|
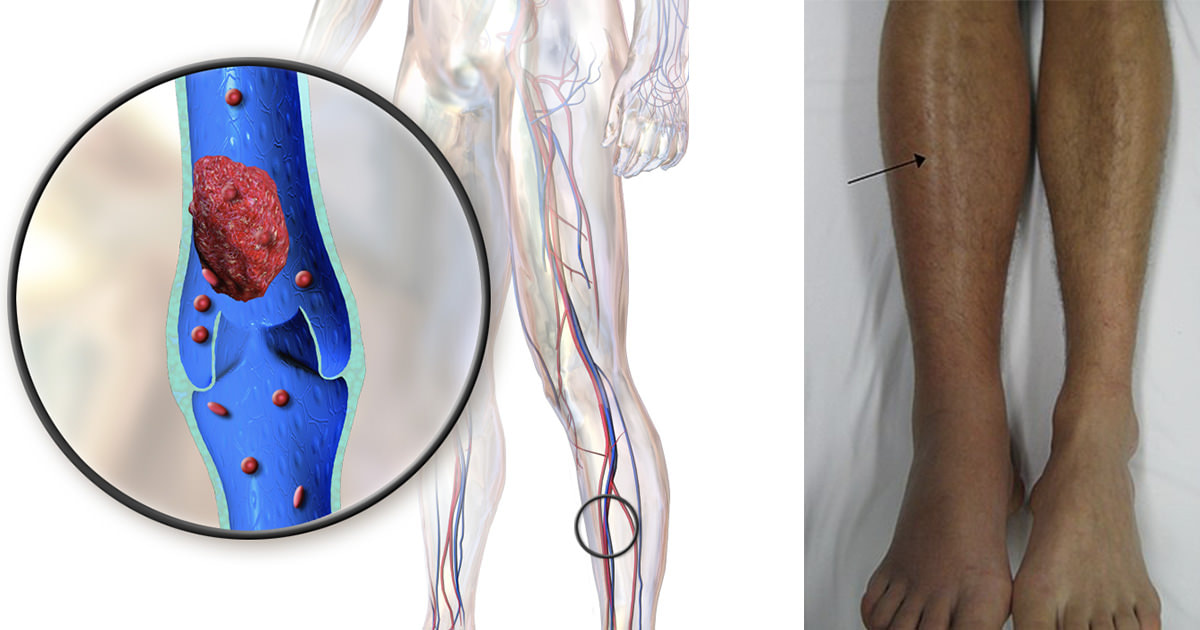
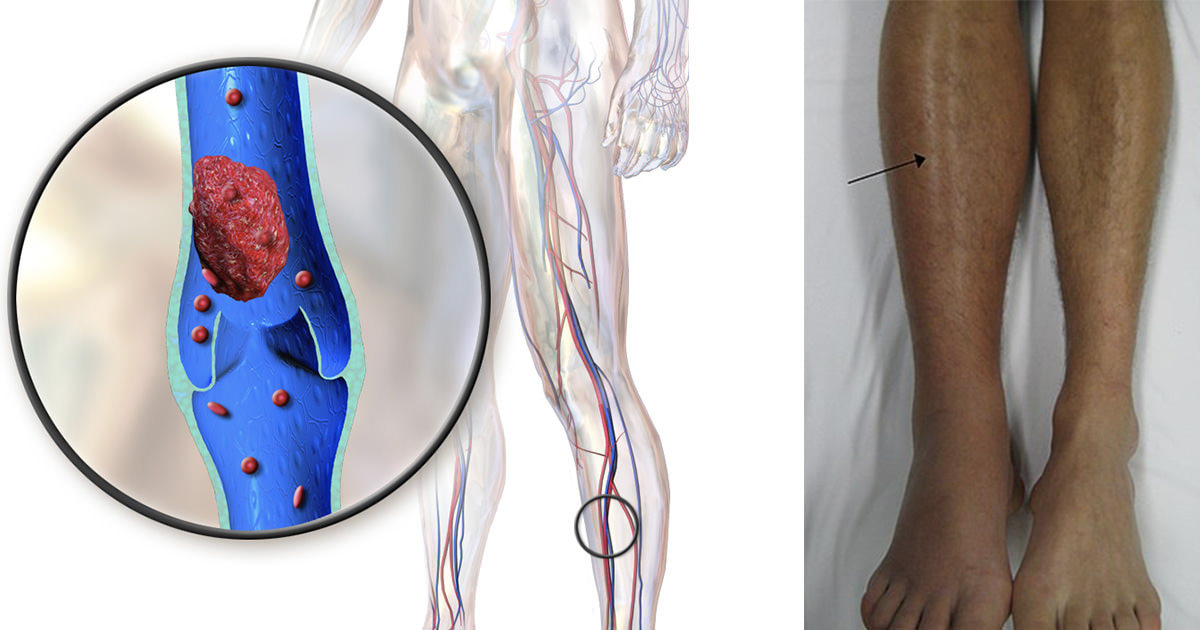
Venous Thromboembolism (VTE) is a medical condition characterized by the formation of blood clots, known as thrombi, in the veins. VTE is a serious and potentially life-threatening condition, as blood clots can dislodge and travel to vital organs, such as the lungs or the brain, causing severe damage or even death. There are two main types of Venous Thromboembolism (VTE): Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE). DVT occurs when a blood clot forms in a deep vein, usually in the legs or pelvis. PE, on the other hand, occurs when a blood clot travels to the lungs and blocks a pulmonary artery, which carries blood from the heart to the lungs. Venous Thromboembolism (VTE) is a relatively common condition, with an estimated incidence of 1 to 2 cases per 1000 people per year. The risk of developing VTE is higher in certain populations, such as individuals over 60 years of age, those with a history of VTE or cancer, pregnant women, and individuals with a genetic predisposition to blood clotting disorders. The development of Venous Thromboembolism (VTE) is often the result of a combination of risk factors. These can include:
The diagnosis of Venous Thromboembolism (VTE) usually involves a combination of clinical evaluation, imaging tests, and laboratory tests. Imaging tests, such as ultrasound or CT scans, can detect the presence and location of blood clots. Laboratory tests, such as D-dimer tests, can help confirm the presence of blood clots. The treatment of VTE typically involves anticoagulant therapy, which helps to prevent the formation of new blood clots and reduce the risk of existing clots traveling to other parts of the body. In some cases, more aggressive treatments, such as thrombolytic therapy or surgical intervention, may be necessary. Preventing VTE is an important goal, particularly in high-risk populations. Measures to prevent VTE can include:
Venous Thromboembolism (VTE) is a serious and potentially life-threatening medical condition that can result in the formation of blood clots in the veins. The risk factors and symptoms of VTE can vary, and early detection and treatment are crucial in managing this condition. Measures to prevent VTE should also be taken, particularly in high-risk populations.
