|
In recent years, the demand for sustainable and environmentally friendly solutions in various industries has grown exponentially. Amidst this shift, butyric acid, a naturally occurring compound, has emerged as a promising alternative for addressing several industrial challenges. Butyric Acid, also known as butanoic acid, is a short-chain fatty acid found in various natural sources, including certain bacteria, dairy products, and plant oils. This versatile organic compound possesses unique properties that make it an ideal candidate for overcoming challenges in diverse industrial sectors. Butyric acid is widely utilized as a flavoring agent and preservative in the food and beverage industry. Its distinct odor and taste contribute to the characteristic flavor profiles of many dairy products, such as cheese and butter. Additionally, butyric acid inhibits the growth of harmful bacteria, thereby extending the shelf life of food products naturally. The pharmaceutical industry has recognized the value of Butyric Acid in the production of drugs and therapies. It serves as a precursor in the synthesis of various pharmaceutical compounds, including esters, salts, and derivatives. Butyric acid has shown potential in cancer treatment, as it exhibits antitumor effects and can promote apoptosis (programmed cell death) in cancer cells. As a feed additive, butyric acid enhances the overall gut health and performance of livestock. It improves nutrient absorption, strengthens the intestinal barrier, and reduces the occurrence of gastrointestinal disorders. By incorporating butyric acid into animal feed, farmers can enhance the overall health and well-being of their livestock while reducing the need for antibiotics. Butyric Acid serves as a vital component in the production of biofuels and bioplastics. Through a process called anaerobic fermentation, butyric acid can be converted into butanol, a promising biofuel that exhibits higher energy density than ethanol. Additionally, butyric acid can be polymerized to create biodegradable plastics, offering an eco-friendly alternative to traditional petroleum-based plastics. One of the significant challenges faced by industries is the remediation of contaminated sites. Butyric acid, with its unique properties, can aid in the process of environmental cleanup. It can be employed to stimulate the growth of certain bacteria that possess the ability to degrade pollutants, such as hydrocarbons and heavy metals, naturally. This bioaugmentation technique offers a sustainable and cost-effective solution for soil and water remediation.
0 Comments
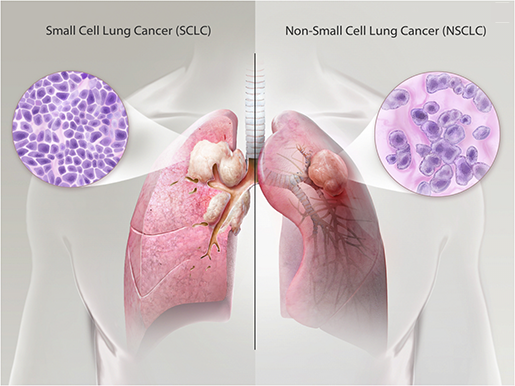
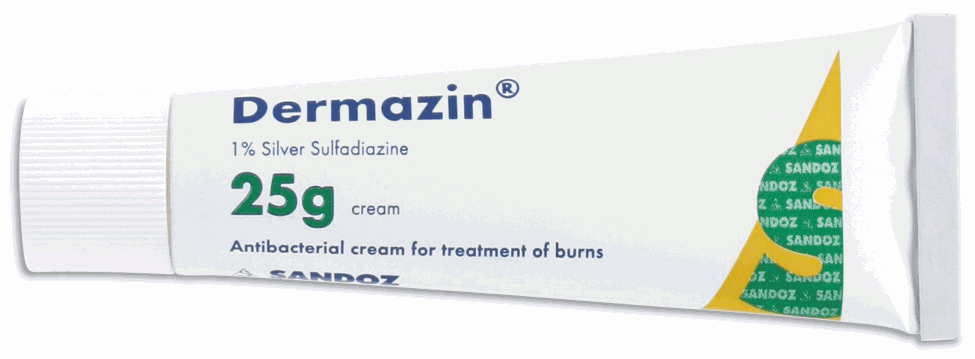
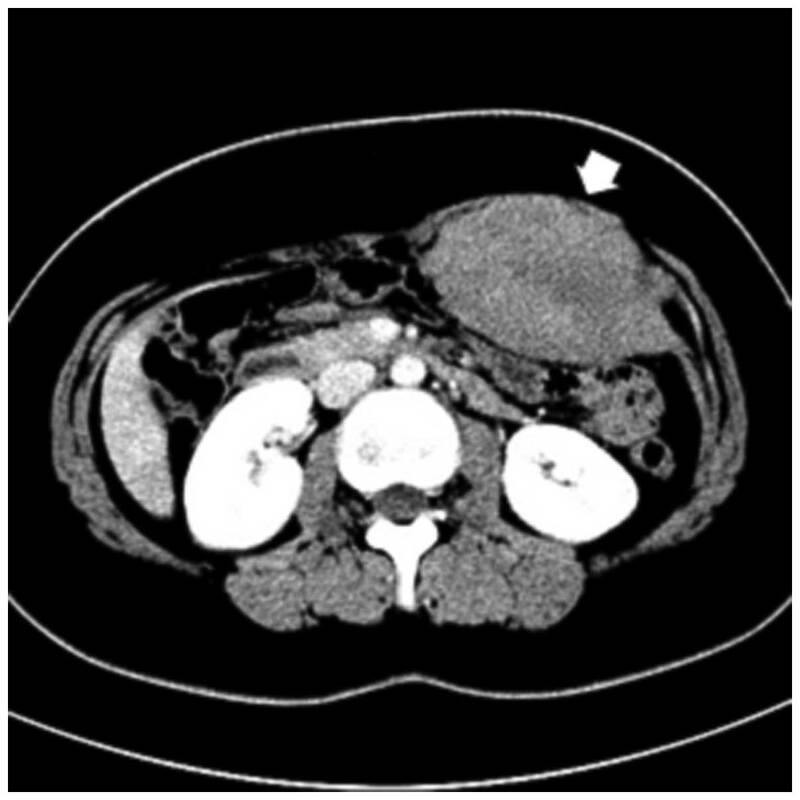
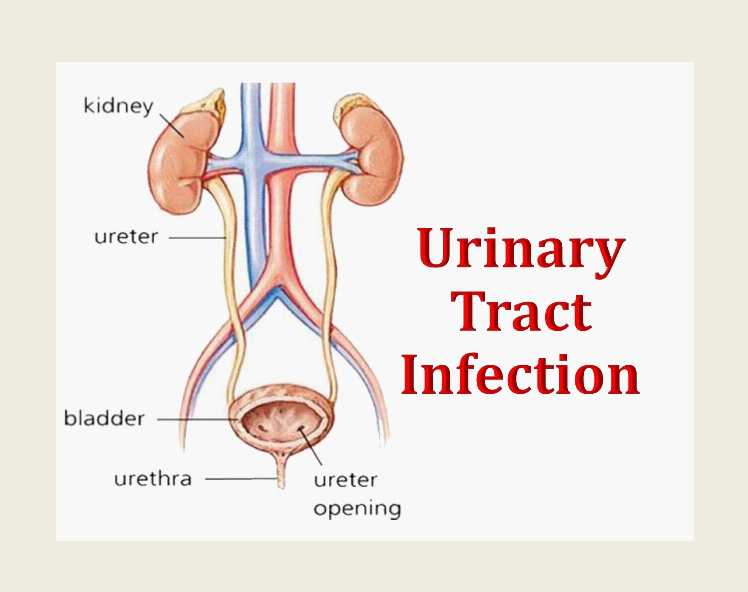
Lung cancer is when abnormal cells grow in the lungs. It can spread to other areas of the body and cause different symptoms. Small cell and non-small cell are types of lung cancer. Non-Small Cell Lung Cancer starts in the flat cells that line the airways and can grow quickly. It is often caused by smoking. Chemotherapy uses drugs to kill cancer cells. It can be used at different times in treatment to achieve different goals, such as shrinking the tumor before surgery or killing leftover cancer cells after surgery. It can also be given alone or to control symptoms and side effects. Squamous cell and adenocarcinoma carcinoma are the most common. They usually grow more slowly than other types of lung cancer and are less likely to spread to other parts of the body. Some people with Non-Small Cell Lung Cancer have a device surgically implanted in their chest, either a pump, catheter or port to give them chemotherapy through a tube called a vein (intravenous or IV) directly into the bloodstream. Other people take chemotherapy pills by mouth. Survival rates for NSCLC vary widely based on a number of factors, including the person’s age and general health, the type of cancer and how it is treated. Statistics only provide averages and can’t tell whether cancer will shorten their life or not. The cancer drugs in targeted therapy interfere with the molecular abnormalities that drive tumor growth. They can also deliver toxins that kill cancer cells without harming healthy cells. Doctors may recommend this treatment if the results of the biopsy show certain genetic changes. NYU Langone’s Perlmutter Cancer Center has a variety of targeted therapies to treat lung cancer, including small-molecule drugs that block specific proteins that help tumors grow. Other targeted drugs, known as angiogenesis inhibitors, starve the tumor by blocking its ability to make new blood vessels that bring it nutrients. Targeted therapy can be used alone or in combination with surgery, radiation, and chemotherapy. It can lower the chances of cancer coming back