventing polio. The vaccine was then made available to the general public, and cases of polio began to decline rapidly. Another type of Polio Vaccines was developed by Dr. Albert Sabin in the late 1950s. Sabin's vaccine used live, weakened polio virus, which could replicate in the intestines but not cause disease. This type of vaccine was easier to administer and provided longer-lasting immunity than the Salk vaccine. Sabin's vaccine was first used in the Soviet Union in 1959 and was widely adopted in the United States and other countries in the 1960s and 1970s. Thanks to the development of Polio Vaccines, the disease has been almost completely eradicated in many parts of the world. According to the World Health Organization (WHO), the number of polio cases has decreased by over 99% since the introduction of the vaccine. In 2020, there were only 22 reported cases of wild poliovirus worldwide, compared to 350,000 cases in 1988. Polio Vaccines have had a significant impact on global health, especially in developing countries where the disease is still endemic. In countries such as Pakistan, Afghanistan, and Nigeria, where polio is still a major health threat, vaccination campaigns have been organized to reach children in even the most remote areas. These campaigns involve health workers going door-to-door to administer the vaccine to every child under the age of five. Despite the challenges posed by conflict, insecurity, and vaccine hesitancy, these campaigns have helped to reduce the number of polio cases in these countries. Pulmonary Arterial Hypertension (PAH) is a rare and potentially life-threatening condition that affects the pulmonary arteries, which are the blood vessels that carry blood from the heart to the lungs. PAH is characterized by high blood pressure in the pulmonary arteries, which can cause the arteries to narrow, become stiff, or even completely block the flow of blood to the lungs. This can lead to a variety of symptoms, including shortness of breath, fatigue, chest pain, and swelling in the legs and ankles. Pulmonary Arterial Hypertension can be caused by a number of different factors, including genetic mutations, connective tissue disorders, HIV infection, and exposure to certain drugs or toxins. Although there is no cure for PAH, there are a number of different drugs that can help to manage the symptoms of the disease and improve quality of life. One type of Pulmonary Arterial Hypertension Drug commonly used to treat PAH is a class of medications known as pulmonary arterial hypertension drugs. These drugs work by dilating the blood vessels in the lungs, which helps to reduce the resistance to blood flow and decrease the workload on the heart. There are currently several different types of pulmonary arterial hypertension drugs on the market, each of which works in a slightly different way. Some of the most commonly used pulmonary arterial hypertension drugs include: Endothelin receptor antagonists (ERAs): These drugs work by blocking the action of endothelin, which is a hormone that constricts blood vessels. By blocking endothelin, ERAs help to dilate the blood vessels in the lungs and reduce blood pressure. Prostacyclin analogs: These drugs mimic the effects of prostacyclin, which is a naturally occurring hormone that helps to dilate blood vessels and prevent blood clots. By mimicking prostacyclin, prostacyclin analogs help to reduce blood pressure and improve blood flow to the lungs. Phosphodiesterase type 5 inhibitors (PDE5 inhibitors): These drugs work by blocking the action of an enzyme called phosphodiesterase type 5, which breaks down cyclic guanosine monophosphate (cGMP). cGMP is a molecule that helps to relax smooth muscle cells in the blood vessels, which in turn helps to dilate the vessels and improve blood flow. Soluble guanylate cyclase stimulators (sGC stimulators): These drugs work by stimulating the production of cGMP, which helps to relax smooth muscle cells in the blood vessels and improve blood flow. Calcium channel blockers: These drugs work by blocking the entry of calcium into the smooth muscle cells in the blood vessels, which helps to relax the cells and reduce blood pressure. In addition to these medications, there are also a number of other drugs that can be used to manage the symptoms of PAH, such as diuretics to reduce fluid buildup in the body, anticoagulants to prevent blood clots, and oxygen therapy to improve breathing. Explore More- https://www.prnewswire.co.uk/news-releases/global-pulmonary-arterial-hypertension-drug-market-to-surpass-us-11-220-2-million-by-2030-coherent-market-insights-873440607.html |
Categories
All
|