0 Comments
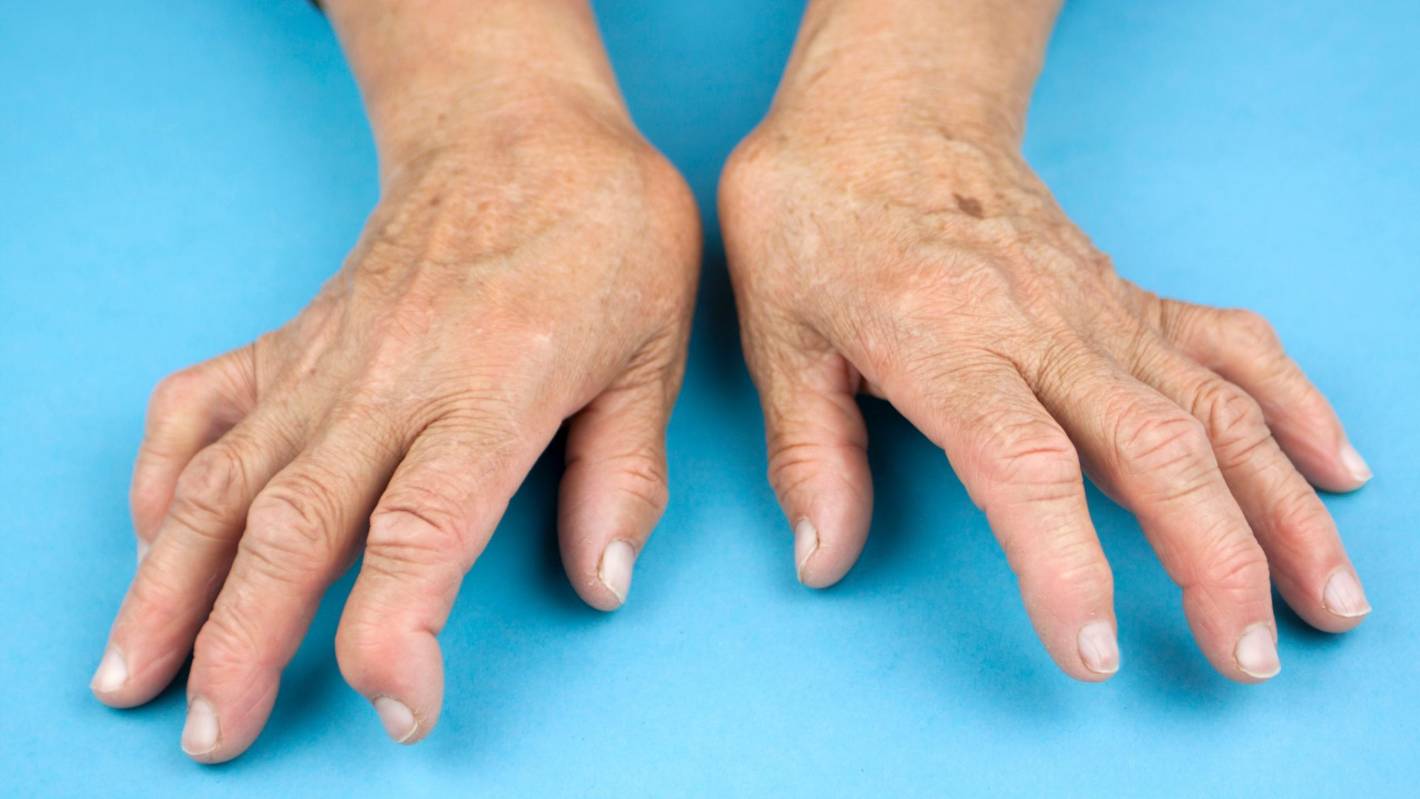
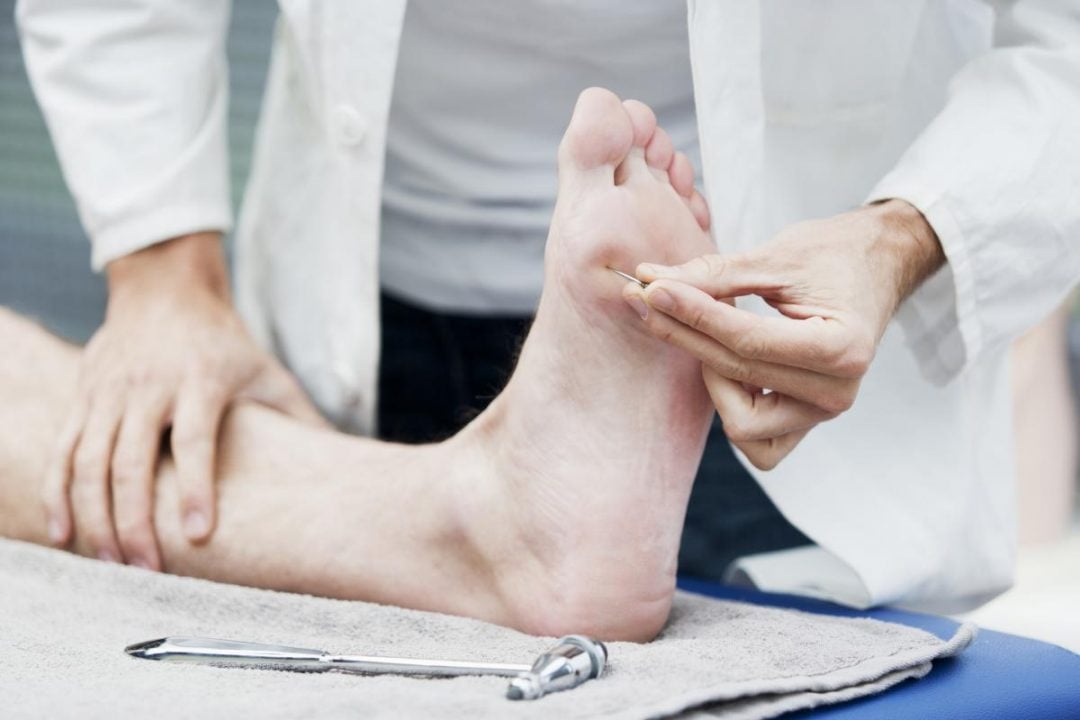
Vasculitis is an immunity disorder that results in infection of the blood vessels. This results in an enhanced threat of severe side effects such as a swelling or aneurysm that can be very risky for life. The main aim of the therapy is to manage the infection and control any fundamental situations that are generating the vasculitis. There are varied diverse kinds of drugs that can be utilized to cure vasculitis. Corticosteroid medicines, such as prednisone, are the most usual drug suggested for decreasing infection linked with vasculitis. Other medicinal therapeutics, such as immune-suppressing causes, are also accessible. The physician might suggest a mixture of these drugs for the best outcomes. Some kinds of vasculitis need persistent usage of these drugs, so it is essential to deliberate the Vasculitis Treatment plan cautiously with the physician and druggist. Other trials and processes that can aid examine vasculitis comprise X-rays, ultrasound, Chromatography or Magnetic Resonance Identification scans of the blood vessels and structures that are impacted. These are protective and painless trials that take around 15 minutes to one hour. A distinctive X-ray known as an angiogram is utilized to access the arteries and veins that are included with vasculitis. Through an angiogram, a straw-based flexible tube is inoculated into a large artery or vein and a particular dye is inoculated. X-rays are then performed as the dye seals the blood vessels and exhibits any part of infection. Many people with vasculitis are cured by their initial care physician or an expert in the field of rheumatology. These physicians have the knowledge to offer one with a complete method to cure the Vasculitis. The main benefits of curing vasculitis is the choice to put the disorder into remission, which states that one will not have any lively prodromes of the vasculitis. This is usually probable in many cases of the varied kinds of vasculitis and can be truly essential for an individual’s standard of life. Keeping the disorder in remission is important as it decreases the threat of relapse and side-effects such as organ destruction. It also states that one can survive a persistent and jovial life as one is very capable to enjoy the objects one love and spend time with family and relatives. One will require to follow a therapy procedure with the physician and one should observe the illness for any complications of drugs. The most usually utilized medicine for the Vasculitis Treatment comprise glucocorticoids, such as prednisone and another drug to manage infection, such as methotrexate, azathioprine, mycophenolate, cyclophosphamide or tocilizumab. The physician might also suggest other therapies to aid regulate the infection and inhibit destruction to the body’s organs. If one have an artery in the body that has become destructed owing to vasculitis, one might require undergo an operation to transmit blood flow over it. Having a better assistive network, being fit and hygienic and understanding the problems are all supportive in sustaining the wellbeing and assisting one to survive better with vasculitis. It is important to have a better communication and interaction with the physician and keep up with the clinical visits, so that one can ensure that the well-being is being taken care of. While there's no cure, Rheumatoid Arthritis Treatment, such as physiotherapy and medication, can help slow the disease's progression. Most cases can be managed with a class of medications called anti-rheumatic drugs (DMARDS). Rheumatoid arthritis (RA) is an autoimmune disease in which body's immune system attacks the lining of the membranes that surround the joints. It's not quite understood why the immune system does this. It is caused by the immune system attacking healthy body tissue. However, it's not yet known what triggers this. The immune system normally makes antibodies that attack bacteria and viruses, helping to fight infection. Methotrexate is usually the first drug given for rheumatoid