after surgery. Immunotherapy uses the body’s immune system to fight cancer. A care team may recommend immunotherapy alone or in combination with chemotherapy and/or radiation therapy. Scientists make drugs in the lab to help the immune system find and kill cancer cells more easily. Some of these drugs, called monoclonal antibodies, block checkpoint molecules like CTLA-4 and PD-L1 that prevent the immune cells from attacking cancer cells. Other monoclonal antibodies carry a drug or radioactive substance that targets specific markers (called antigens) on cancer cells. Still others, known as bi-specific T cell-engaging antibodies, bind to both cancer cells and the immune system’s T cells, which helps the body attack the tumor more effectively. Immunotherapy doesn’t work for everyone, and it takes time to see results. Sometimes, a doctor may prescribe a cancer vaccine to help build an immune response. Other times, they may test the blood or tissue for specific markers that are high in cancer cells and can be targeted with immunotherapy. Surgery isn’t usually used for this type of cancer as it often spreads too far by the time doctors find it. If cancer is found very early, doctors may suggest an operation called a lobectomy or pneumonectomy to remove part of the lung. This is followed by chemotherapy or radiotherapy to destroy any remaining cancer cells. Adenocarcinoma is found in the outer area of the lung; squamous cell carcinoma, which is found in the center of the lung near an air tube (bronchus); and large cell carcinoma, which can occur anywhere in the lungs. Non-Small Cell Lung Cancer cancers grow and spread more slowly than small cell lung cancer. You can Also Read the Press Release of Non-Small Cell Lung Cancer Silver Sulfadiazine is an antiseptic gel that is utilized to aid inhibit and cure inflammation occurred by second- or third-degree wounds. It destroys a vast variety of bacteria, and one generally use it directly to the burn injury. It is often used for other purposes, before using Silver sulfadiazine one should consult to the physician. Silver sulfadiazine is used on the skin one or twice in a day. One is advised to wash the hands before applying it and after using it. One should put it on clean, debrided burn injuries, eluding the periocular region and mucosal regions. A layer around 1/16" thick should totally cover the burned skin. This medicine may be used to the infected skin even if it is coated with other dressing, such as a gauze binding. It is essential to utilize this drug for the complete length of time suggested, as skipping dosages enhances the threat of inflammation that is resistive to antigens. It is not yet clear regarding the proper usage of the medicine, however it is known that Silver Sulfadiazine inhibits the development of bacteria that contaminate a burn. The antigen action of the sulfadiazine combines to the imidazole, sulfhydryl, amino, amide, and carboxyl class of the bacteria, leading protein denaturation and enzyme prevention. Hardly, critical allergic reactions to this medicine takes place, such as life-threatening conditions such as Stevens-Johnson syndrome or anaphylaxis. One should get emergency clinical help if one suffers from hives; breathlessness; bulging of the face, lips, tongue, or esophagus; or if one has any other severe complications. One should tell the physician regarding the symptoms one is suffering from or regarding the allergy being caused due to the usage of other kinds of medicines. Silver Sulfadiazine is an efficient antimicrobial medicine that aids regulate inflammation in burned injuries. It inhibits germs from polluting the open injury and decreases the possibility of transmitting the bacteria into the plasma and causing serious inflammation. Silver Sulfadiazine gel is a topical medicine that is utilized as an adjunctive therapeutic for bacterial prophylaxis in individuals with incomplete and full-thickness wounds. It destroys bacteria, such as gram-positive and gram-negative organisms, and also stops the development of yeast and molds. The bactericidal action of the medicine is extracted from its contact with silver ions and sulfadiazine. It is used as a topical bandage to the injured area one or two times per day and reused as directed by a clinical provider. It is most generally utilized in combination with other topical therapeutics to minimize wound recovery, such as hydrocolloid coverings, granular gauzes and polyurethane exfoliators for negative pressure injury therapy. It is usually put to clean, dry skin that has been cleansed with soap and water. It should not be utilized to cure open injuries that are diseased or wet. This drug is not suggested for gravid women or kids below two months of age as it may lead to problems in the unborn baby. It is also not recognized whether