|
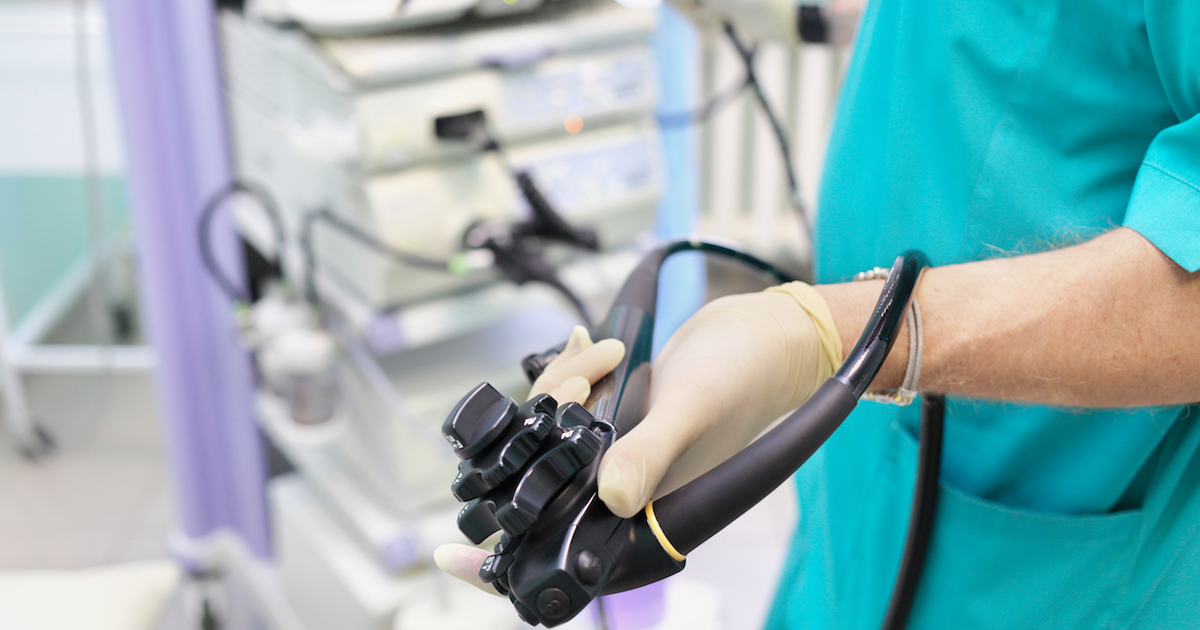
Automated Endoscope Reprocessors can help improve patient safety by automating the cleaning process. These machines can improve reprocessing efficiency and reduce the risk of cross-contamination. Plus, they can improve the consistency of the high-level disinfecting process. Some AERs include features that reduce the risk of contamination, such as automatic cycle starting, computerized cycle documentation, continuous leak testing during the cycle, and a large visual display. The AER can also include a barcode scanner for fast data entry. Automation can increase the efficiency of the reprocessing process by up to 50 percent. Aside from reducing costs, automated reprocessing may have a positive impact on financial performance. In China, for example, automated reprocessing can recover the capital investment within 14 months. In Russia, an Automated Endoscope Reprocessors can offset nearly all additional operating expenses. Furthermore, hospitals will save time and money by eliminating manual soaking. Moreover, Automated Endoscope Reprocessors may generate peracetic acid in situ. This acid is used to disinfect semi critical devices such as endoscopes. However, glutaraldehyde does not seem to be a significant risk to infection transmission. Nonetheless, continued clinical studies are necessary to confirm the findings. The findings suggest that automated endoscope reprocessors may be beneficial in treating many patients. While many benefits of an Automated Endoscope Reprocessors, it should be noted that the most effective ones should be able to meet strict standards. They should also be able to comply with the Healthcare Infection Control Practices Advisory Committee's guidelines, which are based on the best practices of the industry. The standards for automated endoscope reprocessors have been developed to address these issues. The FDA regulates the effectiveness of Automated Endoscope Reprocessors. This agency analyzes the clinical use of endoscopes and considers factors that might lead to infections. The agency also cooperates with manufacturers of endoscope reprocessors, and they are closely scrutinized. Moreover, the FDA considers the validation study protocol and test data that are provided by medical device manufacturers. There are still questions regarding the FDA's approval of AERs, and it is important to make sure that the product is safe before introducing it into practice. Automated endoscope reprocessors are an excellent option for reducing bacterial contamination. They also reduce the amount of clinically relevant pathogens. The high level of disinfection generated by these machines makes it an ideal option for reprocessing endoscopes. However, it is important to note that reprocessing is only an option for endoscopes used for gastrointestinal surgery. After the initial training, the staff members should review the instructions provided by the Automated Endoscope Reprocessors. These instructions should outline the correct way to use each step of the reprocessing process. The training should also address the cleaning process and sterilization of biopsy forceps. As the endoscope reprocessor is used in various surgical procedures, it is essential that each individual staff member receive ongoing training and competency assessment. Automated Endoscope Reprocessors can help prevent the spread of a hospital-acquired infection. Some automated endoscope reprocessors also monitor swab culture to ensure that no microbes are present. This ensures the quality of the process. A multidisciplinary team of endoscope reprocessing personnel should develop and implement the program to minimize infection risk. The team should include the infection prevention authorities, infection control specialists, and reprocessing personnel. If staffing is a concern, consider bringing in a third party to assist with the endoscope reprocessing process.
0 Comments
Leave a Reply. |
Categories
All
|