arthritis, often with another DMARD and a short course of steroids (corticosteroids) to relieve any pain. These may be combined with biological treatments. Methotrexate is the group of drugs called disease‐modifying antirheumatic drugs (DMARDs) and is the most common Rheumatoid Arthritis Treatment. Methotrexate helps prevent further permanent damage that can happen if it is not treated. Methotrexate is regarded as one of the safest of all arthritis drugs, though it carries some potential downsides. Gastrointestinal symptoms such as nausea and vomiting are its most frequent side effects. Common side effects of methotrexate include feeling sick, loss of appetite, sore mouth, diarrhoea, headaches, and hair loss, among others. Moreover, Leflunomide (Arava) is drug approved to treat adult moderate to severe Rheumatoid Arthritis along with other rheumatic diseases. It belongs to a class of drugs called DMARDs, which aim to decrease inflammation and permanent damage. It is a medication used in the management and treatment of rheumatoid arthritis. Leflunomide is used alone or in combination with other medications. Side effects and risks include, feeling sick, mouth ulcers, weight loss, stomach pain, tiredness, headaches, dizziness, and weakness. Hydroxychloroquine (Plaquenil) also belongs to a class of drugs called DMARDs. It can decrease the pain and swelling of arthritis. It may prevent joint damage and reduce the risk of long-term disability. It is used to treat rheumatoid arthritis and lupus. It is relatively safe and well-tolerated agent for the Rheumatoid Arthritis Treatment. While, Sulfasalazine (which also belongs to a class of drugs called DMARDs.) is indicated for the treatment of chronic inflammatory diseases such as rheumatoid arthritis in children and adults. Sulfasalazine is used for rheumatoid arthritis, psoriatic arthritis, and arthritis associated with bowel inflammation. Sulfasalazine (Azulfidine) can decrease pain and swelling of arthritis, prevent joint damage, and reduce the risk of long-term disability. But clinical studies indicate that remission of symptoms is more likely when treatment begins early with drugs known as disease-modifying antirheumatic drugs (DMARDs). To help manage pain and inflammation from a Rheumatoid Arthritis flare-up, one can take over-the-counter (OTC) pain relievers and anti-inflammatory drugs such as naproxen, ibuprofen, or acetaminophen. A doctor may also prescribe a steroid treatment or injection for more severe symptoms. Early treatment and support (drugs, lifestyle changes, supportive Rheumatoid Arthritis Treatment, and surgery) can reduce the risk of joint damage and limit the impact of the condition. Explore more about Rheumatoid Arthritis Treatment - https://tamildada.info/what-are-the-various-possible-rheumatoid-arthritis-treatment-available-today/ Malaria is a deadly disease that kills over 400,000 people a year, mostly children. Mutating parasites and growing resistance to drugs and insecticides have stalled progress toward a malaria-free world. The World Health Organization has endorsed the first-ever malaria vaccine, RTS, S/AS01. It is the result of 30 years of research and development by GSK, PATH, and partners. A Malaria Vaccines are the medicine that reduces the risk of contracting malaria. It can be administered to people living in endemic areas of the world or traveling there. Several different types of malaria vaccines are currently being developed for malaria. One type, called a circumsporozoite vaccine (CSV), directs immune responses against the major circumsporozoite protein covering the surface of infecting sporozoites. Another type of Malaria Vaccine, called a pre-erythrocytic vaccine, targets the first stage of the parasite’s life cycle by intercepting sporozoites before they get to the liver. A third type of vaccine, called a transmission-blocking vaccine, prevents the formation of new gametes in an infected host. These are the reproductive cells of the parasite that can be ingested by a mosquito and initiate infection. The safety of a malaria vaccine is largely dependent on the nature of the parasite. Many