this drug flows into breast milk, so it should be ignored by curing mothers. It is essential to follow the using instructions completely as suggested by the physician orderly to avoid complications, such as a rash or greyish skin yellowing. There are several drawbacks of Silver Sulfadiazine. There are several conflicting data in the silver sulfadiazine regarding the efficacy and protection of this treatment. It is essential to be aware of the limits of this and other procedures, particularly with comparison to negative pressure wound therapy, which has been known to increase recovery of unclean injuries while stopping unwanted silver exposure and optimizing antibiotic resistivity. Additionally, Silver sulfadiazine was capable to reduce established biofilms as contrasting to simply interrupt them. Desmoid Tumors Can Cause Pain, Restrict Movement And Also Obstruct Vital Nerves And Blood Vessels19/5/2023 Desmoid Tumors can grow almost anywhere in the body. They can press against blood vessels and nerves, causing pain, a limp ors problems using legs, feet, arms or hands. Doctors diagnose a desmoid tumor by taking a sample of the mass and looking at it under a microscope. They may also use imaging scans such as magnetic resonance imaging or computerized tomography to find the size and location of the tumor. A desmoid tumor can be diagnosed by physical examination, imaging scans, and a biopsy. The biopsy is a procedure where a small sample of the tumor is removed and looked at under a microscope. Desmoid Tumors can grow anywhere in the body, whereas most often they are found in the shoulder girdle and abdominal wall. They can cause pain and limit movement in the area around them. Desmoid tumors can also obstruct vital nerves and blood vessels. Some desmoid tumors grow very slowly or even shrink without treatment. If they are small and outside the abdomen, doctors may recommend a wait and watch approach. If they are inside the abdomen, doctors can use radiation to destroy the tumor cells. Doctors are also exploring new drugs to shrink or destroy desmoid tumors. These tumors are benign and don't spread, most of the time they don't cause symptoms. Whereas if the tumors grow too large and press against blood vessels, nerves or other tissues, they can cause pain, loss of function, and other health problems. It's not clear what causes desmoid tumors to form, they seem to be linked to changes in a gene called CTNNB1. They often start during or after pregnancy. They also may be associated with a genetic condition called familial adenomatous polyposis, which can lead to colon cancer. Most Desmoid Tumors can be watched with a procedure called active monitoring. This involves regular MRI or CT scans to watch for changes. Treatment options include medication, radiation therapy, cryoablation and surgery. Orthopedic and plastic surgeons have expertise in limb-saving surgery for these tumors, and are constantly working to improve outcomes. Some desmoid tumors grow very slowly and may not need treatment at all. In other cases, the doctor will monitor the tumor and recommend treatment if it grows or causes symptoms. Desmoid tumors can be difficult to remove as they often encapsulate and intertwine with surrounding tissues. This makes it hard for surgeons to identify the outer boundary of the tumor during surgery. Due to this, desmoids have a high rate of recurrence after surgery. Desmoid Tumors can be treated with surgery, chemotherapy, radiation therapy or cryoablation. Cryoablation uses extreme cold to kill cancerous cells and can be used in combination with surgery. Chemotherapy uses drugs that are taken orally or intravenously to shrink or kill cancerous cells. Some of these drugs have long-term side effects. Some promising new medications such as a gamma-secretase inhibitor are showing promise in treating desmoid tumors by slowing their growth. Desmoid tumors can sometimes shrink without treatment, a process that is known as quiescent. Depending on the individual case, desmoid tumors can be monitored with frequent MRI scans to see if they continue to grow or if they start causing symptoms. If the tumor grows or causes symptoms, doctors may then decide to move toward more intensive treatment options such as surgery. It can be difficult to treat a Desmoid Tumors as it is not well encapsulated and it often intertwines with the limb’s nerves, blood vessels and other tissues. This leads to a high rate of local recurrence after surgery ranging from 25-68%. Several nonsurgical treatments have been used for desmoid tumors, including radiofrequency ablation and cryoablation. Urinary Tract Infections (UTIs) are one of the most common types of bacterial infections that affect the urinary system. They occur when bacteria invade the urinary tract, leading to