different genetic variants of the Plasmodium falciparum parasite exist in Africa, and so any new vaccine must be effective against a broad range of these. One approach to malaria vaccine development is to target merozoites during the blood phase of their life cycle. This could be done by using antibodies against a merozoite's surface or by blocking its invasion of red blood cells. But a more promising approach is to target the parasite directly through the immune system. This is a more complex task, and many possible strategies can be used to do so. The RTS, S/AS01E malaria vaccine developed by GSK has been tested in a pilot program and has proven safe and effective in infants. It is a feasible product that can be delivered in settings with routine immunization systems and that increases equity in access to prevention. Malaria is one of the world's deadliest diseases: it kills hundreds of millions of people each year, and many of them are children. Many things can be done to combat the disease, but one of the most promising is a vaccine. However, developing a malaria vaccine requires decades of research. The CDC is working on an experimental vaccine, called R21. The Malaria Vaccine is being tested in 450 children living in Burkina Faso, a country that has high seasonal malaria infections. The vaccine's efficacy was 80% in the trial, but it is important to note that this result is based on data from a very small number of people. Although the vaccine is effective, it also has a high dose that can cause a child to have low hemoglobin levels. This can affect the immune system and cause serious health problems. Malaria Vaccines work by stimulating an immune response against a target. In malaria, this immune response may prevent infection by the parasite. It also may help reduce the symptoms of the disease and/or its effects on human health, such as fever, headache, and joint pain. Diabetes is a chronic metabolic disease characterized by high levels of blood sugar. It can lead to a wide range of complications, including Diabetic Neuropathy. Diabetic neuropathy is a type of nerve damage that can occur in people with diabetes. It is a common complication of diabetes that affects the peripheral nerves, which are the nerves that transmit signals between the central nervous system and the rest of the body. Diabetic Neuropathy can affect different parts of the body, including the feet, legs, hands, arms, and internal organs such as the digestive system, urinary tract, and cardiovascular system. The severity of diabetic neuropathy can vary widely from person to person. Some people may experience mild symptoms, while others may have severe and debilitating symptoms that affect their quality of life. The exact cause of Diabetic Neuropathy is not well understood. However, researchers believe that high blood sugar levels over a prolonged period can cause damage to the nerves. High levels of blood sugar can damage the blood vessels that supply the nerves, leading to decreased blood flow and oxygen to the nerves. This can cause the nerves to malfunction, leading to symptoms of diabetic neuropathy. Symptoms of diabetic neuropathy can vary depending on which nerves are affected. Some common symptoms include:
Diabetic Neuropathy can be classified into several different types, depending on which nerves are affected. Some common types of diabetic neuropathy include:
Diagnosis of Diabetic Neuropathy typically involves a physical exam and a review of symptoms. A doctor may also perform tests to assess nerve function, such as nerve conduction studies or electromyography (EMG). Blood tests to measure blood sugar levels and other tests, such as ultrasound or magnetic resonance imaging (MRI), may also be performed to help diagnose diabetic neuropathy. Treatment of diabetic neuropathy typically involves managing symptoms and controlling blood sugar levels. Medications may be used to manage pain, such as antidepressants or anticonvulsants. In severe cases, opioids may be prescribed. Physical therapy, occupational therapy, or other forms of rehabilitation may also be recommended to