inflammation, pain, and discomfort. UTIs can be caused by different types of bacteria, including Escherichia coli (E. coli), Klebsiella pneumoniae, and Proteus mirabilis, among others. Although UTIs are not life-threatening, they can cause significant discomfort and can lead to complications if left untreated. Therefore, timely and appropriate urinary tract infection therapeutic is essential for the management of UTIs. There are several effective Urinary Tract Infection Therapeutics available. The most common urinary tract infection therapeutics are antibiotics, which work by killing the bacteria causing the infection. However, due to the rise of antibiotic-resistant bacteria, it is essential to use antibiotics judiciously and only when necessary. The therapeutic approach to UTIs depends on several factors, including the severity of the infection, the age and overall health of the patient, and the type of bacteria causing the infection. In general, UTIs can be treated with antibiotics, which are medications that kill or inhibit the growth of bacteria. However, the choice of antibiotic depends on several factors, such as the patient's age, underlying medical conditions, and the local resistance patterns of bacteria. The most common antibiotics used for Urinary Tract Infection Therapeutics include trimethoprim-sulfamethoxazole (TMP-SMX), nitrofurantoin, fosfomycin, and ciprofloxacin. TMP-SMX is a combination antibiotic that is effective against many types of bacteria, including E. coli. It is often used as a first-line urinary tract infection therapeuticfor uncomplicated UTIs, but it is not effective against all bacteria that cause UTIs. Nitrofurantoin is another antibiotic that is commonly used for the treatment of UTIs. It is especially effective against E. coli, and it has few side effects. However, it is not effective against other types of bacteria that cause UTIs, and it should not be used in patients with renal insufficiency. Urinary Tract Infections (UTIs) are common bacterial infection that affects millions of people worldwide each year. Timely urinary tract infection therapeutic is necessary to avoid these issues. While both men and women can develop UTIs, women are more likely to experience them due to their anatomy. UTIs are typically caused by bacteria, and the most common type of bacteria responsible for UTIs is Escherichia coli (E. coli). Symptoms of UTIs include pain or burning during urination, frequent urination, cloudy or strong-smelling urine, and pelvic pain. If left untreated, UTIs can lead to more serious complications such as kidney damage and sepsis. Antibiotics are the most commonly prescribed Urinary Tract Infection Therapeutics. The type of antibiotic prescribed will depend on the type of bacteria causing the infection. Common antibiotics used to treat UTIs include trimethoprim-sulfamethoxazole, nitrofurantoin, and fosfomycin. It is important to complete the full course of antibiotics as prescribed, even if symptoms improve before the medication is finished. Failure to complete the full course of antibiotics can lead to the development of antibiotic-resistant bacteria. Some studies have shown that cranberry juice can help prevent UTIs by preventing bacteria from attaching to the urinary tract lining. While cranberry juice may be effective in preventing UTIs, it is not a recommended urinary tract infection therapeutic for treating an active UTI. Where there no cure currently for pulmonary arterial hypertension, several varied drugs and process can decrease prodromes and enhance the life expectancy. The physician will operate with the individual to find the correct therapeutic plan for individual requirements. Drugs that decrease the blood pressure in the pulmonary are known as vasodilators. These can be consumed orally, inoculated or gulped. A general kind of vasodilator is epoprostenol. It is generally injected from an intravenous method linked to a pump that one uses on the belt or shoulder. Other Pulmonary Arterial Hypertension Drug for Pulmonary Arterial Hypertension comprise diuretics, which aid the cardiac and pulmonary function better. These drugs might be consumed once or two times in a day. One will require to get frequent blood tests to observe for dehydration, low BP, chemical disparities in the plasma, and renal difficulties. Several drugs are utilized to cure HIV and other inflammations have been associated to the growth of PAH in some individuals. Some instances of this comprise rituximab, sofosbuvir, nelfinavir, and cyclosporine. Tiny molecule tyrosine kinase inhibitors are the medicines that are created to inhibit the breakdown of specific chemicals in the body that lead the blood vessels to contract. Carfilzomib, Nilotinib, ponatinib, and ruxolitinib are very well-established and recognized of these medicines. Medicines