improve mobility and function. Lifestyle changes are also an important part of managing Diabetic Neuropathy. Maintaining a healthy diet, exercising regularly, and quitting smoking can help control blood sugar levels and reduce the risk of complications. An abnormal heart rhythm (arrhythmia) known as Atrial Fibrillation (AF or A-fib) is defined by the rapid and erratic beating of the atrial chambers of the heart. Little bouts of aberrant beating are frequently the first to appear, and over time, they often grow longer or never stop. It might also begin as another type of arrhythmia, like atrial flutter, before changing into AF. Episodes could not show any symptoms. Heart palpitations, dizziness, lightheadedness, shortness of breath, and chest pain are examples of symptomatic episodes. Heart failure, dementia, and stroke risk are all elevated by atrial fibrillation. Supraventricular tachycardia of this kind. Atrial Fibrillation (AFib) is a type of cardiac arrhythmia characterized by irregular and often rapid heartbeats. It is the most common type of arrhythmia, and its prevalence increases with age. Atrial fibrillation can lead to various complications, including stroke, heart failure, and cognitive impairment. In this article, we will discuss the causes, symptoms, diagnosis, treatment, and prevention of atrial fibrillation. Causes The exact cause of atrial fibrillation is not always known, but certain factors can increase the risk of developing this condition. Some of these factors include:
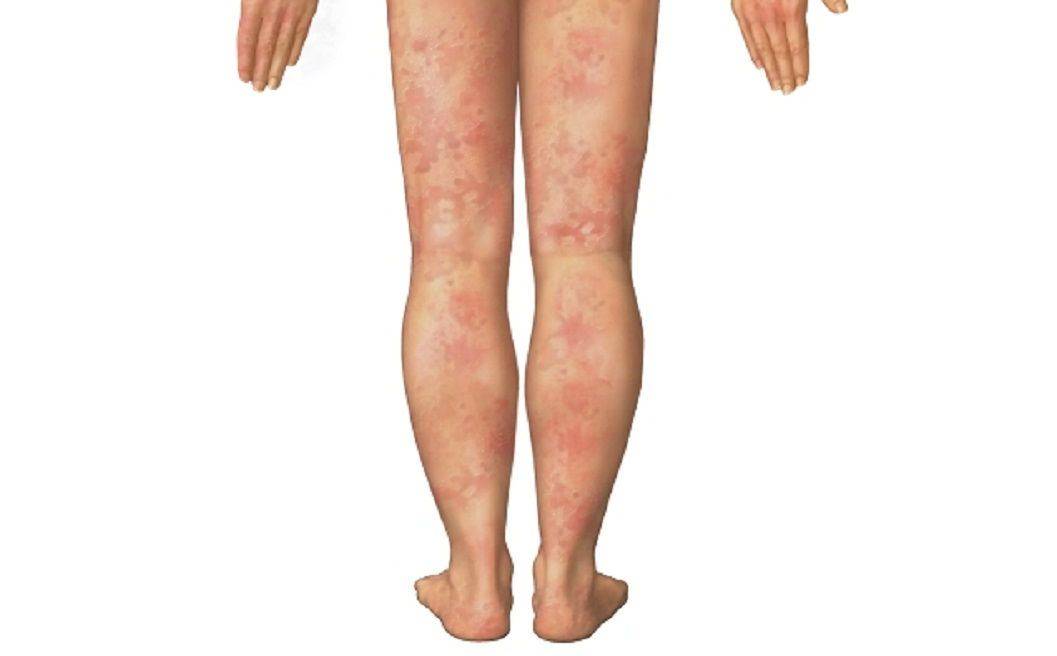
The most frequent modifiable risk factors for Atrial Fibrillation are high blood pressure and valvular heart disease. Heart failure, coronary artery disease, cardiomyopathy, and congenital heart disease are other heart-related risk factors. Rheumatic fever is frequently to blame for valvular heart disease in low- and middle-income nations. The risk factors for lung disease include obesity, COPD, and sleep apnea. The use of excessive amounts of alcohol, smoking, diabetes, and thyrotoxicosis are additional risk factors. However, none of the aforementioned dangers are present in around 50% of cases. After feeling the pulse, medical experts may suspect Atrial Fibrillation and confirm the diagnosis by reading an electrocardiogram (ECG). An ECG indicative of AF displays P waves but with unevenly spaced QRS complexes. Reduced alcohol use, greater physical activity, and weight loss in obese individuals are just a few healthy lifestyle modifications that can lower the incidence of atrial fibrillation and lessen its effects if it does occur. AF is frequently managed using drugs that either reduce the heart rate to a range that is close to normal (rate control) or change the rhythm to normal sinus rhythm (known as rhythm control). When a person is unstable, electrical cardioversion, which can return AF to a normal heart rhythm, is frequently required. Some people's recurrences may be prevented with ablation. Blood-thinning medications are not always necessary for people with Atrial Fibrillation who have a low risk of stroke, though some medical professionals may recommend aspirin or an anti-clotting drug. Experts typically advise taking an anti-clotting medicine for people at higher than low risk. Warfarin and other direct oral anticoagulants are examples of anticoagulant medicines. Stroke risk is increased for the majority of persons. These drugs lower the risk of stroke but raise the incidence of serious bleeding. The Opioids Class Of Drug Is Prescribed By Healthcare Providers To Manage Moderate To Severe Pain17/2/2023 Opioids are a class of drugs that act on the nervous system to produce pain relief and a sense of euphoria. They are derived from the opium poppy plant or are synthetically produced, and they are commonly prescribed for the management of moderate to severe pain. Opioids work by binding to receptors in the brain and other parts of the body, mimicking the effects of endorphins, the body's natural pain relievers. Opioids can be broadly categorized into three groups: natural opioids, semi-synthetic opioids, and synthetic opioids. Natural opioids are derived directly from the opium poppy plant, and include drugs such as morphine and codeine. Semi-synthetic opioids are derived from natural opioids and include drugs such as oxycodone, hydrocodone, and hydromorphone. Synthetic opioids, such as fentanyl, are entirely man-made. While Opioids can be highly effective in relieving pain, they also have a high potential for abuse and addiction. When taken in large doses or for a prolonged period of time, opioids can produce a range of adverse effects, including respiratory depression, constipation, nausea, drowsiness, and cognitive impairment. In extreme cases, opioid overdose can be fatal. Despite these risks, opioid use has become increasingly common in recent years, with many people using prescription opioids for non-medical purposes or turning to illicit opioids such as heroin. This has led to a major public health crisis, with opioid-related overdose deaths reaching record highs in many parts of the world. One of the reasons for the rise in Opioid use and abuse is the over-prescription of opioid painkillers by healthcare providers. In many cases, opioids are prescribed for conditions such as chronic pain that may be better managed with alternative treatments. In addition, patients may become dependent on opioids after taking them for an extended period, even when they are no longer needed for pain relief. Another factor contributing to the opioid crisis is the availability of illicit opioids, such as heroin and fentanyl. These drugs are often much cheaper and more accessible than prescription opioids, making them an attractive option for those who are struggling with addiction. Efforts to address the Opioid crisis have included a range of strategies, such as increasing access to addiction treatment, promoting the use of non-opioid pain management options, and limiting the prescription of opioids for non-cancer pain. In addition, many countries have implemented programs to increase access to naloxone, a medication that can reverse the effects of an opioid overdose and save lives. Despite these efforts, the opioid crisis remains a major public health challenge, with tens of thousands of people dying from opioid-related overdoses every year. To address this crisis, it is important to continue exploring alternative treatments for pain management, promoting safe prescribing practices, and expanding access to addiction treatment and harm reduction services. For More details, Visit https://www.prnewswire.com/news-releases/global-opioids-market-to-surpass-us-52-732-million-by-2028--says-coherent-market-insights-301466399.html The majority of Vasculitis types have unknown origins. Several genes appear to play a little role in the disease due to genetic variables. Vasculitis is considered to be an autoimmune condition, meaning the body is attacked by its own immune system. The immune system attacks blood vessels in vasculitis. Drug responses can lead to vasculitis in some situations. Vasculitis can also be brought on by some chronic (long-term) infections, such as those with the hepatitis C or hepatitis B virus. Vasculitis can occur in conjunction with other rheumatic disorders, most notably Sjögren's syndrome, rheumatoid arthritis, and systemic lupus erythematosus. Most vasculitis sufferers don't have any of these conditions. Vasculitis can cause inadequate blood flow to several body tissues, including the lungs, nerves, and skin. As a result, vasculitis can manifest in a broad variety of ways, including:
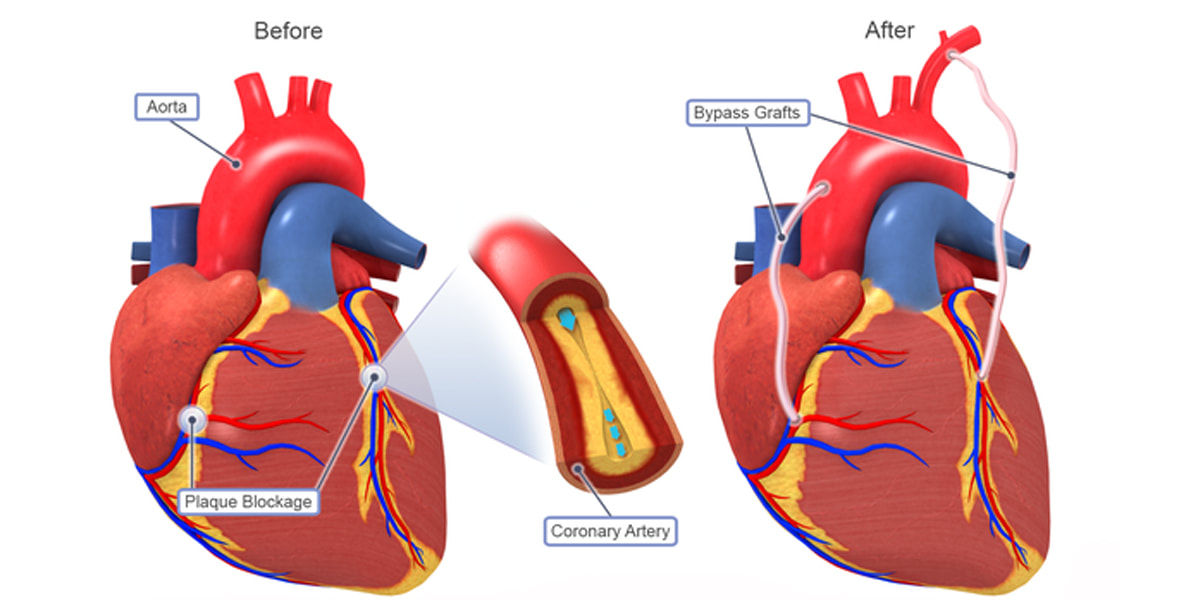
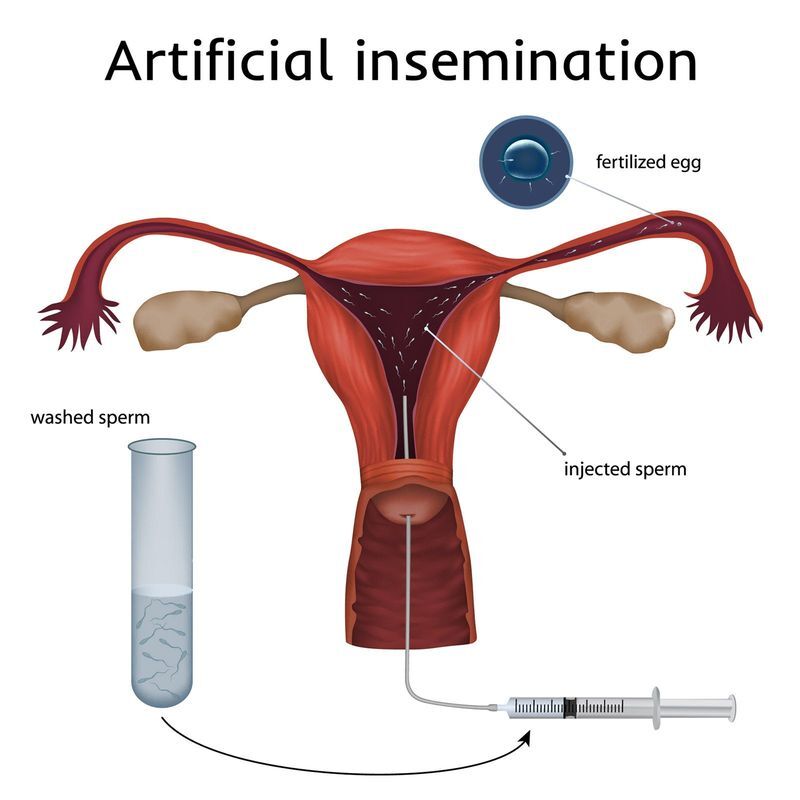