that impact serotonin metabolism are the Agents that mimic on serotonin catabolism have been associated to the growth of pulmonary high blood pressure in some individuals, though many of these medicines are no longer accessible across the globe. Atypical antipsychotics, SSR inhibitors, and lithium have been associated in some situations. Pulmonary arterial hypertension is a disorder in which the pulmonary small blood vessels narrow, resulting it tough for the cardiac to pump oxygen-poor plasma to the pulmonary. This pressures the right portion of the cardiac, which can result to cardiac arrest and other difficulties. For instance, as per AHA, above 350,000 individuals suffer from cardiac arrest in America. Some medicines suggested for individuals with Pulmonary Arterial Hypertension Drug are thought to have several drawbacks. For instance, the anticoagulant warfarin may lead blood clots in individuals with pulmonary arterial hypertension and other problems that rise the threat of developing blood clots. Due to this, Warfarin should be utilized with caution and monthly observation of blood counts and functioning of liver tests is necessary. Calcium channel inhibitors, such as diltiazem and nifedipine are also often utilized for acute therapeutic of Pulmonary arterial hypertension, though they have lost some of their efficiency with time. These Pulmonary arterial hypertension drugs can be costly and need frequent observation and check-up of blood chemistry. Addition of Oxygen is other essential therapy for people with pulmonary aerial hypertension. This treatment leads the lungs to fill with oxygen, which aids relax the pulmonary arteries. Some individuals only need additional oxygen while they exercise or sleep, whereas others need it constantly. Pulmonary Arterial Hypertension is an inherited disorder classified by progressive, dangerous rise in the mean pulmonary arterial pressure. It is generally cured by a grouping of medicine and oxygen treatment to control the pressure and reduce symptoms. Numerous medications are accessible to enhance symptoms and decrease the development of Pulmonary arterial hypertension. These consist blood vessel dilators, such as epoprostenol, nifedipine and amlodipine; calcium channel inhibitors; a class of medicines known as phosphodiesterase 5 blockers; diuretics; and oxygen treatment. Blood vessel dilators, such as Flolan, are injected by Intravenous infusion. This is an efficient therapy for developed disorder however needs a significant assurance from the patient. The Pulmonary Arterial Hypertension Drug is pumped constantly through the Intravenous and must be combined on a daily basis. Utilizing oral drugs, such as nifedipine and amlodipine, may aid some people with developed pulmonary arterial hypertension, however enthusiasm for these therapeutics has reduced over the past few years. They are only utilized if other therapies have not been efficient or have less complications. Polio Vaccines and Future Generations: Safeguarding Health and Eradicating a Global Threat15/5/2023 Polio, short for poliomyelitis, is a highly infectious viral disease that primarily affects young children. It can lead to permanent paralysis and, in severe cases, death. For decades, polio posed a significant global health threat. However, thanks to the development and widespread administration of polio vaccines, the world has made tremendous progress in eradicating this disease. Polio outbreaks were once a global scourge, causing widespread panic and leaving a trail of devastation. Children were particularly vulnerable, with many facing a lifetime of disability. However, the introduction of Polio Vaccines in the mid-20th century revolutionized the fight against this disease. Vaccines, such as the inactivated polio vaccine (IPV) and the oral polio vaccine (OPV), have been instrumental in reducing the incidence of polio cases worldwide. Through vaccination campaigns, immunization drives, and global health initiatives, the burden of polio has significantly diminished. One of the most significant impacts of polio vaccines is their role in protecting future generations. By immunizing children and building their immunity against the poliovirus, vaccines ensure that upcoming generations are shielded from the threat of this debilitating disease. Vaccinations provide a robust defense, preventing polio from gaining a foothold in communities and disrupting young lives. Moreover, Polio Vaccines not only safeguard individual health but also contribute to the overall well-being of communities and societies. By preventing the transmission of the poliovirus, vaccines help establish herd immunity, where a sufficient proportion of the population is immunized to halt the circulation of the virus. This protective shield extends to those unable to receive vaccines, such as infants, individuals with weakened immune systems, or those living in regions with limited access to healthcare. Consequently, future generations can thrive in a polio-free environment, free from the threat of outbreaks and the associated burdens. The eradication of polio is an ambitious global goal, driven by the power of vaccines. Organizations like the World Health Organization (WHO), UNICEF, Rotary International, and the Bill & Melinda Gates Foundation have spearheaded efforts to eliminate polio from the face of the Earth. Through immunization campaigns, surveillance systems, and targeted interventions, these organizations have made significant strides towards achieving a polio-free world. The impact of eradicating polio goes far beyond the immediate benefits. By eliminating polio, we create a foundation for the better health of future generations. As resources previously allocated to polio eradication can be redirected towards other public health priorities, healthcare systems becosme stronger and more resilient. This broader health infrastructure will serve as a lasting legacy, benefitting future generations by improving access to healthcare, strengthening disease surveillance, and bolstering response capabilities. Due to the increased zoonotic disease incidence, rising pet ownership, and expanding animal adoption globally, the market for Veterinary Medicine is expanding rapidly. Additionally, it is anticipated that rising veterinary medicine demand and increased attention to veterinary healthcare will fuel market expansion. However, factors including strict regulatory requirements and a shortage of veterinarians are anticipated to impede market expansion. While remarkable progress has been made in the fight against polio, challenges remain. Polio's eradication necessitates addressing barriers such as reaching remote populations, addressing vaccine hesitancy, and maintaining high vaccination coverage rates. It requires sustained commitment, financial resources, and collaboration among governments, healthcare professionals, and communities. In the pursuit of a polio-free world, innovation plays a crucial role. Advancements in vaccine technology, surveillance systems, and outbreak response capabilities are essential to overcoming the remaining obstacles. Epilepsy is a chronic neurological disorder characterized by recurrent seizures, affecting millions of people worldwide. Anti-Epileptic Drugs (AEDs) play a crucial role in controlling seizures and improving the quality of life for individuals with epilepsy. Over the years, significant advancements have been made in the field of AEDs, leading to the development of novel drugs and innovative treatment approaches. One of the recent breakthroughs in AEDs is the concept of personalized medicine. Researchers are now exploring the use of pharmacogenomics, a field that studies how an individual's genetic makeup influences their response to drugs. By analyzing genetic variations, researchers can predict a patient's drug response and determine the most effective Anti-Epileptic Drugs with minimal side effects. This tailored approach enables physicians to optimize treatment plans and minimize the trial-and-error process, ensuring better seizure control and improved patient well-being. Advancements in our understanding of the molecular mechanisms underlying epilepsy have paved the way for targeted therapies. Researchers are identifying specific molecular targets involved in seizure generation and propagation, allowing the development of drugs that selectively act on these targets. For example, drugs that modulate ion channels, receptors, or neurotransmitter systems involved in epilepsy pathogenesis are being investigated. These targeted therapies aim to enhance efficacy while reducing adverse effects associated with non-selective drugs, thereby improving the overall tolerability and effectiveness of AEDs. Researchers are also exploring innovative drug formulations to improve drug delivery and patient compliance. Novel drug delivery systems such as long-acting injectables, transdermal patches, and implantable devices offer sustained release of Anti-Epileptic Drugs, ensuring a consistent therapeutic level in the body and reducing the frequency of dosing. These formulations can be particularly beneficial for patients with poor medication adherence, helping them achieve better seizure control and minimizing the risk of breakthrough seizures. In addition to traditional AEDs, non-pharmacological approaches are gaining attention as complementary or alternative treatments for epilepsy. Neurostimulation techniques, such as vagus nerve stimulation (VNS), deep brain stimulation (DBS), and responsive neurostimulation (RNS), have shown promising results in controlling seizures in patients