On the other hand, renal vasculitis may not initially manifest any symptoms but is still a major issue. Vasculitis can be moderate, incapacitating, or even fatal. Individuals may only experience one bout of vasculitis or they may experience multiple episodes over several years. The majority of Vasculitis Treatment are done with glucocorticoids, also known as "steroids" (prednisone, prednisolone, or others). The severity of the condition and the length of the patient's illness determine the dosage and duration of the treatment. Some medications can have long-term negative effects even when they lessen inflammation. Immunosuppressive medications are occasionally used by doctors because they may have less severe long-term negative effects than glucocorticoids. This type of Vasculitis Treatment is known as "steroid-sparing." When a serious illness puts crucial organs in jeopardy, doctors may administer cyclophosphamide, one of these medications with the highest potency. Patients may be given methotrexate, azathioprine, or other immune-suppressing medications for less severe vasculitis. These medications are frequently prescribed by doctors to treat various rheumatic disorders, but they are also effective for vasculitis. Vasculitis may benefit from the use of more recent biologic medications made for other autoimmune and inflammatory illnesses. Researchers discovered that rituximab (Rituxan), one of these medications, efficiently manages severe cases of specific types of vasculitis. They include cryoglobulinemic vasculitis, microscopic polyangiitis, and granulomatosis with polyangiitis. Tocilizumab (Actemra), which treats giant cell arteritis, and mepolizumab (Nucala), which treats eosinophilic granulomatosis with polyangiitis, are further biologic medications that have been approved to treat various kinds of vasculitis. Avacopan (Tavneos), a more recent Vasculitis Treatment option for ANCA-related vasculitis, has received FDA approval. The most severe forms of these disorders may require plasmapheresis or intravenous immunoglobulin therapy, also known as "IVIG." Sometimes surgery is necessary to repair damage from severe vasculitis. There may be vascular bypass grafting involved (a surgery to redirect blood flow around a blockage in a blood vessel). Other possible procedures include a kidney transplant or sinus surgery, depending on the location of the damage. The goal of Artificial Insemination is to transport sperm to a woman's cervix or uterus without the use of sexual contact. The American Pregnancy Association lists two primary artificial insemination techniques: intrauterine insemination (IUI), which is a fertility treatment done in a doctor's office where specially prepared semen is inserted into a patient's uterus, and intracervical insemination (ICI), which is typically performed at home with a needleless syringe. Artificial Insemination (AI) is a fertility treatment that involves the deliberate introduction of sperm into a female's reproductive tract, outside of sexual intercourse, with the goal of achieving pregnancy. According to the American College of Obstetricians and Gynecologists (ACOG), if you're under 35 years old and have been trying to conceive for 12 months, or if you're over 35 and have been attempting to conceive for six months, you might want to get advice from a fertility specialist. It's normally ideal to first undergo a fertility workup, which consists of a series of blood tests and ultrasounds that look at your ovarian reserve, uterine shape, tubal shapes, hormone levels, and your partner's sperm. This procedure is quite simple, painless, and can be financially feasible. There are several methods of AI, including:
AI can be performed using sperm from a male partner or donor. The sperm is washed, concentrated and prepared for the procedure. In some cases, the sperm may be frozen for later use. The procedure is performed using a sterile, flexible catheter. AI can be used to treat infertility caused by a variety of factors, including male infertility, cervical mucus issues, endometriosis, and unexplained infertility. It can also be used as an alternative to sexual intercourse in couples who are unable to have sex due to physical or psychological reasons. The success rate of AI varies and depends on several factors, including the cause of infertility, the woman's age, and the quality of the sperm used. In general, the success rate is around 10-20% per cycle. AI is a relatively safe and non-invasive procedure. The most common side effects are mild cramping and discomfort during and after the procedure. In rare cases, infection or bleeding may occur. AI