who do not respond well to medications. Additionally, ketogenic diet therapies, which involve a high-fat, low-carbohydrate diet, have demonstrated effectiveness in reducing seizure frequency, particularly in children with epilepsy. These non-pharmacological interventions expand the treatment options available to patients, offering new avenues for seizure management and improving overall outcomes. Obesity and overweight are primarily caused by an imbalance in energy between calories consumed and calories burned. In light of this, the prevalence of overweight and obesity among kids and teenagers aged 5 to 19 has increased significantly, which is anticipated to fuel the growth of the global Anti-Obesity Drugs market over the coming years. For instance, 39 million children under the age of five were overweight or obese in 2020, according to a World Health Organisation report released in June 2021. The integration of technology into epilepsy management has opened up new possibilities for monitoring, predicting, and preventing seizures. Wearable devices, such as smartwatches and seizure detection devices, equipped with sophisticated algorithms, can detect physiological changes associated with seizures in real-time. This enables timely interventions, such as alerting caregivers or initiating responsive neurostimulation, to prevent seizure progression. Furthermore, advancements in neuroimaging techniques, such as functional magnetic resonance imaging (fMRI) and positron emission tomography (PET), provide valuable insights into the brain's activity during seizures, aiding in the development of targeted interventions. The latest innovations in anti-epileptic drugs hold great promise in revolutionizing seizure management and improving the lives of individuals with epilepsy. The first step in Hyperkalemia Treatment is to identify and treat the underlying cause. Hyperkalemia can be caused by a variety of factors, including kidney disease, certain medications, and adrenal gland disorders. If the condition is caused by a medication, the medication may need to be discontinued or the dosage adjusted. If the condition is caused by kidney disease, treatment may involve dialysis or medications to improve kidney function. Once the underlying cause has been identified and treated, the level of potassium in the blood will often decrease. Hyperkalemia is a medical condition in which the level of potassium in the blood is higher than normal. This can be a serious health issue, as high levels of potassium can lead to muscle weakness, irregular heartbeat, and in severe cases, cardiac arrest. Treatment for hyperkalemia involves managing the underlying cause of the condition, as well as lowering the level of potassium in the blood. In this article, we will discuss the different treatment options for hyperkalemia. Hyperkalemia is a medical condition in which the level of potassium in the blood is higher than normal. Potassium is an essential electrolyte that is important for normal bodily functions such as muscle contractions and the functioning of the heart. However, if the level of potassium in the blood becomes too high, it can lead to serious health problems such as irregular heartbeat, muscle weakness, and in severe cases, cardiac arrest. Hyperkalemia can be caused by a variety of factors, including kidney disease, certain medications, adrenal gland disorders, and other medical conditions. Hyperkalemia Treatment involves managing the underlying cause of the condition, as well as lowering the level of potassium in the blood through dietary changes, medications, and in severe cases, dialysis. Patients with hyperkalemia are often advised to restrict their dietary intake of potassium. Foods that are high in potassium, such as bananas, oranges, and potatoes, should be avoided or consumed in small amounts. Patients may also need to avoid salt substitutes that contain potassium chloride. Several medications are available to help with Hyperkalemia Treatment. These medications work by either increasing the excretion of potassium from the body or by shifting potassium from the bloodstream into the cells. Some of the most commonly used medications for hyperkalemia include: Calcium gluconate is a medication that can help to protect the heart from the effects of high potassium levels. It does not lower the level of potassium in the blood, but it can help to prevent the heart from becoming too sensitive to the effects of high potassium levels. Sodium polystyrene sulfonate is a medication that can help to lower the level of potassium in the blood by binding to potassium in the intestines and removing it from the body through the stool. It is used as a popular hyperkalemia treatment. Diuretics are medications that increase urine production, which can help to remove excess potassium from the body. Insulin and glucose can be used to help shift potassium from the bloodstream into the cells. This can help to lower the level of potassium in the blood. In severe cases of hyperkalemia treatment, dialysis may be necessary to remove excess potassium from the body. Dialysis involves the use of a machine that filters the blood and removes excess potassium, as well as other waste products, from the body. Hyperkalemia is a serious medical condition that requires prompt treatment. Hyperkalemia Treatment involves managing the underlying cause of the condition, as well as lowering the level of potassium in the blood. Patients with hyperkalemia may need to restrict their dietary intake of potassium, take medications to lower potassium levels, or undergo dialysis. Preventing hyperkalemia involves avoiding foods that are high in potassium, monitoring potassium levels regularly, and following prescribed medication regimens. Cluster Headache are a sequence of regular, strongly painful shocks that take place for weeks or several months on a single go. The headache generally takes place for around 15 minutes to 3 hours and are during that time and individual may also experience vomiting, light sensitivity, and vertigo. They are generally very probable and are known to be associated to the body’s heartbeat, a 24-hour clock that reacts to sunlight. Individuals are known to get their Headache at the same duration daily and often even while sleeping at night. Cluster Headache treatment is focused at managing pain after an attack and decreasing the severity of attacks one experiences with time. The physician might suggest medicines that act on brain impulse, such as sumatriptan and verapamil. A pain medication that mimics on blood vessels to decrease can also aid, and it can be coupled with oxygen treatment carried through a face mask or nasal oxygen for 15 minutes once. Corticosteroids are other kind of drugs that can aid, however they are required to be consumed daily. If medicines are not effective and don’t decrease the aching, physicians might suggest operation to enhance the occipital nerve on one part of the cerebrum. This includes grafting an instrument through the occipital nerve and delivering signals with probes. Other method is TVNS. Transcutaneous vagus nerve stimulation includes utilizing a minute or tiny, handheld instrument to stimulate the vagus nerve, which passes from the front of the neck. It can be utilized prior a cluster headache or through an attack to decrease the necessity for medicines, and it can be efficient for some individuals. Dissimilar to migraine Headache, Cluster Headache are not threatful or risky for the individual’s life. However the pain can be extensively devastating and impact the quality of life. Therapy for cluster Headache aims on decreasing the pain while an attack starts, and on protective methods to reduce the frequency and time of attacks. Varied kinds of medicines are utilized to cure the Headache, and some individuals also get behavioral therapies. Preventive drugs, such as calcium channel inhibitors, melatonin, lithium carbonate, and topiramate aid decrease the time a person experiences headache in those who suffer from cluster Headache. A new inoculating medicine, CGRP monoclonal antigen, might be supportive for individuals who have irregular cluster Headache. Some causes of cluster Headache consist consumption of alcohol, a sudden rise in temperature, or working out in hot climate. In other conditions, the causes are a medical history of Cluster Headache in the family, or an underlying clinical problem, such as a brain cancer or a damaged blood vessel in the cranium. Smoking is a main cause for cluster Headache in smokers, and stopping it can aid decrease the headache. However smoking still rises the threat of Cluster Headache through active cluster duration, even if one stop. Oxygen therapeutic by breathing fresh oxygen with the help of a face mask is an efficient therapy for acute incidents of cluster Headache. Anyhow, in some individuals it only stops the attack by a few minutes or hours. The main drawbacks of cluster headache consist a high occurrence, absence of efficient therapeutic choices, and the considerable effect on quality of life. The disorder has also been associated to rising usage of illicit medicines and suicidal ideation. Apart from the drawbacks of cluster headache, there are some therapeutic options that may assist. These consist medicine that cures a cluster headache attack instantly, and preventive medicine that can decrease the threat of cluster headache. Fast-acting drug therapeutic are usually the best choice for instant treatment. Medicines such as triptans, octreotide, and local sedatives can be utilized for rapid relief of cluster headache pain. |
Categories
All
|