is typically covered by insurance in the United States if it is performed for medical reasons. However, coverage for AI using donor sperm is usually not covered by insurance. Artificial Insemination is a fertility treatment that involves introducing sperm into a female's reproductive tract in order to achieve pregnancy. It is a safe and non-invasive procedure that can be used to treat infertility caused by a variety of factors. The success rate of AI varies and depends on several factors, including the cause of infertility and the quality of the sperm used. Oral Care is very important in preserving dental health, avoiding gum disease (gum infection), and maintaining gums (forging). Oral hygiene also plays a part in maintaining good oral health by minimizing the risk of gum disease and promoting good oral health. Oral care involves cleaning, examination, and the selection of recommended therapies and restorative procedures for restoring and/or enhancing oral health. Oral cancer is a common oral cancer type and treatment includes the surgical removal of the tumor and radiation therapy. Oral cancer is cancer that develops in the tissues surrounding the tooth and in the jawbone or pulp. The oral cavity is the space occupied by the teeth. The oral cavity also includes the supporting structures including the dentures and the oral pockets. A small area of the tissue termed the periodontium surrounds the teeth and forms a part of the root system of the tooth. The most common types of oral cavity cancers are in the epithelial layer of the teeth, in the middle layer of the tooth, or in the periapical region. Risk factors for this disease include chronic inflammation of the gums, malignancy, or diabetes and women. Factors that affect the risk factors for this disease include poorly controlled blood pressure, smoking, poor nutritional quality, inadequate fluoride intake, prolonged use of tobacco products, and multiple dental surgeries. Other risk factors of Oral Care include prolonged exposure to radiation, alcohol abuse, and pregnancy. Other preventive measures against the occurrence of oral care problems include daily brushing of teeth, routine dental checkups and examination of the oral cavity, regular use of antiseptics and fluoride, regular cleaning of the teeth and tongue, and routine medical checkups. Oral Care is very important. The first aspect is the diagnosis of periodontal disease. The second aspect is the assessment of the severity or prevalence of periodontal disease using a checklist developed by the American Dental Association (ADA). The third aspect is the management of periodontitis. The fourth aspect is the control of complications arising from untreated periodontitis. Oral Care is the process of maintaining one's mouth free from disease and illness by regularly brushing the teeth and cleaning even between the teeth with a toothbrush and a fluoride mouth rinse. One must not forget that a proper intake of fluoride has been proven to reduce the risks of getting cavities, periodontal diseases, and gum diseases. It is advisable that oral care be done regularly to allow the prevention of various dental diseases and bad breath in adults. The process of saliva production plays an important role in controlling the growth of plaque and bacteria in between teeth. Regularly brushing the teeth with a toothbrush that produces high-quality saliva may eliminate most of the plaque and bacteria that develop in between teeth. Some people with chronic periodontal diseases are required to visit their dentists more often as plaque and bacteria grow more quickly in people with poor oral health care. Oral Care is a vital aspect of nursing. Poor oral hygiene can have a negative impact on a patient's general health and well-being. The definition of oral hygiene is cleaning the mouth, which includes the teeth, gums, tongue, lips, and dentures. As a result, it is essential for the health of a hospitalized patient. Poor oral hygiene habit can affect their quality of life, reduce their intake of nutrients, and increase their risk for infection and gum disease. |
Categories
All
|